Diagnosis
To diagnose mitral valve regurgitation, a health care professional does a physical exam and asks questions about your symptoms and medical history. A device called a stethoscope is used to listen to the heart and lungs. If you have mitral valve regurgitation, a whooshing sound called a murmur may be heard. The mitral valve heart murmur is the sound of blood leaking backward through the valve.
Tests may be done to confirm a diagnosis of mitral valve regurgitation or to check for other conditions that can cause similar symptoms.
Tests
 Echocardiogram
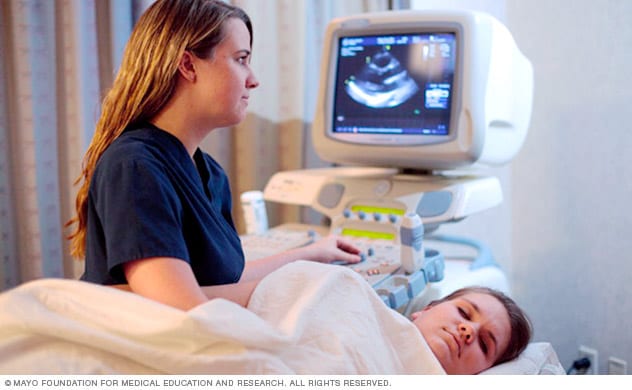
Echocardiogram
A health care professional performs an echocardiogram at Mayo Clinic.
Common tests to diagnose mitral valve regurgitation include:
-
Echocardiogram. Sound waves are used to create pictures of the beating heart. An echocardiogram shows the structure of the mitral valve and blood flow in the heart. A standard echocardiogram is called a transthoracic echocardiogram (TTE). It can confirm a diagnosis of mitral valve regurgitation. The test also can tell how severe the condition is. Echocardiography also can help diagnose congenital mitral valve disease, rheumatic mitral valve disease and other heart valve conditions.
Sometimes, a more-detailed echocardiogram is needed to better see the mitral valve. This test is called a transesophageal echocardiogram (TEE). A TEE creates pictures of the heart from inside the body.
- Electrocardiogram (ECG). This test shows how the heart is beating. Sticky patches called sensors are attached to the chest and sometimes the arms and legs. Wires connect the patches to a computer, which displays or prints results. An ECG can show irregular heart rhythms related to mitral valve disease.
- Chest X-ray. A chest X-ray shows the condition of the heart and lungs. This quick test can help diagnose an enlarged heart or fluid in the lungs.
- Cardiac MRI. This test uses magnetic fields and radio waves to create detailed pictures of the heart. Cardiac MRI may help show the severity of mitral valve regurgitation. The test also gives details about the lower left heart chamber.
- Exercise tests or stress tests. These tests often involve walking on a treadmill or riding a stationary bike while the heart is checked. Exercise tests show how the heart reacts to physical activity. The tests can show whether mitral valve regurgitation symptoms occur during exercise. If you can't exercise, you might be given medicine that makes the heart work like exercise does.
- Cardiac catheterization.This test isn't often used to diagnose mitral valve disease. But it can be helpful if other tests haven't diagnosed the condition. A doctor guides a thin, flexible tube called a catheter through a blood vessel in the arm or groin. It's moved to an artery in the heart. Dye flows through the tube. This makes the arteries in the heart chambers show up more clearly on X-rays taken during the test.
Staging
After testing confirms a diagnosis of mitral or other heart valve disease, your health care team may tell you the stage of disease. Staging helps determine the most appropriate treatment.
The stage of heart valve disease depends on many things, including symptoms, disease severity, the structure of the valve or valves, and blood flow through the heart and lungs.
Heart valve disease is staged into four basic groups:
- Stage A: At risk. Risk factors for heart valve disease are present.
- Stage B: Progressive. Valve disease is mild or moderate. There are no heart valve symptoms.
- Stage C: Asymptomatic severe. There are no heart valve symptoms, but the valve disease is severe.
- Stage D: Symptomatic severe. Heart valve disease is severe and is causing symptoms.
Outlook
How well a person does after being diagnosed with mitral valve regurgitation varies. This is called the outlook, also called prognosis. The outlook for mitral valve regurgitation depends on:
- The cause of the mitral valve disease.
- The stage of heart valve disease.
- The severity of regurgitation.
- How long the condition has been present, also called the duration.
More Information
Treatment
The goals of mitral valve regurgitation treatment are to:
- Help the heart work better.
- Reduce symptoms.
- Prevent complications.
Some people, especially those with mild regurgitation, might not need treatment. Your health care team considers your symptoms and stage of regurgitation, among other things, when planning treatment.
Treatment of mitral valve regurgitation may include:
- Healthy lifestyle changes.
- Regular health checkups.
- Medicines to treat symptoms and prevent complications, such as blood clots.
- Surgery to repair or replace the mitral valve.
A doctor trained in heart diseases typically provides care for people with mitral valve regurgitation. This type of health care professional is called a cardiologist.
If you have mitral valve regurgitation, consider being treated at a medical center with a multidisciplinary team of health care professionals trained and experienced in evaluating and treating heart valve disease.
Medications
Medicines may be needed to reduce mitral valve regurgitation symptoms and to prevent complications of heart valve disease.
Types of medicines that may be used for mitral valve regurgitation include:
- Water pills, also called diuretics. This medicine reduces or prevents fluid buildup in the lungs and other parts of the body.
- Blood thinners, also called anticoagulants. If you have atrial fibrillation due to mitral valve disease, such as mitral valve regurgitation, your health care team may recommend these medicines to prevent blood clots. Atrial fibrillation increases the risk of blood clots and stroke.
- Blood pressure medicines. High blood pressure makes mitral valve regurgitation worse. If you have mitral valve regurgitation and high blood pressure, you may be given medicines to lower blood pressure.
Surgery or other procedures
A diseased or damaged mitral valve might eventually need to be repaired or replaced, even if you don't have symptoms. Surgery for mitral valve disease includes mitral valve repair and mitral valve replacement. Your health care team discusses the risks and benefits of each type of heart valve with you to determine which valve may be best for you.
If you need surgery for another heart condition, a surgeon might perform mitral valve repair or replacement at the same time as that other surgery.
Mitral valve surgery is usually done through a cut in the chest. Surgeons at some medical centers sometimes use robot-assisted heart surgery, a minimally invasive procedure in which robotic arms are used to do the surgery.
Robot-assisted minimally invasive mitral valve repair at Mayo Clinic
In robot-assisted mitral valve repair surgery at Mayo Clinic, two board-certified cardiac surgeons use robotic equipment to perform the exact same procedure conducted in traditional open chest heart surgery, without needing to make a large incision through your breast bone. Your surgeons perform the procedure through small incisions in your right chest, using finger-sized instruments that are slipped in between your ribs. In this procedure, one surgeon sits at a remote console and views your heart using a magnified high-definition 3D view on a video monitor. Another surgeon works at the operating table and ensures the safe movement of the robotic arms. You'll need to be supported by a heart-lung bypass machine during the procedure. This will allow your surgeons to stop your heart briefly and insert instruments into the inner chambers to repair the mitral valve. Your surgeon uses robotic arms to duplicate specific maneuvers used in open-chest surgeries. The procedure is performed through small openings in your chest, through which will be inserted micro instruments and a thin high-definition camera tube or thoracoscope. One opening will be a mini working port through which surgeons will insert materials used during the procedure. Your surgeon performs the procedure from the remote console. Your surgeon's hand movements are translated precisely to the robotic arms at the operating table, which move like a human wrist. At the operating table, another surgeon works together with the surgeon at the console to perform the procedure and ensure it is conducted safely and efficiently. Your surgeon at the console can closely examine the complicated mitral valve problem using the high-definition 3D video monitor. This allows your surgeon to have a clearer, more lifelike perspective of your heart than is possible during open heart surgery, in which surgeons view the heart from a further distance.
To repair the mitral valve, your surgeon makes an incision in the left upper chamber or left atrium of your heart to access the mitral valve. Your surgeon can then identify the problem with your mitral valve and repair the valve itself. In mitral valve prolapse, the mitral valve, located between your heart's left atrium and the left lower chamber or left ventricle, doesn't close properly. The leaflets of the valve bulge or prolapse upward or back into the left atrium as your heart contracts. This leads to blood leaking backward into the left atrium, a condition called mitral valve regurgitation. To repair this condition, various complicated technical procedures are performed. Sometimes a small section of the leaflet, the part of the valve that doesn't close properly, is identified, and a triangular section is removed, as shown. Your surgeon then stitches the cut edges of the leaflet together to repair the valve.
In other cases, new chords or chordae supporting the broken leaflet are inserted. An annuloplasty band is then placed around the circumference of the valve to stabilize the repair. Your surgeon will close the incisions in your chest after the procedure. Mayo's staff will assist you during your recovery over a three-day period in the hospital. In robot-assisted heart surgery, most people have a quicker recovery, smaller incisions, and less pain than following open-chest surgery. Studies have also found that this procedure performed at Mayo Clinic is cost effective, with similar or lower total costs compared with traditional open-chest surgery.
Mitral valve repair
Mitral valve repair
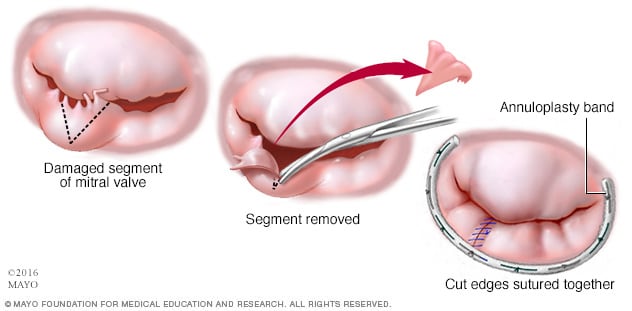
Mitral valve repair
In mitral valve repair, the surgeon removes and repairs part of the damaged mitral valve to allow the valve to fully close and stop leaking. The surgeon may tighten or reinforce the ring around a valve, called the annulus, by placing an artificial ring called an annuloplasty band.
Mitral valve repair
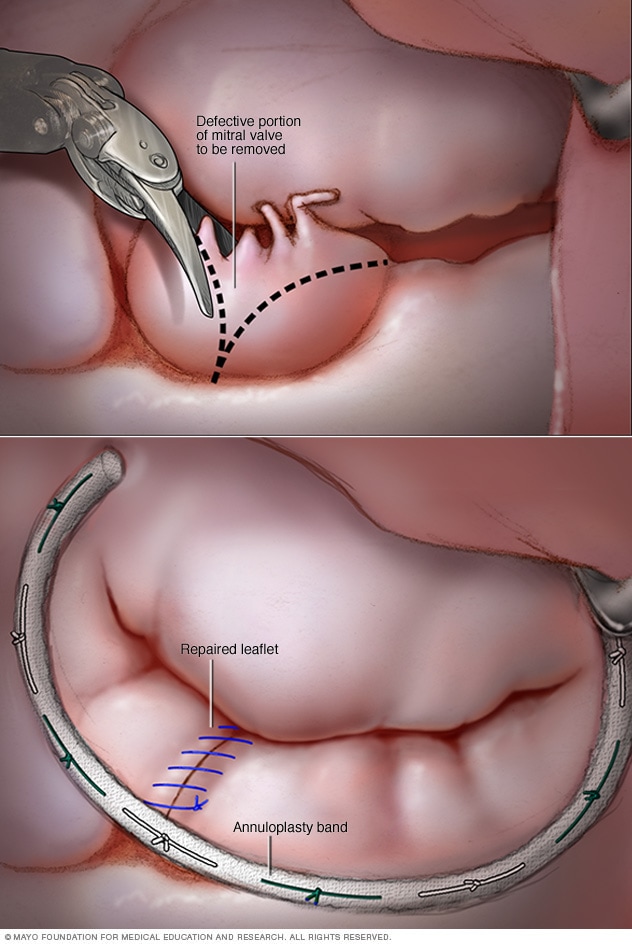
Mitral valve repair
In mitral valve repair, a surgeon removes the part of the mitral valve that doesn't close properly, as shown in the top image. Then the surgeon sutures together the edges and places an annuloplasty band to support the valve, as shown in the bottom image.
Mitral valve repair saves the existing valve and may save heart function. Whenever possible, mitral valve repair is recommended before considering valve replacement. People who have mitral valve repair for mitral regurgitation at an experienced medical center generally have good outcomes.
During mitral valve repair surgery, the surgeon might:
- Patch holes in a heart valve.
- Reconnect the valve flaps.
- Remove excess tissue from the valve so that the flaps can close tightly.
- Repair the structure of the mitral valve by replacing cords that support it.
- Separate valve leaflets that have connected.
Other mitral valve repair procedures include:
- Annuloplasty. A surgeon tightens or reinforces the ring around the valve, called the annulus. Annuloplasty may be done with other techniques to repair a heart valve.
- Valvuloplasty. This treatment is used to repair a mitral valve with a narrowed opening. It might be done even if you don't have symptoms. It's done using a thin tube called a catheter with a balloon on the tip. The surgeon inserts the tube into an artery in the arm or groin and guides it to the mitral valve. The balloon is inflated, widening the mitral valve opening. The balloon is then deflated, and the catheter and balloon are removed.
- Mitral valve clip. In this treatment, a doctor guides a catheter with a clip on its end to the mitral valve through an artery in the groin. The clip is used to improve the closure of the mitral valve leaflets. It reduces the amount of regurgitation. This procedure is an option for people who have severe mitral valve regurgitation or who aren't good candidates for mitral valve surgery.
Mitral valve replacement
Repair of previously replaced valve
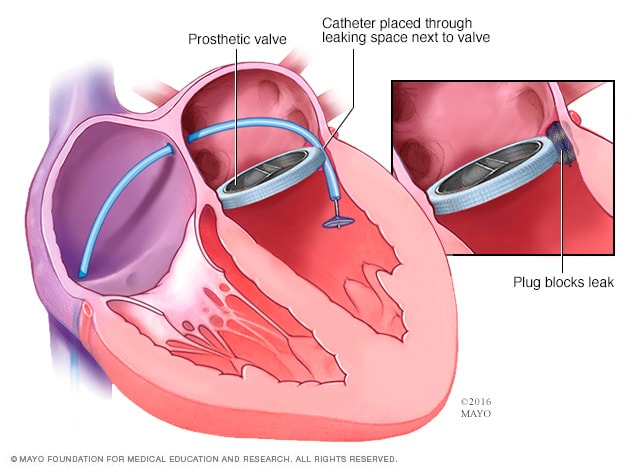
Repair of previously replaced valve
If a previously replaced mitral valve has a leak surrounding the artificial valve, a cardiologist may insert a device to stop the leak.
During mitral valve replacement, the surgeon removes the mitral valve. It's replaced with a mechanical valve or a valve made from cow, pig or human heart tissue. A tissue valve also is called a biological tissue valve.
Sometimes, a heart catheter procedure is done to put a replacement valve into a biological tissue valve that no longer works well. This is called a valve-in-valve procedure.
If you had mitral valve replacement with a mechanical valve, you need to take blood thinners for life to prevent blood clots. Biological tissue valves break down over time and usually need to be replaced.
Mayo Clinic Minute: Mitral valve clip
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Your health care team may suggest that you make several heart-healthy lifestyle changes. Take these steps:
- Manage blood pressure. Control of high blood pressure is important if you have mitral valve regurgitation.
- Eat a heart-healthy diet. Food doesn't directly affect mitral valve regurgitation. But a healthy diet can help prevent other heart disease that can weaken the heart muscle. Eat foods that are low in saturated and trans fats, sugar, salt, and refined grains, such as white bread. Eat a variety of vegetables and fruits, whole grains, and proteins, such as lean meats, fish and nuts.
- Get regular exercise. How long and hard you're able to exercise can depend on whether you have mild, moderate or severe mitral valve regurgitation. Talk with your health care team about the amount and type of exercise that's best for you, especially if you're considering competitive sports.
- Maintain a healthy weight. Being overweight increases the risk of heart disease. Talk with a health care professional to set realistic goals for body mass index and weight.
- Prevent infective endocarditis. If you've had mitral valve replacement, your doctor will likely recommend that you take antibiotics before dental procedures to prevent an infection called infective endocarditis.
- Avoid or limit alcohol. Heavy alcohol use can cause irregular heartbeats and can make your symptoms worse. Excessive alcohol use also can cause a weakened heart muscle that leads to mitral regurgitation. Ask your health care team about the effects of drinking alcohol.
- Avoid tobacco. If you smoke, quit. Ask your health care team about resources to help you quit smoking. Joining a support group may be helpful.
- Practice good sleep habits. Poor sleep may increase the risk of heart disease and other chronic conditions. Go to bed and wake at the same time every day, including on weekends. If you have trouble sleeping, talk with a health care professional about strategies that might help.
If you have mitral valve regurgitation and are thinking about getting pregnant, talk with your health care team first. Pregnancy causes the heart to work harder. How a heart with mitral valve regurgitation tolerates this extra work depends on the degree of regurgitation and how well the heart pumps.
Preparing for your appointment
If you think you have mitral valve regurgitation, make an appointment to see a health care professional. Here's some information to help you prepare for your appointment.
What you can do
- Be aware of pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do beforehand.
- Write down your symptoms, including any that seem unrelated to mitral valve regurgitation.
- Write down important personal information, including a family history of heart disease, heart problems present from birth, genetic conditions, stroke, high blood pressure or diabetes, and any major stresses or recent life changes.
- Make a list of all medications, vitamins and supplements you take. Include the dosages.
- Take a family member or friend along, if possible, to help you remember information you receive.
- Be prepared to discuss your diet and exercise habits. . If you don't already eat well and exercise, be ready to talk with your health care team about challenges you might face in getting started.
- Write down questions to ask your health care team.
For mitral valve regurgitation, some basic questions to ask a health care professional include:
- What is likely causing my condition?
- What are other possible causes for my symptoms?
- What tests will I need?
- What's the best treatment?
- What are other treatment options?
- I have other health conditions. How can I best manage them together?
- Are there restrictions I need to follow?
- If I need surgery, which surgeon do you recommend for mitral valve repair?
- Are there brochures or other printed material I can take with me? What websites do you recommend?
Don't hesitate to ask other questions you have.
What to expect from your doctor
Your health care team is likely to ask you many questions, including:
- When did your symptoms begin?
- Are your symptoms constant or do they come and go?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Sept. 19, 2023