Nov. 25, 2025
Mayo Clinic routinely uses the least invasive approach possible to treat craniosynostosis. Single-incision endoscopy can usually be performed — even for some infants with syndromic craniosynostosis — when the condition is diagnosed early.
"Ideally, we try to treat these infants before age 3 months. That requires an early pickup by parents and pediatricians, and early referral," says Edward S. Ahn, M.D., a pediatric neurosurgeon at Mayo Clinic in Rochester, Minnesota. "We often make exceptions, based on the individual. But the earlier, the better."
Mayo Clinic has experience treating all types of craniosynostosis, from complex genetic syndromes to single fusions. Each year, specialists at Mayo Clinic Children's treat more than 400 children with craniosynostosis or other craniofacial conditions. Neurosurgeons collaborate with pediatric craniofacial surgeons in the Cleft and Craniofacial Clinic at Mayo Clinic to provide care.
"The treatment for craniosynostosis is quite complex. The craniofacial surgeon and neurosurgeon perform different parts of the procedure, to ensure safe execution," says Waleed Gibreel, M.B.B.S., a pediatric plastic and craniofacial surgeon at Mayo Clinic's campus in Minnesota.
Endoscopic treatment typically avoids blood transfusion and scarring and requires only an overnight hospital stay. Dr. Ahn helped pioneer the single-incision approach. Mayo Clinic researchers also are studying ways to minimize helmet therapy and to train artificial intelligence models to diagnose craniosynostosis based on infants' photographs.
"For all of our patients with craniosynostosis, we're trying to be smarter and less invasive," Dr. Ahn says.
Multidisciplinary, patient-centered care
Early diagnosis of craniosynostosis is key to optimal treatment outcomes. "The intervention has to be early enough to prevent further malformation and to reshape the head," Dr. Ahn says.
Infants referred to Mayo Clinic often can be diagnosed with physical examination alone. "We generally try to avoid CT scan for diagnosis, to minimize radiation risks," Dr. Ahn says.
For children with more-complex conditions, including syndromic craniosynostosis, high-definition CT and MRI scans might be used to create computer-simulated surgical plans. Customized models and templates based on those personalized plans help guide calvarial vault remodeling. "Virtual surgical planning enhances the safety of these surgeries," Dr. Ahn says.
"For all of our patients with craniosynostosis, we're trying to be smarter and less invasive."
Children with syndromic craniosynostosis also benefit from the Cleft and Craniofacial Clinic's multidisciplinary expertise. Depending on a person's needs, the care team might include specialists — beyond neurosurgery and pediatric craniofacial surgery — in clinical genomics, medical social services, oral and maxillofacial surgery, orthodontics, ophthalmology, otolaryngology, prosthodontics, psychology and speech pathology.
"Multiple conditions can coexist with syndromic craniosynostosis. It's quite important for these children to be seen in a multidisciplinary team setting," Dr. Gibreel says.
Some infants with syndromic craniosynostosis can be treated with endoscopic therapy. In a study published in 2017 in the Journal of Neurosurgery: Pediatrics, researchers found that early endoscopic suturectomy followed by helmet therapy was sufficient to treat about half the children studied. "A fair number of these infants can achieve decent correction with minimally invasive means," Dr. Ahn says.
Endoscopic treatment requires postoperative helmet therapy to guide cranial growth, for optimal cosmesis. "But there's really no standard of care for how long to wear a helmet," Dr. Ahn notes.
In a study published in 2018 in the Journal of Neurosurgery: Pediatrics, researchers found that maximal correction is usually achieved in about eight months. "Beyond that, the helmet really doesn't do much," Dr. Ahn says. "We've been able to limit helmeting to eight months, and oftentimes, even less."
Potential future directions
Helmet therapy poses burdens for patients and their families. "The helmet needs frequent adjustment by a specialized occupational therapist who can monitor cranial growth," Dr. Gibreel says. "Patients might not have access to this specialized care or might lack the necessary resources for helmet therapy. Also, some kids really cannot tolerate the helmet."
"Multiple conditions can coexist with syndromic craniosynostosis. It's quite important for these children to be seen in a multidisciplinary team setting."
 Avoiding helmet therapy
Avoiding helmet therapy
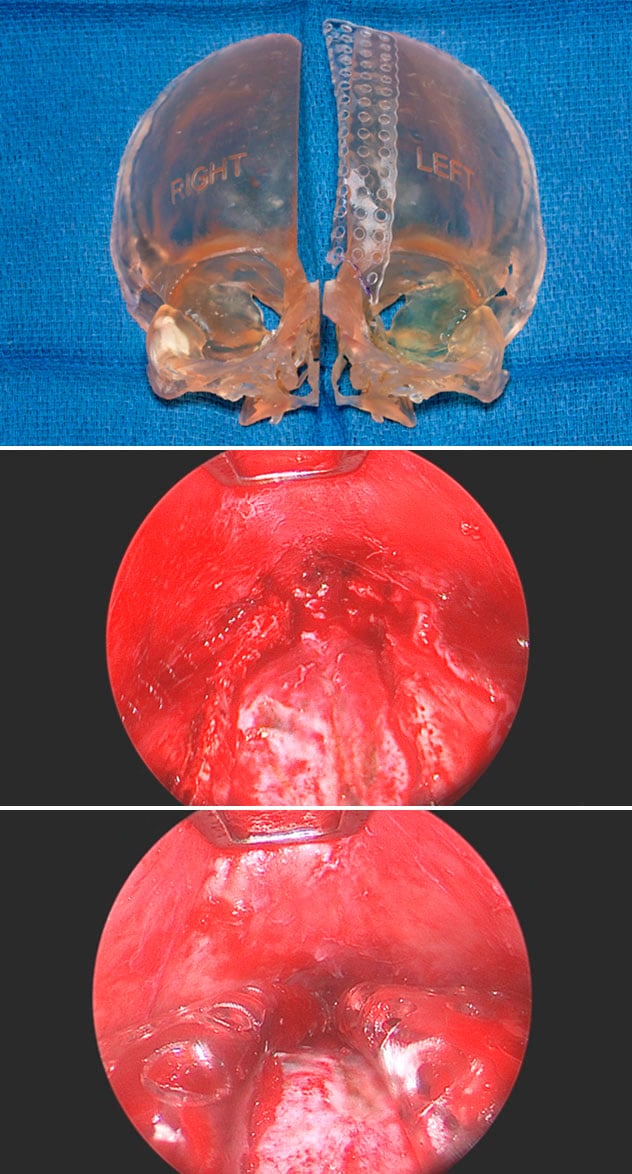
3D printed model of the skull (top) demonstrates suturectomy, followed by the application of an absorbable plate around the edge of the remaining bone. Endoscopic views of the suturectomy (middle) followed by the application of the absorbable plates (bottom).
At Mayo Clinic, a new approach helps some patients avoid helmet therapy after endoscopic surgery. Once the diseased cranial suture is removed, dissolvable plates are wrapped around the edges of the residual bone, to prevent refusion of the suture while the brain grows. The dissolvable plates have been used in other types of plastic surgery, such as cranial vault remodeling surgery. Their application to craniosynostosis arose from the clinical partnership of Drs. Ahn, Gibreel and Uldis Bite, M.D., a pediatric plastic and craniofacial surgeon at Mayo Clinic's campus in Minnesota.
"Our early results with this technique show promise," Dr. Ahn says. "The initial outcomes are very good."
Mayo Clinic clinician-scientists also are developing facial recognition software that can diagnose craniosynostosis based on photographs of an infant's head. Hundreds of photographs of infants affected and unaffected by craniosynostosis are used to train an artificial intelligence (AI) algorithm to recognize the condition.
"The preliminary results show that artificial intelligence is very accurate at detecting craniosynostosis based on the images," Dr. Ahn says. "We'd potentially achieve much faster treatment if family doctors or pediatricians had access to a diagnostic tool and didn't have to wait for a specialist."
The AI project is a joint effort by Dr. Ahn and Bradley J. Erickson, M.D., Ph.D., a neuroradiologist at Mayo Clinic's campus in Minnesota who researches computer-aided diagnosis. "AI can help identify diseases in the home and get patients in for diagnosis and treatment sooner, and that is good for everyone," Dr. Erickson says.
Routine cross-specialty cooperation facilitates this patient-focused research. "Collaboration is built into the culture of Mayo Clinic," Dr. Ahn says. "Everyone wants to make advances that ultimately help patients."
For more information
Mayo Clinic Children's. Mayo Clinic.
Cleft and Craniofacial Clinic. Mayo Clinic.
Hersh DS, et al. Endoscopic surgery for patients with syndromic craniosynostosis and the requirement for additional open surgery. Journal of Neurosurgery: Pediatrics. 2017;20:91.
Iyer RR, et al. Optimal duration of postoperative helmet therapy following endoscopic strip craniectomy for sagittal craniosynostosis. Journal of Neurosurgery: Pediatrics. 2018;22:610.
Refer a patient to Mayo Clinic.