Overview
Prostate brachytherapy (brak-e-THER-uh-pee) is a form of radiation therapy that treats prostate cancer. It involves placing radioactive sources inside the prostate. There, the radiation can kill the cancer cells while causing less harm to healthy tissue nearby. Prostate brachytherapy treats the cancer from inside the prostate.
Prostate brachytherapy is one of several procedures for treating prostate cancer. Other options include external beam radiation therapy and surgery to remove the prostate, known as prostatectomy. Your healthcare team can help you consider your options to see which is right for your circumstances.
Types of prostate brachytherapy
Prostate brachytherapy procedures vary based on the type:
- High dose rate (HDR) brachytherapy delivers a higher dose of radiation over a short time. It involves placing radioactive sources in the prostate gland and giving a high dose of radiation to the targeted area for a few minutes. Then the sources are removed. Treatment may involve a few sessions.
- Low dose rate (LDR) brachytherapy typically uses small radiation seeds, about the size of grains of rice. These are implanted into the prostate gland. The seeds deliver a lower dose of radiation over several months until the radiation is gone. The seeds stay permanently in the body. They are not harmful.
Products & Services
Why it's done
Prostate cancer
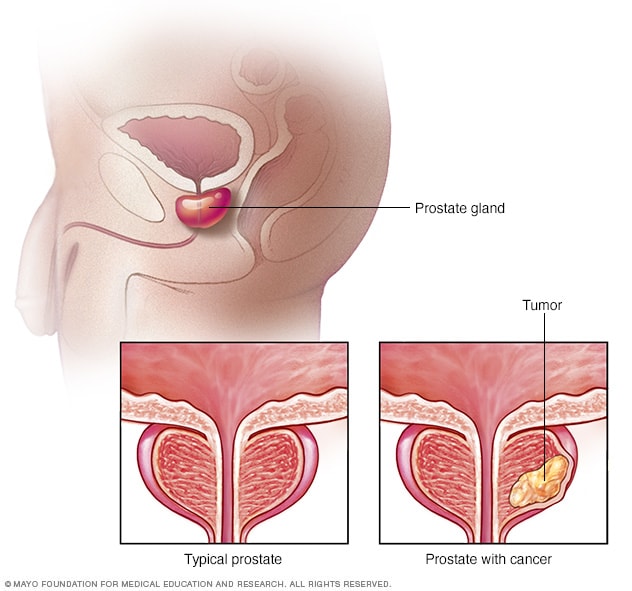
Prostate cancer
Prostate cancer is a growth of cells that starts in the prostate. The prostate is a small gland that helps make semen. It's part of the male reproductive system. This illustration shows a typical prostate gland and a prostate gland with cancer.
Prostate brachytherapy may provide long-term cancer control for prostate cancer. The procedure places radioactive sources inside the prostate. The cancer gets most of the radiation. Nearby healthy tissue gets little radiation. Your healthcare team may recommend brachytherapy for prostate cancer:
- As your main treatment. If you have early-stage prostate cancer that is unlikely to spread beyond the prostate, brachytherapy may be the only treatment you have.
- Along with other treatments. If the cancer is larger or more likely to spread outside the prostate, you may have brachytherapy with other treatments. These might include external beam radiation therapy, hormone therapy or both.
- When prostate cancer returns after radiation to the prostate. If you previously had external beam radiation therapy (EBRT) or brachytherapy for prostate cancer treatment, brachytherapy may be an effective option for cancer that has come back within the prostate.
Healthcare professionals don't often use prostate brachytherapy for metastatic prostate cancer that has spread to the lymph nodes or to other areas of the body.
An advantage of brachytherapy over external beam radiation therapy is potentially shorter treatment time. Brachytherapy usually is completed in one or two visits, often with minimal disruption to your daily routine. A disadvantage of brachytherapy is that it typically requires anesthesia.
Risks
Prostate brachytherapy can lead to side effects, some of which are common while others are rare. If you have existing urinary issues or have had previous pelvic surgeries, your risk of certain side effects may be higher. It's important to discuss these risks with your healthcare team. Depending on your situation, your radiation oncologist might suggest another type of radiation therapy that could offer better results with fewer side effects.
Common side effects
Common side effects of prostate brachytherapy include:
- Discomfort. It is common to have some tenderness or bruising of the perineum. The perineum is the area between the scrotum and the rectal opening. You may see some slight bleeding from this area for the first few days.
- Blood in the urine. You may notice blood in your urine for several days after the procedure. Urinate frequently during the day; do not try to hold your bladder. If you notice increased blood in your urine, reduce your activity. Rest with your feet up. Increase your fluid intake during the next 24 hours.
- Difficult urination. Some people have trouble urinating after the procedure. If you have the urge to urinate and cannot, go to an emergency room. Medicine to help you urinate may be prescribed.
- Urinary irritation. Frequent urination or a strong, sudden urge to urinate may be a sign of an overactive bladder. These symptoms are usually temporary, typically lasting a few weeks to a few months. Medicines may be prescribed to lessen these symptoms. You may feel a burning sensation during urination, but this also can be a sign of a bladder infection. If this becomes a problem for you, contact your healthcare team.
- Discolored semen. Your semen may look brown or black. This comes from bleeding that may take place during the procedure. Semen should return to a usual color within 1 to 2 months. Some people notice a decrease in the amount of semen after brachytherapy. Over time, some people notice a complete absence of semen ejaculation during intercourse and orgasm.
- Bowel problems. Some people have bowel changes after treatment. Your rectal area may feel irritated or painful. You may notice bleeding from the rectum or blood in the stool. You may feel a sudden need to have a bowel movement or need to pass stool more often.
- Sexual side effects. Brachytherapy may affect sexual function. Some people have trouble getting or keeping an erection. This is called erectile dysfunction.
If you have side effects that are getting in the way of your daily life or get worse, talk with your healthcare team. There may be medicines to lessen side effects of treatment. Many side effects of prostate brachytherapy become less noticeable over time.
Brachytherapy may result in fewer issues with urination or sexual function than surgical removal of the prostate.
Rare complications
Some serious complications can happen after prostate brachytherapy, but these are rare. They include:
- Stricture of the urethra. The tube that carries urine from the bladder to the outside of the body may narrow. The tube is called the urethra. The narrowing is called a stricture. Sometimes a procedure can be done to help with urination.
- Rectal ulcer. A sore on the rectum may form. This can lead to prolonged bleeding from the rectum or with bowel movements. Sometimes a procedure can be done to help heal the sore.
How you prepare
To prepare for prostate brachytherapy, you:
- Meet with your radiation oncologist. This is a doctor who specializes in treating cancer with radiation. Your radiation oncologist oversees your brachytherapy treatment.
- Have imaging tests. You have imaging scans done to help plan your treatment. These may include X-rays, MRI scans or CT scans. The images help your radiation oncologist and other members of the care team decide the dose and positioning of the radiation. You have these tests either before your procedure or at the start of your procedure.
- Plan for anesthesia. You and your healthcare team talk about anesthesia for you during the procedure. For prostate brachytherapy, you have general or spinal anesthesia. General anesthesia puts you in a sleeplike state, so you won't feel pain. Spinal anesthesia numbs you from the waist down. For spinal anesthesia, your healthcare team may give you medicine to make you feel drowsy.
- Arrange for someone to drive you home. After you have anesthesia, it is common to have lapses of memory, slowed reaction time and impaired judgment. Do not drive for the rest of the day after the procedure.
- Follow your care team's instructions. Your care team gives you instructions on how to prepare. Instructions include whether you need to stop eating or drinking. They also include whether you need lab tests and, if so, whether you need to change how you take your medicine that day.
What you can expect
What you can expect during prostate brachytherapy depends on the type of brachytherapy treatment you get.
High dose rate (HDR) brachytherapy
High dose radiation therapy for prostate cancer

High dose radiation therapy for prostate cancer
High dose rate (HDR) brachytherapy places a radioactive source inside the prostate for a short time.
HDR brachytherapy for the prostate is temporary. It involves placing a radioactive source in the prostate for several minutes at a time.
Before you get HDR brachytherapy treatments, a wandlike instrument goes into your rectum. This instrument makes ultrasound pictures of your prostate. Guided by these images, your healthcare team inserts thin, hollow needles through the skin between your scrotum and anus, called the perineum, into your prostate. You'll be in a sleeplike state for this part of the procedure so that you aren't aware and won't feel pain.
For HDR brachytherapy treatments, the hollow needles inserted into the prostate connect to a machine. The machine feeds a wire through the needles. This wire holds a radioactive source. The radioactive wire stays in place for a set time in each needle, most often minutes. Then your healthcare team takes out the radioactive wire.
You may have the procedure more than once, depending on your treatment plan.
Because your healthcare team takes the radioactive source out of your body after HDR brachytherapy, you don't need to worry about spreading radiation to other people.
Low dose rate (LDR) brachytherapy
Low dose radiation therapy for prostate cancer

Low dose radiation therapy for prostate cancer
Low dose rate (LDR) brachytherapy implants many tiny radioactive seeds in the prostate for life. The seeds deliver a low dose of radiation over several months until the radiation is gone.
LDR brachytherapy is permanent. It involves placing radioactive seeds in the prostate for life. LDR brachytherapy also is called seed implants.
During this procedure, you have anesthesia to put you in a sleeplike state so that you won't feel pain.
A wandlike instrument goes into your rectum. This instrument makes ultrasound pictures of your prostate. The pictures help to guide long, thin needles that are used to place many seedlike radioactive implants in your prostate.
The needle goes through the skin between your scrotum and your anus, called the perineum, and into your prostate. The seeds, about the size of grains of rice, give off radiation for a few months. They stay in your body for the rest of your life.
After the procedure, you spend some time in a recovery area. Then you can go home. The low levels of radiation in the seeds most often aren't harmful to others. For a short time, as a precaution, you may be asked to avoid being around babies, young children or anyone who is pregnant. You also may be asked to wear a condom during sex for the next few months. This is helpful in the unlikely event that a seed moves out of place and is released through ejaculation.
After the procedure
After prostate brachytherapy, you can expect some pain and swelling of the skin between the scrotum and anus, called the perineum. You may find relief by placing an ice pack over the area and taking pain medicine your healthcare team prescribes.
You can go back to your usual activities when you feel up to it. Your healthcare team may tell you not to do hard exercise or heavy lifting during your recovery.
Results
Brachytherapy is an effective treatment for many people with early-stage prostate cancer. In many cases, it can control the cancer for a long time. For some people with localized prostate cancer, brachytherapy may be an alternative to surgery.
After prostate brachytherapy, you may have follow-up blood tests to measure the level of prostate-specific antigen (PSA) in your blood. Results of these tests can help show whether your treatment has worked.
Your PSA level may rise suddenly after prostate brachytherapy and then go down again. This is called a PSA bounce. Your healthcare team may keep measuring your PSA level to make sure it doesn't keep going up.
Ask your healthcare team when you can expect to know the results of your prostate cancer treatment.
Treatment for a rising PSA after brachytherapy
A PSA level that keeps going up after brachytherapy may mean that the cancer has come back. You may have imaging tests and a prostate biopsy to look for signs of cancer.
There are several treatments for cancer that returns if the cancer is only in the prostate. Treatments include freezing the cancer cells with very cold temperatures, called cryotherapy, and heating the cancer cells with high-intensity focused ultrasound. Treatments also include having additional radiation therapy to the prostate or having surgery to remove the prostate, called salvage prostatectomy.
If your cancer has spread beyond your prostate, you may have other treatments, such as hormone therapy, radiation or chemotherapy.