March 27, 2020
Mayo Clinic is one of the few centers that uses free vascularized fibula grafts (FVFGs) for reconstruction after tumor resection in the spine and pelvis. Surgical teams that include orthopedic oncology surgeons as well as hand and plastic surgeons have performed more than 60 of these complex procedures, with generally favorable outcomes.
"We have achieved a union of the spine and pelvis in more than 90% of these patients," says Peter S. Rose, M.D., an orthopedic surgeon at Mayo Clinic in Rochester, Minnesota. "It's a long and complex procedure, but it's very well suited for patients who are undergoing a curative tumor resection — particularly patients with a strong potential for long life expectancy. They need a durable reconstruction, and the vascularized graft provides healing potential."
Reconstruction of the spine after tumor resection frequently requires surgeons to address large osseous defects and compromised bone healing due to radiation and chemotherapy. In the treatment of lower spinal and sacral tumors, resection often disrupts continuity between the spine and pelvis, resulting in severe biomechanical disadvantages, including the inability to transfer the load of the body to the lower extremities.
Although FVFG transfer has long been performed successfully for lower extremity reconstruction, the procedure's use in the spine and pelvis has been limited. Mayo Clinic's approach uses an FVFG alone or in combination with a structural allograft or reconstruction cage.
طعم الشظية الوعائية مزدوج الطبقات في إعادة بناء العمود الفقري
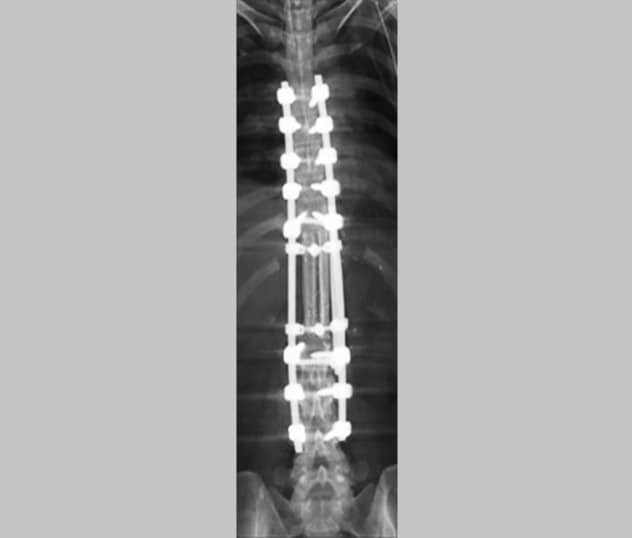
طعم الشظية الوعائية مزدوج الطبقات في إعادة بناء العمود الفقري
تُظهر الأشعة السينية استخدام طعم الشظية الوعائية مزدوج الطبقات في إعادة بناء العمود الفقري.
When used alone, the FVFG is sometimes cut and layered to make it more robust. "We double-barrel or even triple-barrel configurations to increase the strength of the vascularized graft," Dr. Rose says.
Combining an FVFG with an allograft provides even greater bulk, as well as the capacity for osteogenesis. "Putting the two together works very well when we have to cut the side of the femur, for example," Dr. Rose says. "We need something that can bear the patient's whole weight after surgery. But if we use an allograft alone, the patient has difficulty healing and is prone to develop stress fractures over time. As a living bone, the fibula graft has much greater healing potential and can promote healing of a stress fracture if that happens."
The advantages of vascularized bone transfer are particularly noteworthy in the setting of radiotherapy. Mayo Clinic's treatment protocol for many cases of spinal tumor involves proton beam or other high-dose radiation therapies.
"These radiotherapies have very good efficacy for treating the cancer but are highly damaging to bone," Dr. Rose says. "The docking sites for the graft are irradiated, which compromises the graft's ability to heal. A vascularized bone transfer helps us overcome that problem."
Mayo Clinic has also demonstrated favorable results with the use of FVFGs for pediatric limb salvage. In a study published in the October 2018 issue of Plastic and Reconstructive Surgery, Mayo Clinic researchers found that FVFG supplementation reduced the risk of allograft revision for children undergoing lower extremity reconstruction.
The researchers compared the outcomes of 29 pediatric patients who had lower extremity limb salvage using intercalary cadaveric allografts. Eleven patients had reconstruction using allografts alone; 18 had allografts supplemented with FVFGs. Three patients subsequently required allograft revision because of fracture or fracture and infection. However, none of those three allografts had FVFG supplementation.
"Some of the patients in this study had to have a secondary bone graft procedure. But we ultimately achieved union in nearly every one of these children," Dr. Rose says.
Mayo Clinic's extensive experience with vascularized bone transfers has allowed its surgeons to apply the procedure to other musculoskeletal areas. "Major resections of the spine are relatively uncommon," Dr. Rose says. "These long and complex procedures require a big team. At Mayo it's never about a single individual — it's always what can be done with the team."
For more information
Houdek MT, et al. Comparison of pediatric intercalary allograft reconstructions with and without a free vascularized fibula. Plastic and Reconstructive Surgery. 2018;142:1065.