Diagnosis
You first may see someone on your primary healthcare team for your symptoms. You may be referred to a sleep specialist in a sleep disorder center.
A sleep specialist can help you decide whether you need more testing. That might involve overnight monitoring of your breathing and other body functions during a sleep study called polysomnography.
During polysomnography, you're connected to equipment that monitors your heart, lung and brain activity, breathing patterns, arm and leg movements, and blood oxygen levels while you sleep. You may have a full-night or a split-night sleep study.
In a split-night sleep study, you're monitored during the first half of the night. If you're diagnosed with central sleep apnea, staff might wake you to start treatment for the second half of the night. Treatment might be positive airway pressure or supplemental oxygen.
Polysomnography can help diagnose central sleep apnea. It also can help rule out other sleep disorders, such as obstructive sleep apnea, repetitive movements during sleep or narcolepsy. These other conditions can cause daytime sleepiness but require different treatment.
Other specialists may be able to help detect central sleep apnea. These might include doctors trained in nervous system diseases, known as neurologists, or doctors trained in heart disease, known as cardiologists. You may need imaging of your head or heart to look for conditions that play a part in central sleep apnea.
Treatment
Continuous positive airway pressure (CPAP)
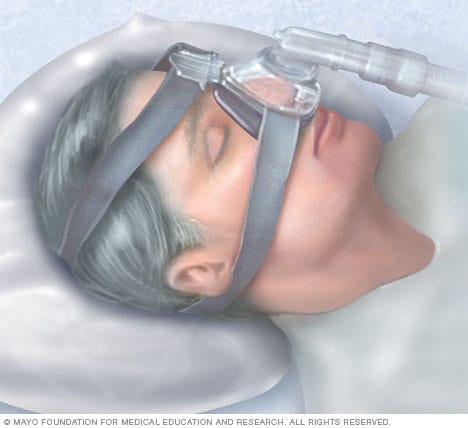
Continuous positive airway pressure (CPAP)
To treat central sleep apnea, your healthcare team may recommend a positive airway pressure machine. Positive airway pressure devices for central sleep apnea include continuous positive airway pressure (CPAP), bilevel positive airway pressure (BPAP) and adaptive servo-ventilation (ASV). These devices deliver pressurized air through a tight-sealing mask to help support breathing.
Treatments for central sleep apnea might include:
- Addressing underlying medical conditions. Central sleep apnea is sometimes caused by other medical conditions. Treating those conditions might help your central sleep apnea. For example, therapy for heart failure might improve central sleep apnea.
- Reducing opioid medicines. If opioid medicines are causing your central sleep apnea, your healthcare team might reduce your dose of those medicines over time to improve your sleep apnea.
-
Continuous positive airway pressure, also called CPAP. This treatment, also used to treat obstructive sleep apnea, involves wearing a mask over the nose or over the nose and mouth while asleep.
The mask attaches to a small pump that supplies a continuous amount of pressurized air to hold open the upper airway. CPAP may prevent the airway closure that can trigger central sleep apnea.
It's important that you use the CPAP device only as directed. If your mask is uncomfortable or the pressure feels too strong, talk with your healthcare team. Several types of masks are available. The care team also can adjust the air pressure.
-
Adaptive servo-ventilation, also called ASV. If CPAP doesn't effectively treat your condition, you might be given ASV. Like CPAP, ASV delivers pressurized air.
Unlike CPAP, ASV adjusts the amount of pressure delivered as you breathe. This smooths out your breathing pattern. The device also may automatically deliver a breath if you haven't taken one within a certain number of seconds.
ASV isn't recommended for people with symptoms of heart failure.
- Bilevel positive airway pressure, also called BPAP. Like ASV, BPAP delivers a certain amount of pressure when you breathe in and a different amount of pressure when you breathe out. Unlike ASV, the amount of pressure delivered when you breathe in is the same each time rather than changing with each breath. BPAP also can be set to deliver a breath if you haven't taken one within a certain number of seconds.
- Supplemental oxygen. Using supplemental oxygen while you sleep might help if you have central sleep apnea. Various devices are available to deliver oxygen to your lungs.
- Medicines. Medicines such as acetazolamide have been used to stimulate breathing in people with central sleep apnea. These medicines might be prescribed to help your breathing as you sleep if you can't tolerate positive airway pressure.
Surgery or other procedures
A newer therapy for central sleep apnea is transvenous phrenic nerve stimulation. With this treatment, a device approved by the U.S. Food and Drug Administration known as the Remede System delivers an electrical pulse to the nerve that controls the diaphragm during sleep. This causes you to take a breath. The system includes a battery-powered pulse generator that's implanted under the skin in the upper chest.
Used for moderate to severe central sleep apnea, this system produces a steady breathing pattern. Researchers continue to study this system and its use.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Preparing for your appointment
You're likely to start by seeing a member of your primary healthcare team. You might then be referred to a sleep specialist.
Here's some information to help you get ready for your appointment.
What you can do
- Bring results of earlier sleep studies or other tests with you or ask that they be sent to your care team.
- Bring someone who has observed your sleep, such as a spouse or partner, to your appointment. This person will likely be able to give more information to your care team.
- Write down your symptoms, including any that may seem unrelated to the reason for which you scheduled the appointment, and when they began.
- Write down key personal information, including major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you take, including doses.
- Write down questions to ask your healthcare team.
For central sleep apnea, some basic questions to ask include:
- What's the most likely cause of my symptoms?
- Are there other possible causes for my symptoms?
- What tests do I need? Do these tests require special preparation?
- Is this condition short term or long lasting?
- What treatments are available, and which do you recommend?
- How will treating or not treating my central sleep apnea affect my health now and in the future?
- I have other health conditions. How can I best manage these conditions together?
- Are there brochures or other printed material that I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your healthcare team is likely to ask you several questions, such as:
- Do you have symptoms all the time or do they come and go?
- Can you describe your typical sleep schedule?
- How long do you sleep, and do you sleep soundly? How many times do you wake during the night?
- Do you know if you snore?
- How do you feel when you wake up? Are you short of breath?
- Do you fall asleep easily during the day?
- Has anyone ever told you that you stop breathing while you're sleeping?
- Are you short of breath when you wake up at night?
- Do you have a heart condition? Have you had a stroke?