Overview
Age spots are small, flat dark areas on the skin. They vary in size and usually appear on areas exposed to the sun, such as the face, hands, shoulders and arms. Age spots are also called sunspots, liver spots and solar lentigines.

Age spots on the shoulder and back
If you have skin that burns easily and spend a lot of time in the sun, you're more likely to develop age spots.
Age spots are very common in adults older than 50, but younger people can get them if they spend time in the sun.
Age spots can look like cancerous growths. True age spots don't need treatment, but they are a sign the skin has received a lot of sun exposure and are an attempt by your skin to protect itself from more sun damage. For cosmetic reasons, they can be lightened or removed.
You can help prevent age spots by regularly using sunscreen and avoiding the sun.
Symptoms
Age spots may affect people of all skin types, but they're more common in adults with skin that sunburns easily. Unlike freckles, which are common in children and fade with no sun exposure, age spots don't fade.
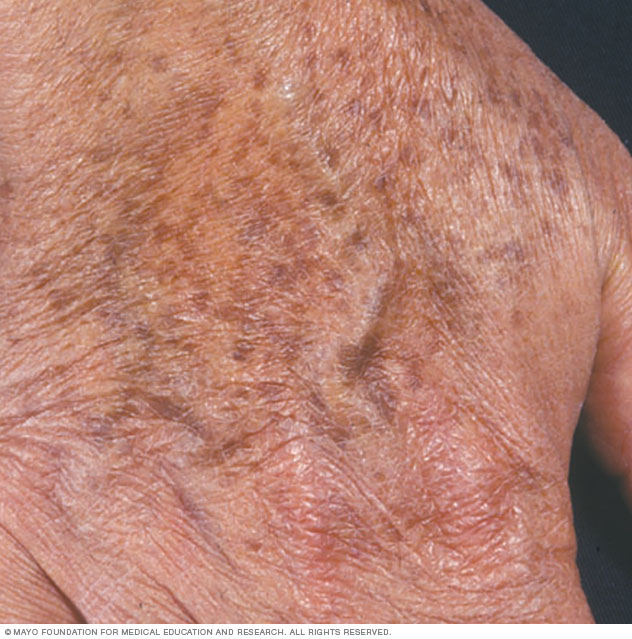
Age spots on the hand
Age spots may grow in size and group together, giving the skin a speckled or mottled appearance. They're very common in areas that get repeated sun exposure, such as on the back of the hand.
Age spots:
- Are flat, oval areas of increased pigmentation.
- Are usually tan to dark brown.
- Occur on skin that has had the most sun exposure over the years, such as the backs of hands, tops of feet, face, shoulders and upper back.
- Range from freckle size to about 1/2 inch (13 millimeters) across.
- Can group together, making them more noticeable.
When to see a doctor
Age spots don't require medical care. Have your doctor look at spots that are black or have changed in appearance. These changes can be signs of melanoma, a serious form of skin cancer.
It's best to have any new skin changes evaluated by a doctor, especially if a spot:
- Is black.
- Is increasing in size.
- Has an irregular border.
- Has an unusual combination of colors.
- Is bleeding.
From Mayo Clinic to your inbox
Causes
Age spots are caused by overactive pigment cells. Ultraviolet (UV) light speeds up the production of melanin, a natural pigment that gives skin its color. On skin that has had years of sun exposure, age spots appear when melanin becomes clumped or is produced in high concentrations.
Use of commercial tanning lamps and beds also can cause age spots.
Risk factors
You might be more likely to develop age spots if you have a history of frequent or intense sun exposure or sunburn.
Prevention
To help avoid age spots and new spots after treatment, follow these tips for limiting your sun exposure:
- Avoid the sun between 10 a.m. and 2 p.m. Because the sun's rays are most intense during this time, try to schedule outdoor activities for other times of the day.
- Use sunscreen. Fifteen to 30 minutes before going outdoors, apply a broad-spectrum sunscreen with a sun protection factor (SPF) of at least 30. Apply sunscreen generously, and reapply every two hours — or more often if you're swimming or perspiring.
-
Cover up. For protection from the sun, wear tightly woven clothing that covers your arms and legs and a broad-brimmed hat, which provides more protection than does a baseball cap or golf visor.
Consider wearing clothing designed to provide sun protection. Look for clothes labeled with an ultraviolet protection factor (UPF) of 40 to 50 to get the best protection.