Breast lump or breast changes: Early evaluation is essential
A breast lump or breast changes need medical attention. Know what to expect during a clinical breast exam and what happens when a breast lump or change needs more study.
By Mayo Clinic Staff
Finding a breast lump or other change in a breast might cause worry about breast cancer.
Worry is common. Breast lumps also are common. But most breast lumps are not cancer. This is especially true for younger women. Breast lumps that are not cancer are called benign.
Still, have a healthcare professional look at any breast lump. Be sure to have a healthcare professional check a new lump or a lump that's still there after a month or two. Also see a healthcare professional if one breast doesn't feel the same as the other breast.
How breast tissue feels
Breast tissues include fat, glands and tissue that gives support, called connective tissue. Some breast-related symptoms, such as feeling tender or lumpy, change with the menstrual cycle. Extra fluid in the breasts during this time might cause lumps. Breast tissue also changes during pregnancy and menopause and while taking hormones.
When to contact a healthcare professional
Nipple changes
Nipple changes
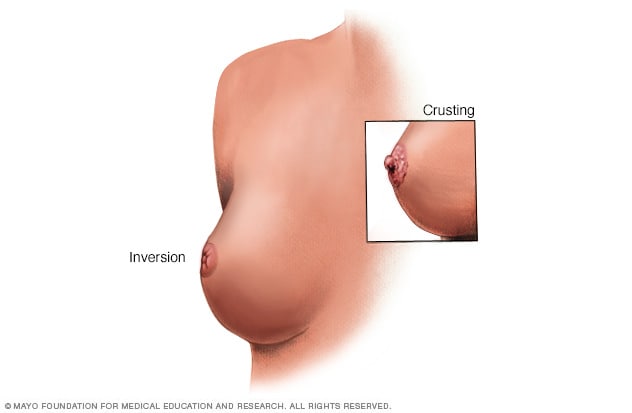
Nipple changes
Breast and nipple changes can be a sign of breast cancer. Make an appointment with your health care provider if you notice anything unusual.
Knowing how your breasts feel most of the time makes it easier to know when there's a change.
Reasons to talk with a healthcare professional include:
- Finding a new breast lump or thickness that doesn't feel the same as the tissue around it or the tissue in the other breast.
- Seeing a change in the size or shape of a breast or how it looks.
- Having pain in the breast, especially if it doesn't go away after the next period.
- Having skin changes on a breast or in the nipple area, such as itchiness, scaling, dimpling, puckering or redness. Redness may be harder to see on Black or brown skin.
- Having a nipple that suddenly turns inside out, called an inverted nipple.
- Seeing fluid come from the nipple, called discharge.
What to expect during a breast exam by a healthcare professional
Learning about a breast lump most often begins with a breast exam. During this exam, a healthcare professional:
- Asks about symptoms and risk factors for breast cancer or other breast conditions. The healthcare professional also asks about other types of cancer in the family, including ovarian, prostate, pancreatic and colon cancers.
- Looks at the breasts and lymph nodes in the armpit, feeling for lumps or any other changes.
- Looks at the skin on the breasts.
- Checks for nipple issues, such as turning inward, called inversion, or giving out fluid, called discharge.
If you have a breast lump or other area of concern, talk with your healthcare professional about testing.
Procedures to study a breast lump
Breast MRI
Breast MRI
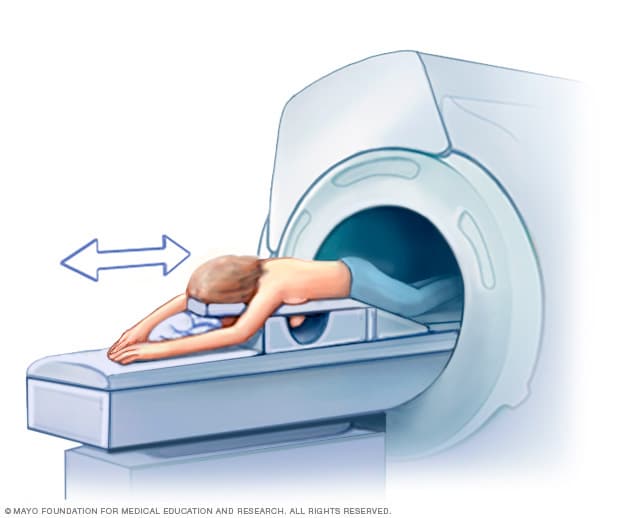
Breast MRI
Getting a breast MRI involves lying face down on a padded scanning table. The breasts fit into a hollow space in the table. The hollow space has coils that get signals from the MRI. The table slides into the large opening of the MRI machine.
Fine-needle aspiration
Fine-needle aspiration
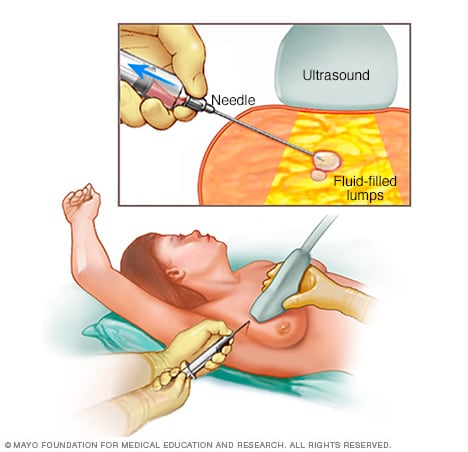
Fine-needle aspiration
During fine-needle aspiration, a healthcare professional puts a special needle into a breast lump and removes any fluid. This is called aspiration. The healthcare professional may use ultrasound to place the needle. An ultrasound is a procedure that uses sound waves to make pictures of the breast on a screen.
Core needle biopsy
Core needle biopsy
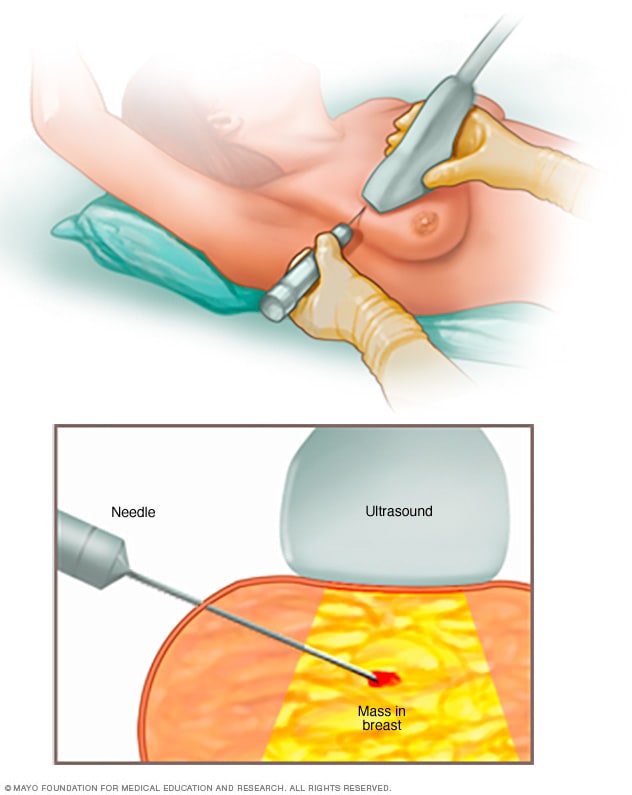
Core needle biopsy
A core needle biopsy uses a long, hollow tube to get a sample of tissue. Here, a biopsy of a suspicious breast lump is being done. The sample is sent to a lab for testing by doctors called pathologists. They specialize in the study of blood and body tissue.
Stereotactic breast biopsy
Stereotactic breast biopsy

Stereotactic breast biopsy
During a stereotactic breast biopsy, two plates firmly press the breast between them. X-rays called mammograms make pictures of the area from different angles. This finds the exact place for the biopsy. A health professional uses a needle to take a sample of breast tissue in the area of concern.
Imaging tests
Learning more about a breast lump may involve:
- Diagnostic mammogram. This specialized breast X-ray shows breast changes. It takes X-ray pictures from several angles.
- Breast ultrasound. Sound waves show pictures of the inside of the breast on a screen. Ultrasound imaging can show whether a breast lump is solid or filled with fluid.
- Breast MRI. An MRI uses a magnet and radio waves to make pictures of the inside of a breast. A breast MRI may help when the diagnosis isn't clear. Before a breast MRI, you might have a dye put into a vein in an arm. The dye helps tissues and blood vessels show up better on the MRI pictures.
Breast biopsy
This test involves a healthcare professional removing a tissue sample for study under a microscope. Ultrasound or mammography might help guide the needle. There might be a medicine to numb the area, called a local anesthetic.
Breast biopsy options include:
- Fine-needle aspiration biopsy. A healthcare professional uses a thin needle with a device to withdraw cells and fluid, called a syringe.
- Core needle biopsy. A healthcare professional uses a larger needle with a special tip to remove a sample of breast tissue.
- Stereotactic biopsy. Mammography makes pictures of the area in question from several angles, called stereo images. A healthcare professional then removes a sample of breast tissue with a needle.
- Vacuum-assisted biopsy. A healthcare professional uses a probe connected to a vacuum device to remove a small sample of breast tissue.
- Surgical excisional biopsy. A surgeon makes a small cut in the skin and breast tissue to remove part of or the whole lump.
Most often the radiologist doing the breast biopsy leaves a tiny clip or marker where the sample came from. This makes the area stand out on later imaging tests and marks the site for later surgery if it's needed.
After a biopsy, the tissue sample goes to a lab for study. A healthcare professional explains the results.
Follow-up after breast lump evaluation
If the breast lump isn't cancer, a healthcare professional decides if you need to have breast exams more often or repeat breast imaging within the year to look for other changes on the mammogram. Your healthcare professional may ask you to return in 2 to 3 months to see if there are changes in your breast.
Tell your healthcare professional if you see changes in the lump or get new areas of concern. Even if you had a recent mammogram that looked OK, have your healthcare professional look at any new breast changes.
If it's not clear whether the breast lump is cancer, you may need to see a surgeon or other specialist. A diagnosis might not be clear, for instance, when a clinical breast exam and a mammogram show areas of concern but the biopsy shows no cancer.
A breast lump that's cancer needs treatment. Treatment depends on the tumor type and other factors.
April 03, 2025
- Sabel MS. Clinical manifestations, differential diagnosis, and clinical evaluation of a palpable breast mass. https://www.uptodate.com/content/search. Accessed March 18, 2025.
- Breast health: Follow-up after an abnormal mammogram. National Cancer Institute. https://www.cancer.gov/types/breast/breast-changes. Accessed March 18, 2025.
- Malherbe F, et al. Palpable breast lump: An age-based approach to evaluation and diagnosis. South African Family Practice. 2022; doi:10.4102/safp.v64i1.5571.
- Breast masses (breast lumps). Merck Manual Professional Version. https://www.merckmanuals.com/professional/gynecology-and-obstetrics/breast-disorders/breast-masses-breast-lumps?query=breast%20masses. Accessed March 19, 2025.
- Vacuum-assisted core biopsy. National Cancer Institute. https://www.cancer.gov/publications/dictionaries/cancer-terms/def/vacuum-assisted-core-biopsy. Accessed March 19, 2025.
- Stereotactic breast biopsy. RadiologyInfo.org. https://www.radiologyinfo.org/en/info/breastbixr. Accessed March 19, 2025.
Advertisement
Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission.
Advertising & Sponsorship
Mayo Clinic Press
Check out these best-sellers and special offers on books and newsletters from Mayo Clinic Press.
.