Sept. 21, 2021
Mayo Clinic has developed 3D-printed models of pediatric cerebrovascular lesions to optimize training with respect to these rare conditions. The models clarify the relationships between the various lesions and adjacent anatomical structures, to better prepare trainee neurosurgeons for future cases.
Convertir 2D a 3D

Convertir 2D a 3D
Una resonancia magnética T2 axial, una angiografía por tomografía computarizada, una angiografía por resonancia magnética con proyección de máxima intensidad y una angiografía por sustracción digital muestran una malformación arteriovenosa del cerebelo en una niña de 10 años.
"One of the biggest challenges for a junior neurosurgeon is developing 3D visualization — the ability to turn a series of neuroimages into a mental image in three dimensions," says Christopher S. Graffeo, M.D., a researcher in Neurosurgery at Mayo Clinic in Rochester, Minnesota. "A 3D-printed model can be viewed from different angles and turned around in the surgeon's hands. Adding a tactile object to a simple visual object gives a much more sophisticated perspective."
Pediatric cerebrovascular lesions are challenging to treat. Most tertiary referral centers treat only one or two pediatric patients with aneurysms a year — and typically fewer children with arteriovenous malformations (AVMs) or vein of Galen malformations (VOGMs).
"Due to the rarity and complexity of these lesions, it's difficult to train the next generation of neurosurgeons on the nuances of treating them," says David J. Daniels, M.D., Ph.D., a pediatric neurosurgeon at Mayo Clinic in Rochester, Minnesota. "Children's blood vessels are also much smaller, further adding to the complexity. A better understanding of the overall anatomy is very valuable in this setting."
Mayo Clinic's 3D-printed models depict an aneurysm, an AVM and a VOGM in three pediatric patients who were treated at Mayo Clinic. The models were created in Mayo Clinic's additive manufacturing facility, the largest point-of-care 3D printing facility in the United States.
In a subjective survey, a group of neurosurgical residents reviewed the models and case materials from the pediatric patients. All reviewers reported enhanced understanding of pediatric cerebrovascular diseases after incorporating the 3D models into their training.
"Our point-of-care manufacturing facility gives the neurosurgeon and neurosurgical trainees patient-specific, life-sized, 3D physical models. We spend our whole lives interacting with 3D objects, and thus no translation is needed," says Jonathan M. Morris, M.D., a neuroradiologist and medical director of the 3D Anatomic Modeling Laboratory at Mayo Clinic in Rochester, Minnesota. "For example, if the patient is an infant, the skull is going to fit inside the surgeon's hand. If the patient is 17 years old, the surgeon will need both hands to hold the skull. But both skulls may look the same size on a screen."
Gold standard manufacturing
At Mayo Clinic, patients with cerebrovascular lesions typically have CT and MRI scans, MR angiogram and often a cerebral angiogram.
Combinación de lo táctil y lo visual
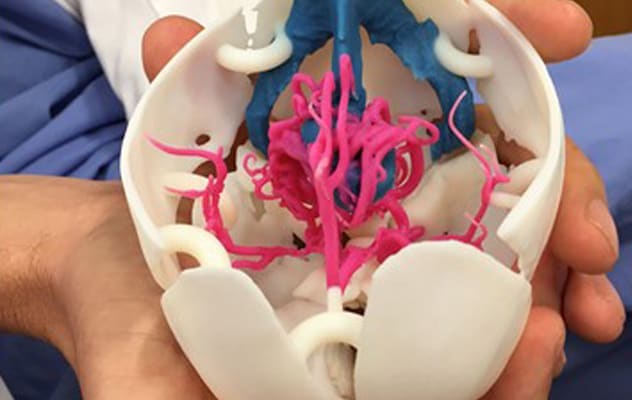
Combinación de lo táctil y lo visual
La foto muestra el modelo impreso en 3D de Mayo Clinic de malformaciones de la vena de Galeno en un bebé de 3 años.
Modelo impreso en 3D
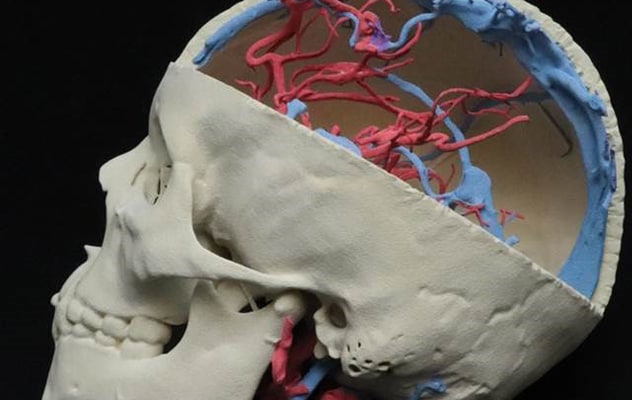
Modelo impreso en 3D
Usando software de diseño asistido por computadora, las cuatro modalidades de imágenes se registraron de forma conjunta y se segmentó la anatomía relevante para crear el modelo impreso en 3D.
"Combining those four specific data sets in the mind to create a patient-specific 3D model is very difficult," Dr. Morris says. "But using computer-aided design software to coregister the varied imaging data sets to one another allows us to print a life-sized model."
Mayo Clinic's manufacturing facility provides the benefit of close collaboration among neuroradiologists, engineers and neurosurgeons. "We have most of the available technologies for 3D printing in-house, just above the operating room," Dr. Morris says. "Neurosurgeons can come during normal working hours and have access to this technology, the imaging expertise of neuroradiologists and the design expertise of engineers. We have all the necessary resources and understanding to work across all of these disciplines to make gold standard diagnostic, patient-specific models for preoperative planning."
Mayo Clinic researchers are using this expertise to develop additional types of 3D-printed models. One example is 3D-printed aneurysms that contain lumens. "We can place the model aneurysm in a plastic brain in a plastic skull for simulated aneurysm surgery," Dr. Graffeo says.
Another effort involves 3D-printed models with arteries that can be perfused with imitation blood. "The arteries could be used in the lab to simulate an aneurysm rupture, as part of neurosurgical training," Dr. Graffeo says. "Our goal, in addition to providing optimal patient care, is to help new neurosurgeons to move more quickly through the learning curve."