Sept. 23, 2022
Krystin A. Hidden, M.D., an orthopedic surgeon at Mayo Clinic's campus in Rochester, Minnesota, is passionate about nonunion repair, which is when a surgically repaired fracture from trauma never heals. Patients often come to see her or her colleagues because they are symptomatic despite surgical fracture repair months previously, experiencing persistent pain where the extremity is typically stable. In other cases, patients experience hardware failure: If the bone has not healed, the hardware may begin to break.
"It's a race between the bone healing and the implant failing. If I see hardware shifting, I have a high suspicion for nonunion," says Dr. Hidden.
While studying a patient's case, she asks these questions:
- Biomechanics. Were appropriate implants and hardware used in the previous surgery? Are the current implants accomplishing what the injury requires?
- Biology. Is the necessary biology present to achieve complete healing? Is there a large incision with significant tissue stripping?
- Infection. Are any infection signs present?
- Stability. Is the bone stable with the current hardware?
- Bone loss. Is there bone loss? Is a bone graft needed from a different body part or from a deceased donor? Would the bone need a 3D-printed allograft?
- Nutrition and hormones. Is the patient deficient in calcium or vitamin D? Are any hormones working improperly?
- Polytrauma. Did the patient experience additional injuries, multiplying the total healing time needed?
- Nature of injury. Where and how did the fracture occur? Was it a high-energy injury? Did it result in an atypical femur fracture? An open injury with protruding bone?
Determining risk factors prior to nonunion surgery
Beyond considering these aspects of the case, Dr. Hidden ascertains any risk factors that may impact nonunion repair outcome, such as:
- Diabetes
- Tobacco smoking status
- Immune-modulating agents or medications
- Morbid obesity
- Peripheral neuropathy
Dr. Hidden and colleagues collaborate with patients with these risk factors to help them achieve the biology necessary for successful nonunion repair. For patients with diabetes, she partners with Mayo Clinic endocrinologists, who help patients control their glycated hemoglobin (hemoglobin A1C), targeting a range of 5.6 to 6 or lower. Dr. Hidden refers patients who smoke tobacco to a smoking cessation program. Successful nonunion repair requires tobacco-free status, as any nicotine in the system impacts blood vessel diameter and decreases healing.
Dr. Hidden states, "It's hard to fill a swimming pool with a water hose. Nicotine decreases blood vessel diameter, which in turn can't deliver the nutrients required for successful healing."
Immune-modulating agents can produce inadequate healing responses, especially in the setting of chronic steroids, antirheumatic medications, radiation or chemotherapy. She discusses elevated nonunion surgical risk with patients with morbid obesity, including increased infection risk and wound-healing issues. She refers these patients, if they elect to proceed, to Mayo Clinic weight-loss experts for guidance in lowering body mass index (BMI) prior to surgery.
An orthopedic surgeon also must rule out infection before nonunion repair. If present, at least two procedures are usually necessary to clear the infection. "If the skin or limb is at risk, it swings the pendulum toward more-emergent surgery," says Dr. Hidden.
She feels working with patients pre-surgically on modifiable risk factors is a key part of her role in their treatment. Tobacco is one such modifiable risk factor. She recognizes smoking cessation is a challenge.
Ultimately, however, she collaborates with the patients needing nonunion surgery to weigh the risks and benefits to determine if the surgery will be safe and effective.
"I would not recommend nonunion surgery if it would harm the patient or not improve the quality of life," says Dr. Hidden.
In some cases, nonunions may be treated without surgery. She indicates that correcting deficient levels of vitamin D and calcium could prevent the need for nonunion surgery at all. If these nutrients are insufficient — noting low vitamin D in particular is common in the Northern Hemisphere — she refers the patient to Endocrinology for supplement intervention and even bone-building medications in select cases. She says nonunion specialists work as a team with Endocrinology, and she collaborates with colleagues in this discipline, often during the same preoperative visit.
Nonunion repair methodology
إصلاح عدم الالتحام
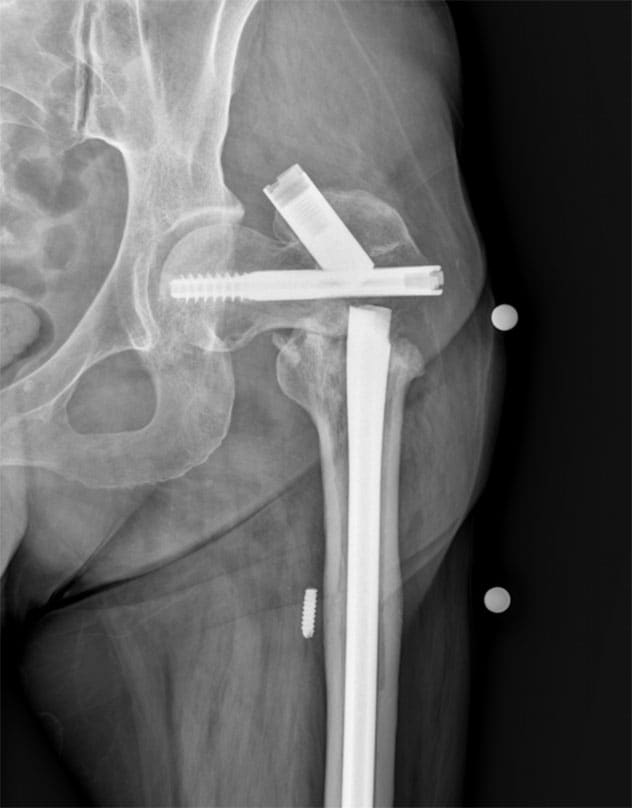
إصلاح عدم الالتحام
عدم التحام عظم الفخذ الداني مع فشل في الأجهزة
إصلاح عدم الالتحام
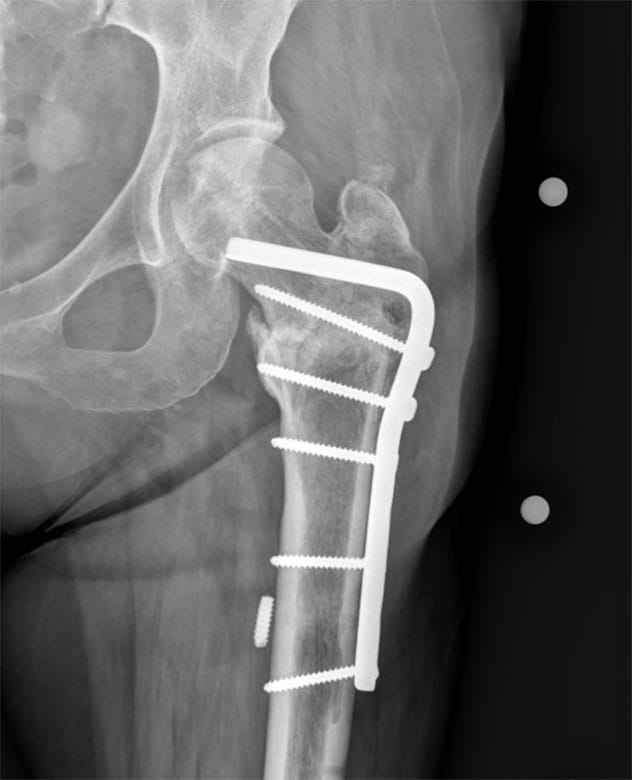
إصلاح عدم الالتحام
إصلاح مشكلة عدم التحام عظم الفخذ الداني الأيسر مع فشل في الأجهزة
Nonunion treatment depends on whether the patient is symptomatic, says Dr. Hidden. Most nonunion repairs involve biological adjuncts, preferably using the patient's own biology, either from the same bone presenting with nonunion or from the iliac crest or pelvis bone. If necessary for sufficient bone volume, the orthopedic surgeon may expand the biologics from the patient's body with donor bone or by taking bone from another area in the body. Though most patients accept donor bone use, if needed, Dr. Hidden indicates that cultural or religious factors occasionally cause patients to prefer different options.
Another alternative is to use bone graft substitutes to repair the nonunion, such as calcium phosphate bone cement.
While nonunions occur most frequently with lower extremities, a similar problem may arise in a repaired upper extremity, with gross mobility requiring further surgery.
When to refer or treat locally for nonunions
For orthopedic surgeons familiar and comfortable with nonunion repair, Dr. Hidden indicates it makes sense for them to operate on patients with this condition in the community. However, for surgeons trained in other aspects of orthopedics who are not as familiar with nonunions, she suggests a referral to Mayo Clinic's Orthopedic Trauma Service specialists.
For more information
Refer a patient to Mayo Clinic.