Dec. 20, 2022
John M. Tokish, M.D., an orthopedic surgeon specializing in shoulder repair at Mayo Clinic in Arizona, and team developed a shoulder instability procedure to address bone loss in patients undergoing instability surgery. The procedure, described in a 2020 issue of Arthroscopy Techniques, addresses bone loss that accompanies repeated shoulder dislocations following initial injury with a labral tear. This arthroscopic procedure utilizes a bone graft to augment the glenoid along with labrum repair. The procedure also uses suture anchors rather than metal or plastic screws, which Dr. Tokish and colleagues describe in the April 2022 edition of Arthroscopy Techniques, a free, open-access journal.
"This repair is effective with low complication rates and strong reducibility for surgeons nationwide," says Dr. Tokish. Suture anchor fixation also avoids previously reported drawbacks with other materials.
"This is a promising new advance decreasing shoulder instability repair morbidity," says Dr. Tokish.
Shoulder instability commonly occurs in older adults from falls and is prevalent in athletes ages 13 to 25.
"We really see it in young athletes who participate in contact sports," said Dr. Tokish. "Typical mechanism of injury examples are football tackles or motorcycle crashes."
Prior to injury, the glenoid cavity may appear pear shaped. However, significant bone loss converts it to an inverted pear shape. The injury transforms the glenoid's rounded crest to a missing arc.
Shoulder instability repair technique evolution
In 1954, Michel Latarjet, M.D., a French surgeon, developed a repair for shoulder instability with bone loss, transferring a portion of the coracoid to the glenoid. This repair is described in a 2016 Knee Surgery, Sports Traumatology, Arthroscopy article. "The Latarjet procedure had good outcomes yet was technically difficult and challenging for broad replication," says Dr. Tokish.
Due to this shortcoming, arthroscopic Bankart repair — attaching the glenoid labrum and joint capsule, a procedure Dr. Tokish calls "simple, fast and slick" — surpassed Latarjet in the 1970s.
Yet, an article on the Bankart technique published in a 2000 issue of Arthroscopy noted a 6.5% failure rate in 194 patients studied after arthroscopic Bankart repair. Though Dr. Tokish considers this acceptable, if the patient had bone loss, failure rate was 69%. For contact athletes, failure rate was 89%.
A concern with a Bankart repair is how to address soft tissue damage that contributes to shoulder instability yet excludes bony structure repair. The initial injury may damage the glenoid and humeral head, leading to repeated dislocation resulting in additional bone loss over time.
The data in this Arthroscopy article prompted the Latarjet's resurgence, especially in France, with low early failure rates, according to Dr. Tokish, yet Latarjet's learning curve was steep.
"Latarjet works — it's wonderful, but most people are uncomfortable doing it," he says.
Surgeons using the Latarjet then incorporated intraoperative monitoring triggers — nerve alerts — warning about nerve damage risk and need for technique modification. Next, in a 2014 Neer Award paper published in the Journal of Shoulder and Elbow Surgery, a Boston research group found nerve alerts occurred during 77% of Latarjet procedures studied. When investigators evaluated postoperative complications, 21% demonstrated nerve damage, though most resolved.
Some surgeons suggested improper technique prompted complication rates. But a study based on French recommendations found no statistically significant differences in post-Latarjet nerve damage. The study was published in a 2012 issue of The Journal of Bone and Joint Surgery.
"It's a rare complication, but if it happens, it's a significant problem," says Dr. Tokish.
Due to concerns with the Latarjet procedure, some surgeons transitioned to repair via autograft and allograft from sources such as iliac crest bone. However, a Latarjet vs. iliac crest bone graft transfer study published in Journal of Shoulder and Elbow Surgery demonstrated significant postsurgical hip pain. Other surgeons continued with traditional Bankart repair.
Bankart versus techniques addressing bone loss
Measuring bone loss percentage is crucial for shoulder instability injuries, says Dr. Tokish. At 13% glenoid bone loss, Bankart failure rate is high; notably, over half of patients have 13.5% bone loss post-injury.
Dr. Tokish is concerned that by using the Bankart, a soft tissue repair which does not augment bone, surgeons are failing to address missing bone.
Though Dr. Tokish's new procedure involves distal clavicle autograft, he indicates a surgeon may customize an allograft or autograft source from the iliac crest, distal clavicle, distal tibia or donor graft, based on individual injury. Potential determining factors include limited donor graft storage time and bone quantity needed.
"Distal clavicle is the patient's own bone," says Dr. Tokish. "It's free, but grafts can be smaller, so it can't work for significant bone loss."
Mayo Clinic in Arizona distal clavicle allograft experience and patient referrals
فيديو الإجراء الطبي
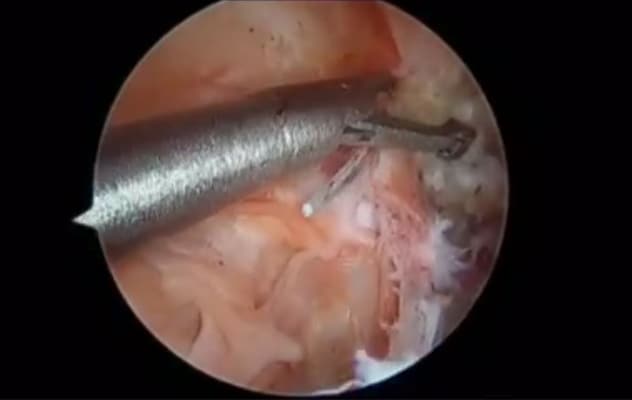
The arthroscopic bone grafting procedure Dr. Tokish developed has performed well for Mayo Clinic in Arizona. It has demonstrated known arthroscopic procedure cosmetic and healing benefits and has low dislocation and graft site morbidity rates.
Nerve damage risk has prevented some patients from pursuing shoulder instability repair, especially those concerned about sports careers, he says. Dr. Tokish's technique uses standard portals that most surgeons are familiar with, and it does not require the steps that the Latarjet does, decreasing the potential risk of nerve injury.
Dr. Tokish invites surgeons whose patients may benefit from the allograft or autograft with suture anchor technique to refer patients to Mayo Clinic in Arizona.
For more information
Hassebrock JD, et al. Arthroscopic technique for bone augmentation with suture button fixation for anterior shoulder instability. Arthroscopy Techniques. 2020;9:e97.
Tokish JM, et al. Arthroscopic technique for distal tibial allograft bone augmentation with suture anchor fixation for anterior shoulder instability. Arthroscopy Techniques. 2022;11:e903.
Van der Linde JA, et al. The Bristow–Latarjet procedure, a historical note on a technique in comeback. Knee Surgery, Sports Traumatology, Arthroscopy. 2016;24:470.
Burkhart SS, et al. Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy. 2000;16:677.
Delaney RA, et al. 2014 Neer Award paper: Neuromonitoring the Latarjet procedure. Journal of Shoulder and Elbow Surgery. 2014;23:1473.
Shah AA, et al. Short-term complications of the Latarjet procedure. The Journal of Bone and Joint Surgery. 2012;94:495.
Moroder P, et al. Neer Award 2019: Latarjet procedure vs. iliac crest bone graft transfer for treatment of anterior shoulder instability with glenoid bone loss: a prospective randomized trial. Journal of Shoulder and Elbow Surgery. 2019;28:1298.
Refer a patient to Mayo Clinic.
Disclosure
Dr. Tokish is a consultant for Arthrex, a company working with implants, but which has not provided funding for this project.