Aug. 08, 2020
Skeletal fragility related to osteoporosis is a common contributing factor to fracture in adults. Despite a number of effective treatments to lower the risk of fracture, osteoporosis remains underdiagnosed and undertreated even among individuals who have sustained a fragility fracture. Recent studies indicate that the rate of osteoporosis treatment initiation after a hip fracture has actually been declining in recent years such that in 2015 less than 5% of individuals not already on osteoporosis treatment at the time of hip fracture received such treatment. This undertreatment results in further fractures and the individuals' consequent pain, disability and loss of quality of life.
Recognizing the treatment gap as a contributing factor to the reversal of the trend in declining hip fracture incidence, leading researchers and bone health experts from the American Society for Bone and Mineral Research (ASBMR), National Osteoporosis Foundation, National Bone Health Alliance, Mayo Clinic and International Osteoporosis Foundation met on Sept. 19, 2016, at the ASBMR 2016 Annual Meeting and issued a call to action with recommendations to aggressively address the critical care gap and reduce fracture risk in our aging population. Sundeep Khosla, M.D., with Endocrinology, Diabetes, Metabolism, and Nutrition at Mayo Clinic's campus in Rochester, Minnesota, a leading participant in the call to action, described the purpose: "To address this osteoporosis treatment crisis, organizations representing patients, specialists, surgeons and primary care providers came together to pledge to intensify their current efforts and collaborate on new opportunities to increase the screening, diagnosis and treatment of individuals at high risk to prevent fractures and to partner with patients to make informed choices about osteoporosis treatment options." The call to action was endorsed by 39 organizations from around the world.
Dr. Khosla and other thought leaders including Bart L. Clarke, M.D., (ASBMR president at the time), and Ann E. Kearns, M.D., Ph.D., (representing the American Association of Endocrinologists, AACE), both with Endocrinology, Diabetes, Metabolism, and Nutrition at Mayo Clinic's campus in Rochester, Minnesota, convened an international multispecialty coalition to develop consensus recommendations regarding secondary fracture prevention. Dr. Clarke says, "The coordination role of the ASBMR in this endeavor is consistent with its mission not only to advance bone, mineral and musculoskeletal science worldwide but also to promote the translation of basic and clinical research to improve human health."
التوصيات المتفق عليها للوقاية من الكسور الثانوية
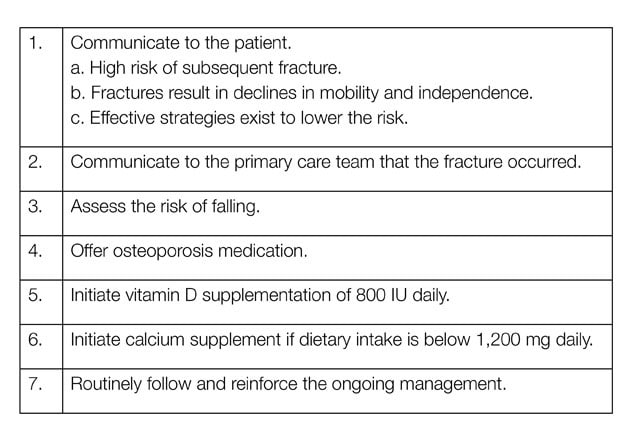
التوصيات المتفق عليها للوقاية من الكسور الثانوية
التوصيات الرئيسية المتوافق عليها للوقاية من الكسور الثانوية لدى الأشخاص الذين تزيد أعمارهم عن 65 عامًا الذين يعانون كسرًا في الوِرك أو العمود الفقري
The coalition included representation from medical specialists, primary care, orthopedic surgery and patient advocacy groups. Over a series of conference calls and in-person meetings, the coalition was able to develop consensus recommendations around secondary fracture prevention that were published in the Journal of Bone and Mineral Research in 2020. These recommendations have galvanized the message that an older person who has a vertebral or hip fracture is at high risk of additional fractures, requires treatment with osteoporosis medication in addition to adequate calcium and vitamin D, and warrants continued management to lower the risk of additional fractures.
Effective implementation of the recommendations is a team effort. Clinical endocrinologists play a key role by bringing their osteoporosis expertise to treat patients with complex cases and dispel myths and misperceptions about medication efficacy and complications. They also often lead or oversee fracture liaison services. In addition to her role with AACE, Dr. Kearns also leads the Fragility Fracture Clinic at Mayo Clinic in Rochester, Minnesota. "Case management systems such as fracture liaison services or fragility fracture clinics are very effective care delivery mechanisms to achieve the goals of not only initiating treatment but also educating patients and families and communicating with primary care providers about ongoing management," specifies Dr. Kearns.
The coalition is forging ahead with continued efforts to disseminate the key recommendations through the ASBMR Secondary Fracture Prevention Initiative website. Educational materials are also in development to assist patients and providers in discussions about optimizing skeletal health with fracture prevention as a key endpoint. In addition, efforts are ongoing to improve reimbursement for fracture liaison services to allow the best care delivery models to be financially viable for many institutions, and to develop and implement a national fracture registry that will enhance tracking and measurement of fracture rates.
For more information
Conley RB, et al. Secondary fracture prevention: Consensus clinical recommendations from a multistakeholder coalition. Journal of Bone and Mineral Research. 2020;35:36.
Clinical recommendations. American Society for Bone and Mineral Research.