Feb. 24, 2023
High-risk atherosclerotic plaque components are now recognized as important factors in the management of carotid atherosclerotic disease, even in cases of mild arterial narrowing. Mayo Clinic uses the latest imaging technology to evaluate carotid plaques, facilitating a distinctive approach to treatment.
Current guidelines consider the degree of luminal stenosis as the main criterion for intervention when managing individuals with carotid artery disease.
"But the evidence increasingly suggests that certain plaque features seen on imaging may be just as important as the actual degree of stenosis. These high-risk plaques may predispose patients to recurrent strokes, including embolic stroke of undetermined source," says John C. Benson, M.D., a neuroradiologist at Mayo Clinic in Rochester, Minnesota. "Limiting the assessment of atherosclerotic disease to the degree of stenosis is inadequate."
Lesión aterosclerótica carotídea con hemorragia intraplaca
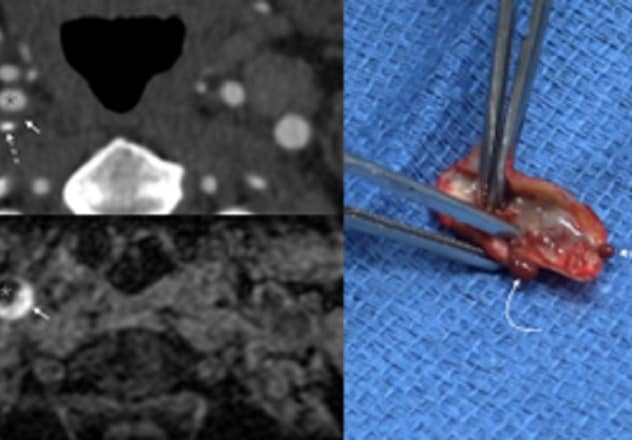
Lesión aterosclerótica carotídea con hemorragia intraplaca
Arriba a la izquierda, la angiografía por tomografía computarizada inicial muestra una placa no estenótica en la arteria carótida derecha de un paciente, con componentes blandos (flechas cortas) y calcificados (flecha larga discontinua). El asterisco indica el lumen del vaso. Abajo a la izquierda, la resonancia magnética (IRM) de seguimiento muestra una hemorragia intraplaca (flecha). El asterisco indica el lumen del vaso. A la derecha, la fotografía muestra una lesión aterosclerótica con hemorragia intraplaca (flechas) que se extirpó del paciente durante la endarterectomía carotídea. Los componentes sanguíneos podrían extraerse de la lesión extirpada.
Mayo Clinic uses MRI sequence magnetization-prepared rapid acquisition gradient echo (MPRAGE), in addition to CT angiography (CTA), to identify specific components of carotid plaques. Selected individuals whose stenosis is mild but whose imaging shows vulnerable plaques might be considered for carotid endarterectomy.
"Clinical management has lagged behind the major advances in our understanding of carotid atherosclerosis physiopathology," Dr. Benson says. "Imaging is advancing our knowledge and helping us to improve treatment."
Elucidating the role of plaque components
Mayo Clinic neuroradiologists are leading efforts to learn more about the role of carotid plaque components in atherosclerosis. In a review published in the February 2023 issue of the American Journal of Neuroradiology, Mayo Clinic researchers outlined the radiographic features that might be associated with embolic stroke of undetermined source.
Intraplaque hemorrhage is of particular interest. The results of a Mayo Clinic study suggest that in the setting of intraplaque hemorrhage, patients with mild stenosis might be at greater risk of future strokes.
As described in the July 2021 issue of the American Journal of Neuroradiology, the researchers found that carotid intraplaque hemorrhage was more likely to be observed in arteries with increasing degrees of luminal stenosis. At the same time, intraplaque hemorrhage was associated with symptoms in patients with less than 30% stenosis — but not in patients with greater stenosis.
"The presence of intraplaque hemorrhage might actually matter most in plaques that have minimal underlying stenosis," Dr. Benson says. "That's an interesting finding because historically, nonstenotic plaques haven't been treated, whether or not they have intraplaque hemorrhage."
Similarly, current guidelines support carotid endarterectomy for secondary stroke prevention only in cases of moderate or severe stenosis. But a Mayo Clinic study, published in the June 2022 issue of Stroke and Vascular Neurology, found that carotid endarterectomy is safe and well tolerated for certain individuals with nonstenotic carotid artery disease in the setting of vulnerable plaque. The procedures were performed at Mayo Clinic without significant complications and with excellent secondary stroke prevention for patients.
"Most of these patients underwent surgery after multiple recurrent ischemic events, despite intensive medical management," Dr. Benson says. "Our data strengthen the role of nonstenotic carotid artery disease in embolic strokes."
Other Mayo Clinic studies found:
- Low-density plaque components are more frequently present in patients with elevated total cholesterol or elevated low-density lipoprotein cholesterol — suggesting that cholesterol levels might be directly related to the formation of specific high-risk plaque features. That study was published in the June 2022 issue of The Neuroradiology Journal.
- The "rim sign" on CTA — characterized by soft-plaque components surrounded by a rind of thin adventitial calcification — has poor sensitivity and specificity for the detection of intraplaque hemorrhage. That study, published in the March 2022 issue of the Journal of Neuroradiology, was the first to assess the rim sign's capability with histologic confirmation of plaque tissue.
Improving CTA is another focus of research. Although CTA can show the degree of carotid stenosis and determine whether plaque is calcified or low density, it can't differentiate between intraplaque hemorrhage and lipid-rich necrotic core.
"We're looking for this holy grail of stroke imaging that can accurately characterize plaque on CTA because that's the imaging typically used in acute settings," Dr. Benson says. "The better we're able to provide real-time diagnostic imaging on that type of platform, the better we will be able to provide individualized medicine to patients who need it most."
For more information
Larson AS, et al. Nonstenotic carotid plaques and embolic stroke of undetermined source: A multimodal review. American Journal of Neuroradiology. 2023;44:118.
Larson AS, et al. Carotid intraplaque hemorrhage and stenosis: At what stage of plaque progression does intraplaque hemorrhage occur, and when is it most likely to be associated with symptoms? American Journal of Neuroradiology. 2021;42:1285.
Nardi V, et al. Carotid artery endarterectomy in patients with symptomatic non-stenotic carotid artery disease. Stroke and Vascular Neurology. 2022;7:251.
Benson JC, et al. Cardiovascular risk factors and cervical carotid plaque features on CT angiography. The Neuroradiology Journal. 2022;35:346.
Benson JC, et al. Reassessing the carotid artery plaque "rim sign" on CTA: A new analysis with histopathologic confirmation. American Journal of Neuroradiology. 2022;43:429.
Refer a patient to Mayo Clinic.