Aug. 28, 2020
Editor's note: This interview originally published on July 17, 2020, in OncLive, written by Erica DiNapoli. It has been updated and shared here with permission from OncLive.
A slew of actionable alterations has emerged in colorectal cancer (CRC) in recent years, and with their identification comes targeted therapies that are boosting survival outcomes, according to Daniel H. Ahn, D.O. Now, research efforts are focused on exploring novel combinations and sequencing strategies to further move the needle.
"In the past, we didn't have many targetable alterations — all we had was anti-EGFR monoclonal antibody therapy for patients with KRAS wild-type disease," said Dr. Ahn. "We now have identified numerous targetable alterations. Approximately 50% to 75% of patients could potentially benefit from some form of targeted therapy. Many of these rare alterations were once deemed "undruggable," and now they just might be (treatable)."
In an interview with OncLive, Dr. Ahn, medical oncologist and assistant professor of medicine at Mayo Clinic in Phoenix, Arizona, elaborated on exciting updates in CRC, the importance of tumor sidedness in guiding treatment decisions, the emergence of targetable alterations and ongoing research efforts.
What are some of the recent developments that have been made in CRC?
With regard to updates in CRC, specifically from what we've seen during the 2020 ASCO Virtual Scientific Program and the 2020 ESMO World Congress on Gastrointestinal Cancer, the big theme that I've noticed is that "less chemotherapy is more." In other words, there's been a lot of fresh new data looking at targeted therapies as well as combination strategies in the advanced setting. Most recently, we had the update from KEYNOTE-177, which showed the efficacy of pembrolizumab compared with physician's choice of chemotherapy for patients with treatment-naive, metastatic, microsatellite instability-high CRC. Essentially, what that trial showed was a near doubling in progression-free survival (PFS) (with pembrolizumab) compared with chemotherapy. While, at this time, the median overall survival (OS) has not been (reached). This study was designed so that if either of the primary endpoints were met, then it would be considered a success. Given the significant benefit observed in PFS, the study did meet its primary endpoint and recently, the Food and Drug Administration (FDA) did approve the use of pembrolizumab for patients in the frontline setting.
Interestingly, a lot of advancement has been seen with targeted therapies. If we look back at 2010, the only mutation we were aware of in CRC was KRAS exon 2; however, over the past decade, we've seen lush new data (in this area). From undergoing tumor genomic sequencing, as well as developing a better understanding of tumor biology in terms of left-sided versus right-sided tumors, we have a lot of data suggesting that a bevy of other alterations could potentially be actionable. In addition to KRAS mutations, we now understand more about KRAS G12C mutations and pan-KRAS inhibitors also are coming out. A lot of advancements have been made with regard to BRAF V600E mutations, most notably from the BEACON trial and the ANCHOR study. We also know about FGFR alterations, NTRK and ROS1, and ALK aberrations. We know that up to 50% to 75% of patients may benefit from some type of targeted therapy.
Aside from mutational status, how has tumor location impacted treatment decisions?
Data over the past three years have helped us to better understand that tumor sidedness does matter. When we look at sidedness, we know that differences exist with regard to genomic alterations. Right-sided tumors tend to be associated with BRAF V600E mutations and a higher prevalence of KRAS mutations, while left-sided, or even rectal, tumors tend to have a higher incidence of HER2 alterations. Some other genomic alterations also are coming into play. When we looked at the data from CALGB/SWOG 80405, results showed that sidedness does matter in terms of sequencing treatments.
We know that, specifically with regard to the right-sided tumors, patients should probably receive anti-VEGF monoclonal antibody therapy prior to anti-EGFR monoclonal antibody therapy. For those with left-sided tumors, the data are less clear. However, we at least know that, on the right side, there can be a potential prognostic effect with sequencing these agents.
Could you expand a bit on how the genomic alterations differ between the left-sided and right-sided tumors?
With regard to targetable alterations, one area that has garnered a lot of interest is HER2-targeted therapies. To this end, it's important to mention the DESTINY-CRC01 trial, the MOUNTAINEER trial, and the initial phase 1 results with the Zymeworks' compound ZW25. (All these trials showed) that targeting HER2 is a relevant treatment strategy in patients with advanced CRC and all these agents appeared to have efficacy, with response rates that varied from 35% to up to 50% and a similar PFS of around six months or so. As such, all these therapies appear to be effective in terms of treating (patients with) HER2-amplified CRC. The treatment strategy, along with how we sequence these agents, is going to be really important going forward.
These classes of agents all have different toxicity profiles. For example, with fam-trastuzumab deruxtecan-nxki (Enhertu; DS-8201) being an antibody-drug conjugate, one of the unique toxicities that was observed with the agent in the phase 2 study was pneumonitis. About 6% of patients did experience pneumonitis, which is not typically seen with many of these agents. For example, if a patient had underlying comorbidities, such as chronic obstructive pulmonary disease or interstitial lung disease, that agent would not be my first choice.
Tucatinib in combination with trastuzumab showed a significant benefit in breast cancer, and those data were published in the New England Journal of Medicine in 2019 and led to its FDA approval. The combination is now being investigated in CRC. John Strickler, M.D., of Duke University School of Medicine, led this effort in the MOUNTAINEER trial through the ACCRU research consortium. A multi-institutional phase 2 study showed that the combination was not only effective, but safe. Results showed a response rate of nearly 50%, a PFS of approximately seven months, and an OS of approximately 18 months. That study is still ongoing with an expansion. All of this points to the fact that targeting HER2 is a relevant strategy in gastrointestinal malignancies, including CRC.
Looking specifically at the relapsed/refractory setting, could you discuss some of the exciting combination trials that are being conducted in the third-line setting?
Las vías PI3K y MAPK
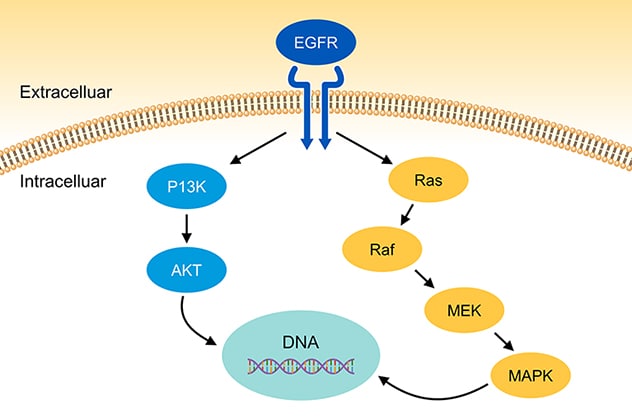
Las vías PI3K y MAPK
Las vías PI3K y MAPK y sus asociaciones con la oncogénesis en el cáncer colorectal
An area that always remains of interest is targeting KRAS mutations; specifically, KRAS G12C has been an area of interest, with two compounds currently under investigation: the Amgen compound AMG 510 and the Mirati Therapeutics Inc. compound (MRTX849). We have seen phase I results (with these agents), and (data) were presented at the 2019 ESMO Congress and most recently at the 2020 ESMO World Congress on Gastrointestinal Cancer. Results showed that patients treated with these agents experienced a favorable toxicity profile. However, when we looked at the response rates, they were very minimal and modest, ranging from approximately 5% to 7%. Additionally, PFS was about 4.2 months, as seen with AMG 510. As such, based on a lot of preclinical data, combination strategies are going to be investigated even more moving forward.
The CodeBreak 101 trial is examining combinations consisting of PD-L1 inhibitors, MEK inhibitors and anti-EGFR monoclonal antibody therapies; these are all strategies that are aimed at downstream targeting RAS, which can sometimes be activated, or other co-parallel downstream signaling pathways. Potentially there may even be an immunogenic phenomenon that needs to be investigated. Initial results from CodeBreak 100 demonstrated the potential efficacy of these agents. Now, moving forward, combination strategies are of interest will be investigated in this multiarmed study.
Another agent that appears very interesting for the rest of the KRAS mutations is onvansertib; this is a PLK1 inhibitor that is currently being investigated in CRC. We currently have the phase 1b/2 study open here at Mayo Clinic, which I have been fortunate to lead. Preclinically, results showed that PLK1 is often overexpressed in patients with solid tumor malignancies. Specifically, in KRAS-mutated metastatic CRC, RAS mutant cells can experience synthetic lethality when PLK is inhibited with synergistic anti-tumor activity when administered in combination with various chemotherapy agents. Based off these preclinical data, we conducted the second line study of FOLFIRI (leucovorin calcium, 5-fluorouracil and irinotecan) in combination with bevacizumab and onvansertib. Results showed a response rate of near 44% with the regimen. Typically, in this patient population, we expect to see a response rate of up to 10% in patients with KRAS mutations in the second line setting. The data appear to be very intriguing, and notably, the combination also appears to be safe and well tolerated. This study will be moving forward to the phase 2 component.
What are some of the approaches under investigation for patients whose tumors do not harbor genomic alterations?
An area of interest right now is: What about patients who don't have genomic alterations? Specifically, what do we do for patients who have microsatellite stable or RAS wild-type disease, or those who don't have any other potentially targetable alterations such as BRAF, HER2 or FGFR? What do we do for these patients? A lot of interest has been channeled into strategies dedicated to understanding how we can make "cold" tumors into "hot" ones.
To this end, many were looking forward to the REGONIVO trial with regorafenib/nivolumab data as well as the data with regorafenib/avelumab. Initial results reported in Japan showed that the combination of regorafenib, a multitargeted TKI, with PD-L1 inhibition can result in potential synergistic effect. Unfortunately, when they presented the updated results at 2020 ESMO World Congress on Gastrointestinal Cancer, as well as the results from the regorafenib/avelumab study, the response rates were not as robust as those previously observed from our Japanese colleagues.
Specifically, data from the REGONIVO trial that were recently presented showed response rates of less than 5%. Out of the 21 patients that were enrolled in the study, only one patient had a partial response. It does not appear that the combination of these two agents have significant activity. In some ways, this was expected.
Moving forward, strategies are going to be examining other ways to potentially prime the immune system. Unfortunately, we've already investigated atezolizumab in combination with a MEK inhibitor cobimetinib and that did not pan out in a phase 3 study (IMblaze370). However, other potential strategies at priming the immune system include adoptive T cell therapies in combination with immunotherapy strategies, which remains of interest.
Sequencing options is also of great importance. One study that was presented at the 2018 Gastrointestinal Cancers Symposium was the REVERCE trial. In that study, patients were randomized in a 1-1 ratio; one group received regorafenib before the anti-EGFR monoclonal antibody therapy cetuximab, and the other group received the opposite order. At that time, it wasn't understood whether sequencing treatments that were already FDA approved would lead to better outcomes. Interestingly, what they observed in the Japanese study was that patients who received regorafenib prior to anti-EGFR monoclonal antibody therapy saw a near six-month improvement in OS as well as an improvement in PFS-2.
Based off these intriguing data, we are now leading the REVERCE II trial in the United States, which will investigate the same concept. We are examining whether sequencing strategies matter for patients with MSS, RAS wild-type, metastatic CRC. Patients will be randomized in a 1-1 ratio to receive either regorafenib followed by an anti-EGFR monoclonal antibody therapy, assuming that they haven't received either one, in combination with irinotecan or the (reverse sequencing). Patients will be able to receive either panitumumab or cetuximab based on investigator's discretion. The primary endpoint of the study is OS. Based on the intriguing early data that we observed from our Japanese colleagues, hopefully we can better understand how sequencing matters moving forward.
What are some of the challenges in this space that you hope to see addressed in the future?
While there have been a lot of positive data, especially with these targeted therapies, when we look at overall outcomes, patients eventually do progress on many of these approaches. When results from the BEACON and ANCHOR trials were presented, we saw that in both the refractory and the frontline settings, the PFS results were very similar. We need to develop a better understanding with regard to the mechanisms of resistance of these targeted therapies. We have to understand whether it's a potential immunogenic effect or the emergence of new mutation clones. Interplaying tumor biopsies, or liquid tumor biopsies, to better understand the development of secondary resistance mechanisms is important.
While these agents that target genomic alterations are very effective and can provide a significant benefit for many patients, we know that eventually the patients will progress. Gaining a better understanding of why they progress is the next step forward.
What is your take home message?
The recurring theme that we continue to discuss is: Sequencing and testing does matter. Initially, we were mainly concerned about (differentiating between) KRAS-mutated or non-KRAS-mutated disease. Now, BRAF, HER2, FGFR, NTRK, ROS1 and ALK aberrations have also emerged. We have seen great results, especially with some of these rare alterations like NTRK. When you combine these rare alterations, even though some of these may be found in less than 1% of all patients with CRC, when you combine some of these, we're really talking about potentially another 25% of patients who could have a molecularly targeted therapy available to them, whether it's through standard approved therapies or clinical trials.