Feb. 01, 2020
The treatment of cardiovascular disease is increasingly guideline driven, gleaned from data collected in clinical trials. Technological advances and changing clinical practice require that these guidelines be periodically revisited and updated.
The 2014 American Heart Association/American College of Cardiology (AHA/ACC) valvular heart disease guidelines updated recommendations were previously reviewed in 2006. These guidelines included recommendations regarding timing of surgical intervention in severe aortic regurgitation. While the studies used to formulate the updated recommendations were the best available, they were nonetheless based on patient populations evaluated more than 20 years ago.
Moreover, these prior studies did not routinely include nonsurgical patient populations or uniformly control for the effects of concomitant coronary artery disease. Additionally, echocardiographic parameters to quantitate aortic valve function and ventricular diastolic function were not yet standardized. Furthermore, over the decades, the pathophysiology of aortic regurgitation has changed and surgical experience and the technical aspects of valve repair have evolved.
A recent study led by Patricia A. Pellikka, M.D., cardiologist at Mayo Clinic in Rochester, Minnesota, and director of the Mayo Clinic Echocardiography Laboratory, addresses these contemporary issues in patients with isolated chronic aortic regurgitation of at least moderate severity in light of the 2014 AHA/ACC guidelines.
Imágenes transtorácicas que ilustran los mecanismos de la regurgitación de la válvula aórtica
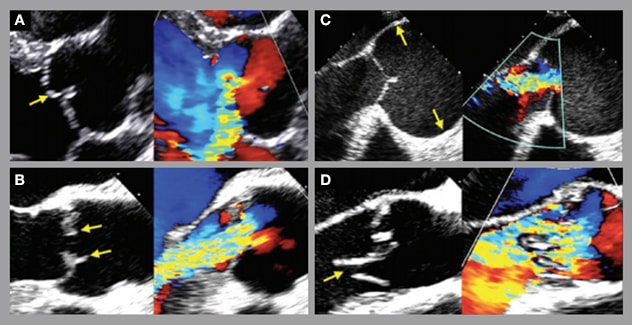
Imágenes transtorácicas que ilustran los mecanismos de la regurgitación de la válvula aórtica
A. Prolapso de la cúspide (flecha). Movimiento excesivo y tejido de cúspide redundante, y borde libre por debajo del plano anular o por debajo de la cúspide opuesta en la diástole, generalmente asociado con el chorro excéntrico que se opone a la cúspide prolapsante. B. Restricción y retracción de la cúspide (flechas). Restricción: disminución de la movilidad sistólica en la cúspide. Retracción: acortamiento cualitativo de la distancia entre la base de la cúspide y su borde libre en comparación con otras cúspides. C. Dilatación de la raíz aórtica (flechas). Dimensiones: >2 desviaciones estándar de los valores de referencia normales. Anillo: >27 mm (hombres); >24 mm (mujeres). Unión sinotubular: >35 mm (hombres); >32 mm (mujeres). D. Perforación de la cúspide (flecha). Caída de tejido dentro del cuerpo de la cúspide acompañada de un flujo de color que penetra en el defecto.
Dr. Pellikka and colleagues retrospectively reviewed 748 consecutive patients who underwent comprehensive transthoracic echocardiographic evaluation at Mayo Clinic in Rochester, Minnesota, between January 2006 and October 2017 and were identified as having isolated, moderate-severe or severe aortic regurgitation. Their results were published in the Journal of the American College of Cardiology in 2019.
Patients with concomitant aortic or mitral stenosis, mitral regurgitation, endocarditis, aortic dissection, prior mitral or aortic valve surgery, hypertrophic cardiomyopathy, ischemic cardiomyopathy, prior myocardial infarction or coronary artery bypass grafting, or terminal malignancies were excluded from the review.
Comprehensive transthoracic echocardiographic evaluation with chamber quantification was performed, including measurements of left ventricular chamber dimensions and systolic and diastolic function. An integrated diagnostic approach combining quantitative and semiquantitative measures — proximal isovelocity surface area-derived regurgitant volume (PISA), vena contracta width and time-velocity integral of the reversed flow in the descending aorta — was used to determine aortic regurgitation severity.
Symptom status was determined by documentation in the electronic health record by the treating cardiologists and cardiovascular surgeons. Surgical indications and class were defined by the 2014 AHA/ACC guideline criteria, including symptoms (Class I), left ventricular (LV) ejection fraction less than 50% (Class I), surgery for aortic disease (Class I), indexed LV end-systolic dimension greater than 25 mm/m2 (Class IIa), LV end-systolic diameter greater than 50 mm (Class IIa) and LV end-diastolic dimension greater than 65 mm (Class IIb).
The endpoint was all-cause mortality; cardiac mortality was not used due to the limitations of data derived from death certificates. The observation period was the time between date of qualifying transthoracic echocardiographic evaluation and last evaluation or death. Mean overall observation duration for the group was 4.9 years. The mean age of the group was 58 ± 17 years, and 18% were female. Aortic valve surgery was performed in 48% of patients (and of those almost 90% were within six months of contact) and included repair in 27% and replacement in 73% of these; 52% of patients did not have surgery.
Importantly, this study demonstrated that the decision to pursue surgical intervention in patients with aortic regurgitation of at least moderate-severe degree was driven largely by the presence of Class I indications, of which symptoms were by far the most common; Class II indications were the only criteria in 14% of patients who went on to surgery. However, the researchers also noted that symptom status was a strong predictor of all-cause mortality, despite the fact that surgical mortality has been reduced to very low levels. Symptomatic patients were older and had more severe diastolic dysfunction. Over 80% of symptomatic patients did not have guideline-defined LV enlargement, perhaps delaying recognition of clinically significant aortic regurgitation.
Supervivencia después de la cirugía de la válvula aórtica
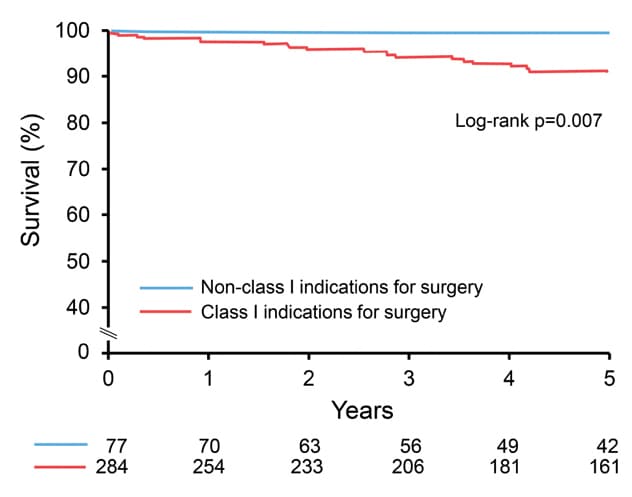
Supervivencia después de la cirugía de la válvula aórtica
Supervivencia después de la cirugía de la válvula aórtica según la indicación.
Other than aortic valve surgery, which was associated with better survival, the LV end-systolic diameter indexed to body surface area was the only objective criterion linked to all-cause mortality. The risk of death clearly began to increase when LV end-systolic diameter index exceeded 20 mm/m2, with a 1.5-fold increase in mortality compared with patients with LV end-systolic dimension index less than 20 mm/m². This measurement is lower than the threshold of 25 mm/m² or greater suggested by current guidelines.
This variable is likely to be particularly important in identifying asymptomatic surgical candidates among women and elderly patients with smaller body surface areas who are less likely to have indexed dimensions that meet guideline criteria.
"The observation in this study that patients had a higher mortality once they developed any symptoms suggests that the presence of Class II criteria should prompt consideration of surgical intervention even if the patient has not yet developed symptoms," says Dr. Pellikka. "Aortic valve surgery was associated with improved outcome and should be considered at an earlier stage of left ventricular enlargement."
For more information
Yang LT, et al. Outcomes in chronic hemodynamically significant aortic regurgitation and limitations of current guidelines. Journal of the American College of Cardiology. 2019;73:1741.