Overview
Prostate gland
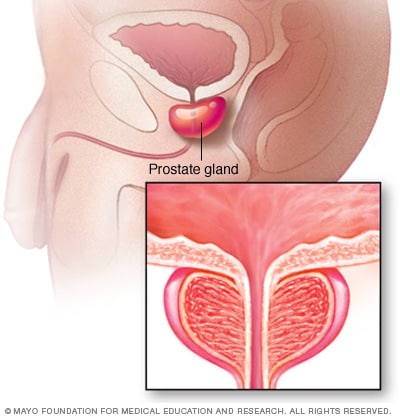
Prostate gland
The prostate gland sits just below the bladder. It surrounds the top part of the tube that drains urine from the bladder, called the urethra. The prostate's main job is to make the fluid that feeds and carries sperm, called seminal fluid. The prostate is part of the male reproductive system.
Transurethral incision of the prostate (TUIP) is a procedure to treat urinary symptoms caused by an enlarged prostate, a condition known as benign prostatic hyperplasia (BPH). TUIP is generally used in younger men with a small prostate who are concerned about fertility.
A combined visual and surgical instrument (resectoscope) is inserted through the tip of the penis into the tube that carries urine from your bladder (urethra). The prostate surrounds the urethra. The doctor cuts one or two small grooves in the area where the prostate and the bladder are connected (bladder neck) to widen the urinary channel and allow urine to pass through more easily.
TUIP is one of several minimally invasive treatment options for BPH. To determine the right BPH treatment choice for you, your doctor will consider how severe your symptoms are, what other health problems you have, and the size and shape of your prostate.
Products & Services
Why it's done
TUIP helps reduce urinary signs and symptoms caused by BPH, including:
- Frequent, urgent need to urinate
- Difficulty starting urination
- Slow (prolonged) urination
- Increased frequency of urination at night
- Stopping and starting again while urinating
- The feeling of not being able to completely empty the bladder
- Urinary tract infections
TUIP might also be done to treat or prevent complications due to blocked urine flow, such as:
- Recurring urinary tract infections
- Kidney or bladder damage
- Inability to control urination or an inability to urinate at all
- Bladder stones
- Blood in the urine
TUIP can offer several advantages over other methods of treating BPH, such as transurethral resection of the prostate (TURP) and open prostatectomy. The advantages can include:
- Lower risk of bleeding. TUIP can be a good option for men who take medication to thin their blood or who have a bleeding disorder that doesn't allow their blood to clot normally.
- Minimal hospital stay. TUIP can be done on an outpatient basis, although some men need to stay overnight for observation. TUIP might be a safer option than surgery if you have certain other health problems.
- Lower risk of dry orgasm. TUIP is less likely than some other BPH treatments to cause the release of semen during ejaculation into the bladder rather than out of the penis (retrograde ejaculation). Retrograde ejaculation isn't harmful, but it can interfere with the ability to father a child.
Risks
TUIP is generally safe with few if any major complications. Possible risks of TUIP can include:
- Temporary difficulty urinating. You might have trouble urinating for a few days after the procedure. Until you can urinate on your own, you may need to have a tube (catheter) inserted into your penis to carry urine out of your bladder.
- Urinary tract infection. This type of infection is a possible complication after any prostate procedure. An infection is increasingly likely to occur the longer you have a catheter in place. Treatment typically includes antibiotics.
- Need for re-treatment. TUIP might be less effective on urinary symptoms than other minimally invasive treatments or surgery. You might need to be treated again with another BPH therapy.
How you prepare
Food and medications
Several days before surgery, your doctor might recommend that you stop taking medications —such as warfarin (Jantoven) or clopidogrel (Plavix) — that can increase your risk of bleeding. You also are likely to be prescribed an antibiotic to prevent a urinary tract infection.
Other precautions
Arrange transportation because you won't be able to drive yourself home after the procedure that day or generally if you have a catheter in your bladder.
Recovery after TUIP is generally quick, and most men have few symptoms after surgery. Ask your doctor how much recovery time you might need.
What you can expect
You'll receive either a general anesthetic, which will put you to sleep, or an anesthetic that blocks feeling from the waist down (spinal block).
During the procedure
Your doctor might put numbing gel inside your urethra and might numb the prostate area with an injection given through your rectum.
Once the anesthetic is working, your doctor will insert a resectoscope into the tip of your penis and extend it to the prostate area. The resectoscope has a lens or camera, a cutting device, and valves to release fluid to wash the surgery area. Using the resectoscope, the doctor makes one or two cuts (incisions) on the inner surface of the prostate.
After the procedure
You might have TUIP on an outpatient basis or you might need to stay overnight in the hospital for observation.
You will likely have a urinary catheter in place because of swelling that blocks urine flow. The catheter is generally removed after 1 to 3 days. You'll also likely take antibiotics to prevent a urinary tract infection.
You might notice:
- Blood in the urine. This typically lasts a few days.
- Irritating urinary symptoms. You might feel an urgent or frequent need to urinate, or you might have to get up more often during the night to urinate. Most men experience burning, especially at the tip of the penis and near the end of urination. These symptoms generally last a few days.
- Difficulty holding urine.The loss of bladder control (incontinence) can occur because your bladder is used to having to push urine through a urethra narrowed by enlarged prostate tissue. For most men, this issue improves with time.
- Urinary tract infection. Urinary tract infections are a possible complication after any enlarged prostate procedure. The risk of infection increases the longer you have a catheter in place.
Results
It might take several weeks for you to experience noticeable improvement in urinary symptoms. If you notice any worsening urinary symptoms over time, see your doctor. Some men need additional BPH treatment.
Aug. 19, 2025