Overview
Copper IUD (ParaGard)

Copper IUD (ParaGard)
The copper IUD (ParaGard) contains no hormones and prevents pregnancy for up to 10 years.
ParaGard is an intrauterine device (IUD) that can provide long-term birth control (contraception). It's sometimes referred to as a nonhormonal IUD option.
The ParaGard device is a T-shaped plastic frame that's inserted into the uterus. Copper wire coiled around the device produces an inflammatory reaction that is toxic to sperm and eggs (ova), preventing pregnancy.
ParaGard is the only copper IUD available in the United States. It can prevent pregnancy for up to 10 years after insertion.
Why it's done
ParaGard offers effective, long-term contraception. It can be used in premenopausal women of all ages, including teenagers.
Among various benefits, ParaGard:
- Eliminates the need to interrupt sex for contraception
- Can remain in place for up to 10 years
- Can be removed at any time
- Can be used while breast-feeding
- Doesn't carry the risk of side effects, such as blood clots, related to hormonal birth control methods
- Can be used for emergency contraception if inserted within five days after unprotected sex
ParaGard isn't appropriate for everyone. Your health care provider may discourage use of ParaGard if you:
- Have uterine abnormalities — such as large fibroids — that interfere with the placement or retention of ParaGard
- Have a pelvic infection, such as pelvic inflammatory disease
- Have uterine or cervical cancer
- Have unexplained vaginal bleeding
- Are allergic to any component of ParaGard
- Have a disorder that causes too much copper to accumulate in your liver, brain and other vital organs (Wilson's disease)
Risks
Less than 1 percent of women who use ParaGard will get pregnant in the first year of typical use. Over time, risk of pregnancy in women who use ParaGard remains low.
If you do conceive while using ParaGard, you're at high risk of an ectopic pregnancy — when the fertilized egg implants outside the uterus, usually in a fallopian tube. But because ParaGard prevents most pregnancies, the overall risk of having an ectopic pregnancy is lower than it is for sexually active women who don't use contraception.
ParaGard doesn't offer protection from sexually transmitted infections (STIs).
Side effects associated with ParaGard include:
- Bleeding between periods
- Cramps
- Severe menstrual pain and heavy bleeding
It's also possible to expel ParaGard from your uterus. You might not feel the expulsion if it occurs.
You may be more likely to expel ParaGard if you:
- Have never been pregnant
- Have heavy or prolonged periods
- Have severe menstrual pain
- Previously expelled an IUD
- Are younger than age 25
- Had the IUD inserted immediately after childbirth
How you prepare
ParaGard can be inserted anytime during a normal menstrual cycle. If you just had a baby, your doctor might recommend waiting about eight weeks after delivery before inserting ParaGard.
Before inserting ParaGard, your health care provider will evaluate your overall health and do a pelvic exam. You may have a pregnancy test to confirm you're not pregnant, and you may be screened for STIs.
Taking a nonsteroidal anti-inflammatory drug, such as ibuprofen (Advil, Motrin IB, others), one to two hours before the procedure can help reduce cramping.
What you can expect
ParaGard placement
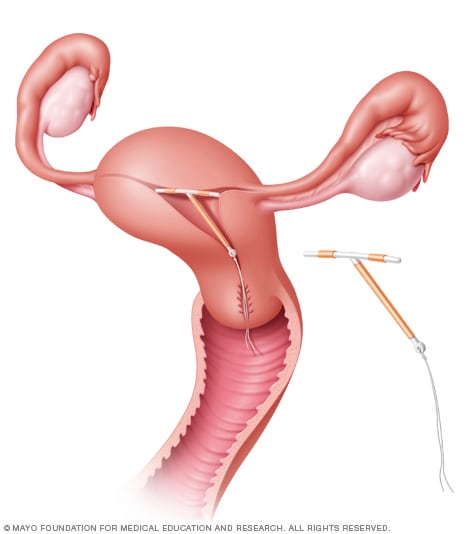
ParaGard placement
The ParaGard IUD can remain in place in your uterus for up to 10 years. Short strings connected to the device extend beyond the cervix into the vagina and allow for device removal.
ParaGard is typically inserted in a health care provider's office.
During the procedure
Your health care provider will insert a speculum into your vagina and clean your vagina and cervix with an antiseptic solution. A special instrument might be used to gently align your cervical canal and uterine cavity. Next, your health care provider will fold down ParaGard's horizontal arms and place the device inside an applicator tube.
The tube is inserted into your cervical canal and ParaGard is carefully placed in your uterus. When the applicator tube is removed, ParaGard will remain in place. Your health care provider will trim ParaGard's strings so that they don't protrude too far into the vagina and may record the length of the strings.
During ParaGard insertion, you may experience dizziness, fainting, nausea, low blood pressure or a slower than normal heart rate. Your health care provider will likely suggest that you stay lying down for a few minutes to allow these side effects to pass. Rarely, it's possible for the IUD to perforate the uterine wall or cervix. If this complication occurs, your health care provider will discuss the appropriate management.
After the procedure
About a month after ParaGard is inserted, your health care provider may re-examine you to make sure the device hasn't moved and to check for signs and symptoms of infection.
While you're using ParaGard, contact your health care provider immediately if you have:
- Signs or symptoms of pregnancy
- Unusually heavy vaginal bleeding
- Foul vaginal discharge
- Worsening pelvic pain
- Severe abdominal pain or tenderness
- Unexplained fever
- Possible exposure to an STI
It's also important to contact your health care provider immediately if you think your ParaGard is no longer in place. Call your doctor if:
- You have breakthrough bleeding or bleeding after sex
- Sex is painful for you or your partner
- The strings are missing or suddenly seem longer
- You feel part of the device at your cervix or in your vagina
Your health care provider will check the location of ParaGard and remove it if necessary.
Removal
ParaGard is usually removed in a health care provider's office. Your provider will likely use forceps to grasp the device's strings and gently pull. The device's arms will fold upward as it's withdrawn from the uterus.
Light bleeding and cramping are common during removal. Rarely, removal can be more complicated.