Diagnosis
To diagnose your condition, your doctor will review your signs and symptoms, and your medical history. Your doctor will also perform a physical examination.
Your doctor may ask your partner some questions about when and how you snore to help assess the severity of the problem. If your child snores, you'll be asked about the severity of your child's snoring.
Imaging
Your doctor may request an imaging test, such as an X-ray, a computerized tomography scan or magnetic resonance imaging. These tests check the structure of your airway for problems, such as a deviated septum.
Sleep study
Depending on the severity of your snoring and other symptoms, your doctor may want to conduct a sleep study. Sleep studies may sometimes be done at home.
However, depending upon your other medical problems and other sleep symptoms, you may need to stay overnight at a sleep center to undergo an in-depth analysis of your breathing during sleep by a study, called a polysomnography.
In a polysomnography, you're connected to many sensors and observed overnight. During the sleep study, the following information is recorded:
- Brain waves
- Blood oxygen level
- Heart rate
- Breathing rate
- Sleep stages
- Eye and leg movements
More Information
Treatment
Continuous positive airway pressure (CPAP)
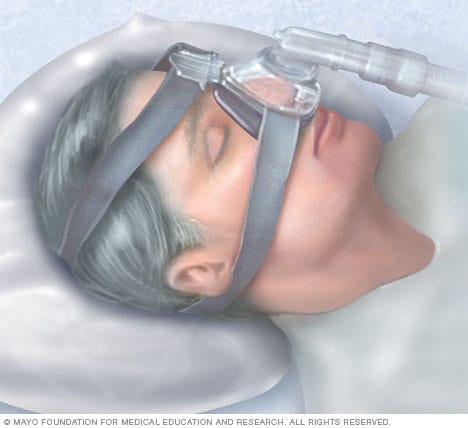
Continuous positive airway pressure (CPAP)
To eliminate snoring and prevent sleep apnea, a healthcare professional may recommend a device called a continuous positive airway pressure (CPAP) machine. A CPAP machine delivers just enough air pressure to a mask to keep the upper airway passages open, preventing snoring and sleep apnea.
To treat your snoring, your doctor likely will first recommend lifestyle changes, such as:
- Losing weight
- Avoiding alcohol close to bedtime
- Treating nasal congestion
- Avoiding sleep deprivation
- Avoiding sleeping on your back
For snoring accompanied by OSA, your doctor may suggest:
-
Oral appliances. Oral appliances are form-fitting dental mouthpieces that help advance the position of your jaw, tongue and soft palate to keep your air passage open.
If you choose to use an oral appliance, you'll work with your dental specialist to optimize the fit and position of the appliance. You'll also work with your sleep specialist to make sure the oral appliance is working as intended. Dental visits may be necessary at least once every six months during the first year, and then at least annually after that, to have the fit checked and to assess your oral health.
Excessive salivation, dry mouth, jaw pain and facial discomfort are possible side effects from wearing these devices.
-
Continuous positive airway pressure (CPAP). This approach involves wearing a mask over your nose or mouth while you sleep. The mask directs pressurized air from a small bedside pump to your airway to keep it open during sleep.
CPAP (SEE-pap) eliminates snoring and is most often used to treating snoring when associated with OSA.
Although CPAP is the most reliable and effective method of treating OSA, some people find it uncomfortable or have trouble adjusting to the noise or feel of the machine.
-
Upper airway surgery. There are a number of procedures that seek to open the upper airway and prevent significant narrowing during sleep through a variety of techniques.
For example, in a procedure called uvulopalatopharyngoplasty (UPPP), you're given general anesthetics and your surgeon tightens and trims excess tissues from your throat — a type of face-lift for your throat. Another procedure called maxillomandibular advancement (MMA) involves moving the upper and lower jaws forward, which helps open the airway. Radiofrequency tissue ablation employs a low-intensity radiofrequency signal to shrink tissue in the soft palate, tongue or nose.
A newer surgical technique called hypoglossal nerve stimulation employs a stimulus applied to the nerve that controls forward movement of the tongue so the tongue does not block the airway when you take a breath.
The effectiveness of these surgeries varies and the response can be challenging to predict.
Lifestyle and home remedies
To prevent or quiet snoring, try these tips:
- If you're overweight, lose weight. People who are overweight may have extra tissues in the throat that contribute to snoring. Losing weight can help reduce snoring.
- Sleep on your side. Lying on your back allows your tongue to fall backward into your throat, narrowing your airway and partially obstructing airflow. Try sleeping on your side. If you find that you always end up on your back in the middle of the night, try sewing a tennis ball in the back of your pajama top.
- Raise the head of your bed. Raising the head of your bed by about 4 inches may help.
- Nasal strips or an external nasal dilator. Adhesive strips applied to the bridge of the nose help many people increase the area of their nasal passage, enhancing their breathing. A nasal dilator is a stiffened adhesive strip applied externally across the nostrils that may help decrease airflow resistance so you breathe easier. Nasal strips and external nasal dilators aren't effective for people with OSA, however.
-
Treat nasal congestion or obstruction. Having allergies or a deviated septum can limit airflow through your nose. This forces you to breathe through your mouth, increasing the likelihood of snoring.
Ask your doctor about a prescription steroid spray if you have chronic congestion. To correct a structural defect in your airway, such as a deviated septum, you may need surgery.
- Limit or avoid alcohol and sedatives. Avoid drinking alcoholic beverages at least two hours before bedtime, and let your doctor know about your snoring before taking sedatives. Sedatives and alcohol depress your central nervous system, causing excessive relaxation of muscles, including the tissues in your throat.
- Quit smoking. Smoking cessation may reduce snoring, in addition to having numerous other health benefits.
- Get enough sleep. Adults should aim for at least seven hours of sleep per night. The recommended hours of sleep for children vary by age. Preschool-aged children should get 10 to 13 hours a day. School-age children need nine to 12 hours a day, and teens should have eight to 10 hours a day.
Alternative medicine
Because snoring is such a common problem, there are numerous products available, such as nasal sprays or homeopathic therapies. However, most of the products haven't been proved effective in clinical trials.
Coping and support
If your partner is the one who's snoring, you may sometimes feel frustrated as well as fatigued. Suggest some of the home remedies mentioned, and if those don't help quiet your partner's nocturnal noisemaking, have your partner make a doctor's appointment.
In the meantime, ear plugs or background noise, such as a white noise machine or a fan near the bed, may help mask snoring noise so you get more sleep.
Preparing for your appointment
You're likely to first see your family doctor or a general practitioner. However, you may then be referred to a doctor who specializes in treating sleep disorders.
Because appointments can be brief, and because there's often a lot to talk about, it's a good idea to arrive well-prepared. Here's some information to help you get ready for your appointment, and what to expect from your doctor.
What you can do
-
Write down any symptoms you're experiencing, including any that may seem unrelated to the reason for which you scheduled the appointment. Ask your partner to describe what he or she hears or notices at night while you're sleeping.
Or, better yet, ask your sleep partner to go with you to your appointment so that he or she can talk with your doctor about your symptoms.
- Make a list of all medications, as well as any vitamins or supplements that you're taking.
- Write down questions to ask your doctor.
Your time with your doctor may be limited, so preparing a list of questions can help you make the most of your time together. For snoring, some basic questions to ask your doctor include:
- What makes me snore when I sleep?
- Is my snoring a sign of something more serious, such as OSA?
- What kinds of tests do I need?
- What happens during a sleep test?
- What treatments are available for snoring, and which do you recommend?
- What types of side effects can I expect from treatment?
- Are there any alternatives to the primary approach that you're suggesting?
- Are there any steps I can take on my own that will help my snoring?
- I have other health conditions. How can I best manage these conditions together?
- Are there any brochures or other printed material that I can take home with me? What websites do you recommend visiting?
In addition to the questions that you've prepared to ask your doctor, don't hesitate to ask questions during your appointment.
What to expect from your doctor
Your doctor is likely to ask you a number of questions. Being ready to answer them may reserve time to go over any points you want to spend more time on. Your doctor may ask:
- When did you first begin snoring?
- Do you snore every night or only once in a while?
- Do you often wake up during the night?
- Does anything you do seem to improve your snoring?
- What, if anything, appears to worsen your snoring?
- Does your snoring depend on specific positions of sleep?
- How loud is your snoring? Does it bother your bed partner? Can it be heard outside the bedroom?
- Does your bed partner ever tell you that you have pauses or irregularities in your breathing during sleep?
- Do you snort, choke or gasp yourself awake from sleep?
- What daytime symptoms are you experiencing, such as sleepiness?
What you can do in the meantime
While you're waiting to see your doctor, here are some tips you can try:
- Don't drink alcohol or take sedatives before bed.
- Try over-the-counter nasal strips.
- Sleep on your side, instead of your back.
- If nasal congestion is an issue, try an over-the-counter decongestant for a day or two.
Dec. 22, 2017