June 19, 2021
Mayo Clinic's use of state-of-the-art myelography facilitates the localization of even tiny cerebrospinal fluid (CSF) leaks. A key tool, used since 2018, is lateral decubitus digital subtraction myelography (DSM).
"Before you can treat a CSF leak, you have to find it. And that can be very tricky," says Carrie M. Carr, M.D., a neuroradiologist and chair of neuroradiology procedures at Mayo Clinic in Rochester, Minnesota. "Often the leak is small and subtle, but even a large leak can be quite difficult to image."
Lateral decubitus DSM is part of Mayo Clinic's new imaging protocol for patients who present with spontaneous intracranial hypotension. That protocol starts with:
- High-resolution brain MRI, which can measure abnormalities down to the millimeter
- High-resolution spinal MRI, which can detect even very small areas of extradural fluid
"Each of these successive steps is important," Dr. Carr says. "A standard spine MRI, without these specialized techniques, often can't tell us what type of myelogram would best find the precise location of the leak."
Spinal CSF leaks can cause debilitating symptoms. "Most patients I see are completely miserable. They are missing work and important life activities because of orthostatic headaches and other manifestations of CSF leaks," says Jeremy K. Cutsforth-Gregory, M.D., a neurologist and director of the CSF dynamics clinic at Mayo Clinic in Minnesota. "Many patients are rendered bedbound, but effective treatment is often available once the leak is found."
High diagnostic yield
At Mayo Clinic, specific findings on brain and spinal MRI guide decisions about subsequent myelography. Hyperdynamic CT myelogram is used when a herniated disc or an osteophyte appears to have caused a rent in the dura and CSF leak. Lateral decubitus DSM is used when a CSF-venous fistula or nerve root sleeve tear is suspected.
Lateral decubitus DSM at Mayo Clinic has a high diagnostic yield for finding the exact location of a CSF leak. A retrospective study published in Neurology in 2021 found that 53.2% of patients investigated for spontaneous intracranial hypotension at Mayo Clinic had a CSF leak identified on lateral decubitus DSM.
تصوير النخاع الرقمي
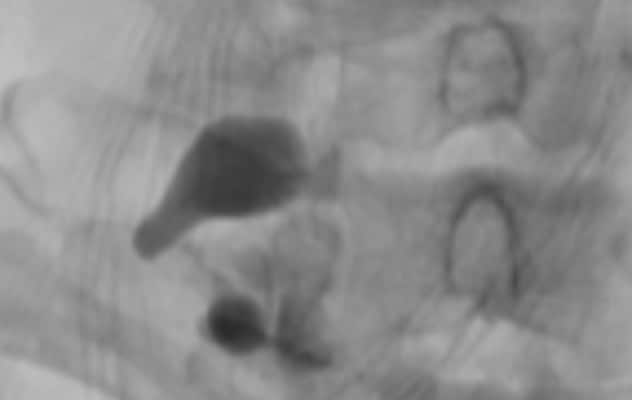
تصوير النخاع الرقمي
صورة توضح تشخيص امرأة عمرها 61 عامًا حضرت وهي تشعر بصداع حاد مفاجئ مرتبط بمناورة فالسالفا. وقد تعرضت المريضة في وقت لاحق لطنين الأذن وانخفاض السمع والصداع اليومي المستمر. وأظهر تصوير النخاع الرقمي الذي أُجري في مركز كبير عدم وجود تكتلات ورديدية حول رتج غلاف العصب غير الطبيعي.
تقنية تصوير النخاع الرقمي المعزز في مايو كلينك
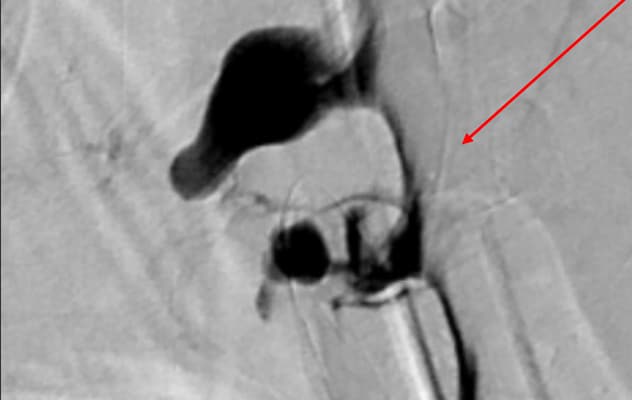
تقنية تصوير النخاع الرقمي المعزز في مايو كلينك
صورة توضح تشخيص امرأة عمرها 61 عامًا حضرت وهي تشعر بصداع حاد مفاجئ مرتبط بمناورة فالسالفا. وقد تعرضت المريضة في وقت لاحق لطنين الأذن وانخفاض السمع والصداع اليومي المستمر. أظهر تصوير النخاع الرقمي أثناء الاستلقاء على الجانب الذي أُجري في مايو كلينك وجود ناسور وريدي في السائل الدماغي النخاعي كبير ومعقد في المكان ذاته.
Dr. Carr notes that DSM can yield varying results, depending on the techniques used. She cites a recent patient who came to Mayo Clinic after DSM at another major center didn't detect a CSF leak. "We performed our lateral decubitus DSM protocol and found a very large CSF-venous fistula," Dr. Carr says. "A lot of highly specialized work has gone into perfecting our technique."
Mayo Clinic routinely performs bilateral DSM testing to evaluate both sides of the spine, as the presence of leak can be bilateral, though this is rare. The testing is performed over two days due to limits on the amount of contrast dye that can be injected. A succession of fluoroscopic images is taken, with any constant aspects of the successive images subtracted from the original.
"That helps us to detect change," Dr. Carr says. "Contrast flows into the fistula, opacifying the connection between the thecal sac and the abnormal connection to veins. These blood vessels are tiny, and the contrast can flicker, making it difficult to visualize. The digital subtraction technique makes these CSF-venous fistulas more conspicuous."
Treatment of spinal CSF leaks and CSF-venous fistulas typically involves spinal surgery, paraspinal vein embolization, epidural blood patch or fibrin glue injection. Determining the optimal treatment for each patient requires definitive localization and characterization of the leak.
"Surgery and embolization — the most definitive treatments — are only possible when the precise site of a leak is known," Dr. Cutsforth-Gregory says. "Epidural blood patch and fibrin glue can be applied in a nontargeted fashion but are much more effective when performed at the precise site of leakage. Adding CT guidance during patching enhances safety, as the needles — and thus the blood or fibrin — are directed closer to the nerve roots and the ventral aspect of the spinal cord. The close collaboration between neurologists and neuroradiologists at Mayo Clinic allows us to tailor the treatment to the clinical circumstances."
Mayo Clinic's distinguished history of imaging expertise is a cornerstone of Mayo's ability to manage CSF leaks. "We always put the patient first, and the practice supports innovation," Dr. Carr says. "We are willing to invest time and effort to successfully detect and treat CSF leaks."
For more information
Kim DK, et al. Diagnostic yield of lateral decubitus digital subtraction myelogram stratified by brain MRI findings. Neurology. 2021;96:e1312.