Overview
Posterior vaginal prolapse (rectocele)
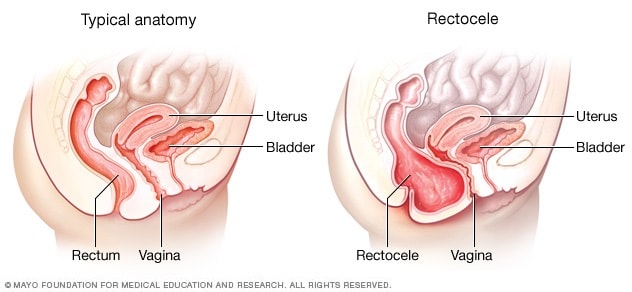
Posterior vaginal prolapse (rectocele)
Posterior vaginal prolapse, also known as a rectocele, is when the wall of tissue that separates the rectum from the vagina weakens or tears. When this happens, tissues or structures just behind the vaginal wall — in this case, the rectum — can bulge into the vagina.
A posterior vaginal prolapse is a type of pelvic organ prolapse. It happens when the tissue between the rectum and vagina weakens or tears. This can cause tissue from the rectum to push into the vagina, creating a bulge. Posterior vaginal prolapse also is called a rectocele (REK-toe-seel).
A rectocele can be caused by tears during childbirth, long-term straining with bowel movements and other activities that put pressure on pelvic tissues. A small rectocele might not cause symptoms.
A large rectocele can cause tissue to bulge through the vagina. To pass stool, you might need to support the vaginal wall with your fingers. This is called splinting. The bulge can be uncomfortable or cause you to feel like you can't completely empty your rectum during bowel movements. But it's rarely painful.
Treatment for posterior vaginal prolapse often is based on the person's symptoms and how much the symptoms affect daily life. Many people may benefit from self-care and other nonsurgical options. Some people with more severe posterior vaginal prolapse may have surgery.
Products & Services
Symptoms
A small posterior vaginal prolapse, also called a rectocele, might not cause symptoms.
Symptoms you may notice include:
- A soft bulge of tissue in the vagina that might come through the opening of the vagina.
- Trouble having a bowel movement.
- Feeling pressure or fullness in the rectum.
- Feeling as if the rectum isn't completely empty after a bowel movement.
- Needing to support the vaginal wall with your fingers to pass stool. This is called splinting.
If you have posterior vaginal prolapse, you also may have prolapse of other pelvic organs, such as the bladder or uterus. During a pelvic exam, a healthcare professional can look at the prolapse and talk about ways to manage the symptoms.
When to see a doctor
Sometimes, posterior vaginal prolapse doesn't cause symptoms. But moderate or severe posterior vaginal prolapse might be uncomfortable. See a healthcare professional if your symptoms bother you or get worse.
Causes
Posterior vaginal prolapse, also called a rectocele, is caused when the tissue that separates your rectum and vagina weakens. This can happen for many reasons, including:
- Vaginal childbirth. Childbirth can cause birth-related tears and put strain and pressure on the pelvic floor. Medical tools such as forceps that are used during birth also may damage pelvic floor muscles and supporting tissues.
- Long-lasting straining. Straining to have a bowel movement can weaken pelvic floor tissues over time.
- Increased pelvic floor pressure. Anything that puts pressure on the pelvic floor for a long time may cause a rectocele. This may include a long-lasting cough or bronchitis, being overweight, or heavy lifting.
Pregnancy and childbirth
Many of the muscles, ligaments and tissues that support the vagina are stretched during pregnancy, labor and delivery. This can make those tissues weaker and less supportive. The more pregnancies you have, the more likely you are to have posterior vaginal prolapse.
You're less likely to have posterior vaginal prolapse if you've had only cesarean deliveries. But you still could develop the condition.
Risk factors
Posterior vaginal prolapse, also called a rectocele, can happen to anyone who has a vagina. However, some things may increase risk, such as:
- Genetics. Some people are born with weaker connective tissues in the pelvic area. This makes them more likely to develop posterior vaginal prolapse.
- Vaginal childbirth. Having several vaginal births can increase the risk of posterior vaginal prolapse. If you had tearing or needed a small cut — called an episiotomy — to help with delivery, that also can increase the risk. Also, the use of tools such as forceps to help with delivery is linked to a higher chance of posterior vaginal prolapse.
- Aging. Pelvic floor issues such as a rectocele are more common with age. That's because growing older causes the loss of muscle mass, elasticity and nerve function. This can cause muscles to stretch or weaken.
- Menopause. Women who have gone through menopause are more likely to have posterior vaginal prolapse. Hormone changes that happen during menopause can weaken connective tissues in the pelvic area.
- Overweight and obesity. Extra body weight places stress on pelvic floor tissues and increases the risk of posterior vaginal prolapse.
Prevention
Posterior vaginal prolapse, also called a rectocele, can't always be prevented. But you can try some things to keep it from getting worse:
- Do Kegel exercises regularly. These exercises can strengthen pelvic floor muscles, which support the bladder, rectum and uterus.
- Treat and prevent constipation. Drink plenty of fluids and eat high-fiber foods, such as fruits, vegetables, beans and whole-grain cereals. Fiber helps prevent constipation and straining, which may reduce the risk of a rectocele.
- Avoid heavy lifting and lift correctly. Use your legs instead of your waist or back to lift.
- Control coughing. Get treatment for a chronic cough or bronchitis.
- Maintain a healthy weight. Ask your healthcare professional about the best weight for you. Ask for help losing weight, if needed.
- Quit smoking. Smoking may cause a long-term cough, which can stress pelvic floor muscles. Talk to your healthcare professional if you need help quitting smoking.