Overview
Myasthenia gravis is a condition that happens when communication between nerves and muscles breaks down. This causes muscles to feel weak and get tired quickly. This condition may affect any of the muscles you control, called voluntary muscles. Certain muscle groups are more commonly affected than others. These include muscles in the face, throat, arms and legs.
Your eyelids may droop, you may have double vision, trouble speaking or eating, or you may have trouble holding up your head because of weak neck muscles. Myasthenia gravis can happen at any age. But it's more common in people younger than 40 who were assigned female at birth and people older than 60 who were assigned male at birth.
There's no way to prevent or cure myasthenia gravis. But treatment can help manage symptoms.
Products & Services
Symptoms
Symptoms of myasthenia gravis may come and go. They usually get better when the weak muscle is rested but get worse again when the muscle is used. Symptoms often progress and may be at their worst one or two years after the disease begins.
Common symptoms of muscle weakness with myasthenia gravis include:
Eye muscles
In more than half of people with myasthenia gravis, the first symptoms involve eye muscles, such as:
- Drooping of one or both eyelids, called ptosis.
- Double vision, called diplopia. This may affect the horizontal or vertical vision. It may improve or stop when one eye is closed.
Face and throat muscles
In about 15% of people with myasthenia gravis, the first symptoms involve face and throat muscles. It may be hard to:
- Speak. Your speech might sound soft or nasal, depending on which muscles are affected.
- Swallow. You may choke easily, making it difficult to eat, drink or take pills. At times, when you swallow liquid, it may come out of your nose.
- Chew. The muscles used for chewing might tire halfway through a meal. This is especially true if you've been eating something hard to chew, such as steak.
- Control facial expressions. For example, you might have trouble fully raising your eyebrows or holding a smile because the muscles tire quickly. Your facial expression may not fully reflect what you are feeling.
Neck and limb muscles
Myasthenia gravis also may cause weakness in the neck, arms and legs. These symptoms may happen later as the condition worsens. Weakness in the legs can affect how you walk. Weak neck muscles can make it hard to hold up the head.
When to see a doctor
Talk with your healthcare professional if you have trouble with any of the following:
- Breathing.
- Vision.
- Swallowing.
- Chewing.
- Walking.
- Using your arms or hands.
- Holding up your head.
Causes
The exact cause of myasthenia gravis is not known. Myasthenia gravis is an autoimmune condition. These conditions happen when the immune system creates antibodies that mistakenly work against or attack healthy cells or tissue. Antibodies are proteins that help fight unhealthy or foreign substances in the body, such as bacteria or viruses.
Antibodies
Receptors
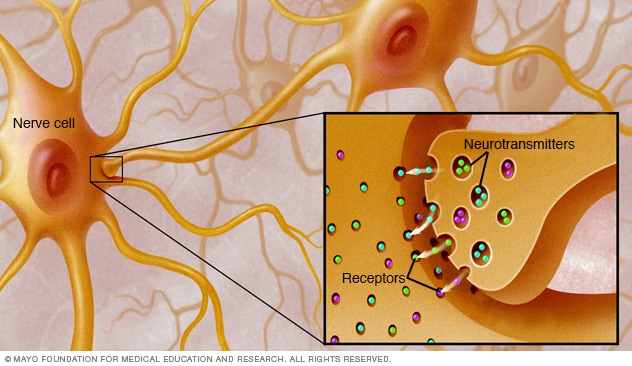
Receptors
Chemical messengers called neurotransmitters fit precisely into receptor sites on muscle cells. In myasthenia gravis, certain receptor sites are blocked or destroyed, causing muscle weakness.
In myasthenia gravis, the immune system mistakenly makes antibodies that stop the neurotransmitter acetylcholine from communicating with muscles.
Nerves communicate with muscles by releasing chemicals called neurotransmitters that send signals between cells.
The antibodies destroy or block the path to muscle cells called receptor sites. With fewer receptor sites available, the muscles receive fewer nerve signals. This causes muscle weakness.
Myasthenia gravis also may happen if antibodies block proteins such as muscle-specific receptor tyrosine kinase, also called MuSK, or lipoprotein-related protein 4, also called LRP4. These proteins work together to form strong connections between nerve cell signals and muscles. When antibodies block MuSK or LRP4, the signal between nerves and muscles is limited or does not get through, leading to muscle weakness. Research likely will continue to find other antibodies that play a role in myasthenia gravis.
Myasthenia gravis is not always caused by antibodies that block acetylcholine, MuSK or LRP4. A type of myasthenia gravis called seronegative myasthenia gravis is known as antibody-negative myasthenia gravis. In general, researchers believe this type of myasthenia gravis still happens because of issues with the immune system, but the antibodies involved are not yet known.
Thymus gland
Thymus gland
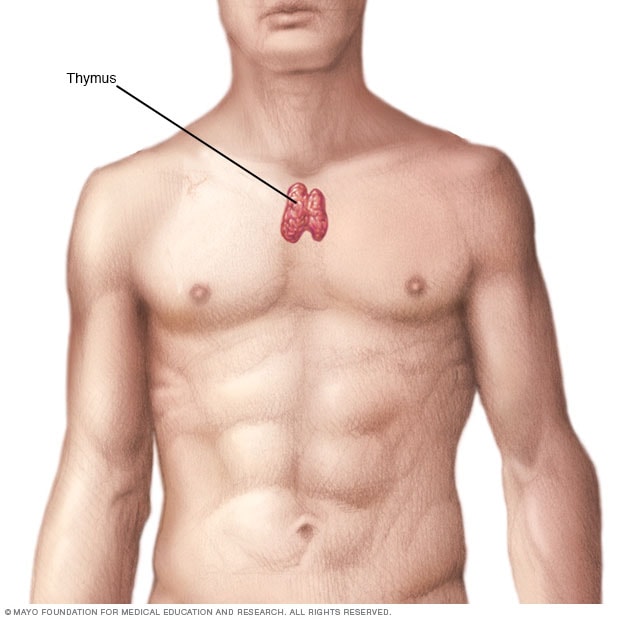
Thymus gland
The thymus gland, a part of the immune system, is in the upper chest beneath the breastbone. The thymus may trigger or support the production of antibodies that result in muscle weakness.
Researchers believe the thymus gland makes or helps make the antibodies that block acetylcholine. The thymus gland is part of the immune system. It is located in the upper chest beneath the breastbone.
The thymus gland is large in babies and small in adults who don't have health conditions. In some adults with myasthenia gravis, the thymus gland is larger than usual. Some people with myasthenia gravis also have tumors of the thymus gland. These tumors are called thymomas. Thymomas are cancer, but they usually aren't malignant. This means the cancer typically does not spread throughout the body. These tumors may be removed with surgery.
Other causes
Children born to people with myasthenia gravis may rarely have the condition at birth. This is called neonatal myasthenia gravis. If treated immediately, children usually recover within two months after birth.
Some children are born with a rare hereditary form of myasthenia gravis called congenital myasthenic syndrome. Congenital myasthenic syndrome is often treated with medicine to manage symptoms.
Factors that can make myasthenia gravis worse include:
- Fatigue.
- Illness or infection.
- Surgery.
- Stress.
- Some medicines:
- Beta blockers.
- Quinidine gluconate, quinine sulfate (such as Qualaquin).
- Phenytoin (such as Dilantin).
- Some anesthetics and antibiotics.
- Pregnancy.
- Menstrual periods.
Risk factors
While the exact cause of myasthenia gravis is not fully understood, certain factors may increase the likelihood of having it.
- Genetics. A personal or family history of autoimmune conditions may put you at higher risk.
- Thymus gland issues. Having an enlarged thymus or a thymoma may play a role in myasthenia gravis.
- Age and sex assigned at birth. Myasthenia gravis is more common in people younger than 40 who were assigned female at birth, and in people older than 60 who were assigned male at birth.
- Lifestyle and health. Stress, infections and some medicines may trigger the condition in some people.
These factors increase the risk but do not mean you will get myasthenia gravis.
Complications
Complications of myasthenia gravis are treatable, but some can be life-threatening.
Myasthenic crisis
Myasthenic crisis is a life-threatening condition. It happens when the muscles that control breathing become too weak to work. Emergency treatment and mechanical assistance with breathing are needed. Medicines and therapies that filter the blood help people breathe on their own.
Thymus gland tumors
Some people with myasthenia gravis have tumors in their thymus glands. The thymus gland lies under the breastbone and is part of the immune system. Most of these tumors, called thymomas, are not malignant, meaning they likely will not spread and can be removed with surgery.
Other conditions
People with myasthenia gravis often have other autoimmune conditions, such as:
- Thyroid disease. The thyroid is a gland located in the neck that helps manage metabolism. Metabolism is how the body uses energy. If your thyroid is too active or not active enough, you may have a hard time managing body temperature and weight and you may have other symptoms.
- Rheumatoid arthritis. This condition causes inflammation and pain, typically in the bones of joints.
- Lupus. In this condition, the immune system attacks healthy tissues throughout the body. This can damage the skin, joints, kidneys, heart and brain. Symptoms range from mild, such as fatigue, joint pain and skin rashes, to severe, such as kidney inflammation or cardiovascular issues.
Aug. 22, 2025