Overview
Lumbar puncture, also known as a spinal tap
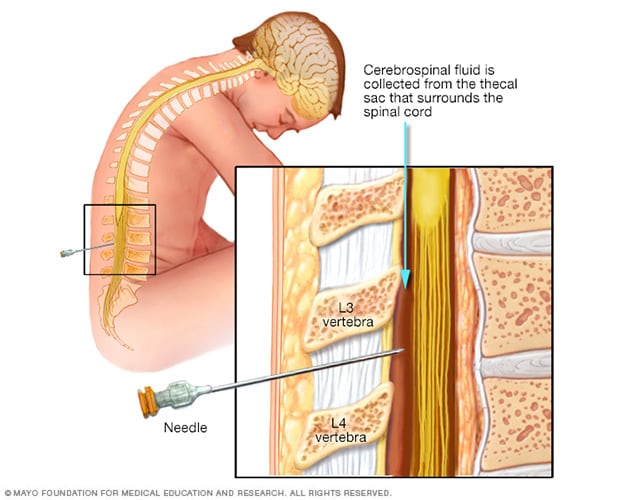
Lumbar puncture, also known as a spinal tap
During a lumbar puncture, also known as a spinal tap, you typically lie on your side with your knees drawn up to your chest. Then a needle is inserted into your spinal canal — in your lower back — to collect cerebrospinal fluid for testing.
A lumbar puncture, also known as a spinal tap, is a test used to diagnose certain health conditions. It's performed in your lower back, in the lumbar region. During a lumbar puncture, a needle is inserted into the space between two lumbar bones, called vertebrae. Then a sample of cerebrospinal fluid is removed. This is the fluid that surrounds the brain and spinal cord to protect them from injury.
A lumbar puncture can help diagnose serious infections, such as meningitis. It also can help diagnose other diseases of the central nervous system, such as Guillain-Barre syndrome and multiple sclerosis. A lumbar puncture may be used to diagnose bleeding around the brain or cancers of the brain or spinal cord. Sometimes a lumbar puncture is used to inject anesthetic medicines or chemotherapy into the cerebrospinal fluid.
Why it's done
A lumbar puncture, also known as a spinal tap, may be done to:
- Collect cerebrospinal fluid to check for infections, inflammation or other diseases.
- Measure the pressure of cerebrospinal fluid.
- Inject spinal anesthetics, chemotherapy or other medicines.
- Inject dye, known as myelography, or radioactive substances, known as cisternography, into cerebrospinal fluid to make diagnostic images of the fluid's flow.
Information gathered from a lumbar puncture can help diagnose:
- Serious bacterial, fungal and viral infections, including meningitis, encephalitis and syphilis.
- Bleeding around the brain, known as subarachnoid hemorrhage.
- Certain cancers involving the brain or spinal cord.
- Certain inflammatory conditions of the nervous system, such as multiple sclerosis and Guillain-Barre syndrome.
- Autoimmune neurological conditions.
- Alzheimer's disease and other forms of dementia.
More Information
Risks
Although a lumbar puncture, also known as a spinal tap, is generally safe, it does carry some risks. These include:
Post-lumbar puncture headache. As many as 25% of people who undergo a lumbar puncture develop a headache afterward due to fluid leaking into nearby tissues.
The headache typically starts several hours and up to two days after the procedure. The headache may occur with nausea, vomiting and dizziness. The headaches are usually present when sitting or standing and resolve after lying down. Post-lumbar puncture headaches can last from a few hours to a week or more.
- Back discomfort or pain. You may feel pain or tenderness in your lower back after the procedure. The pain might radiate down the back of your legs.
- Bleeding. Bleeding may occur near the puncture site or, rarely, in the epidural space.
-
Brainstem herniation. A brain tumor or other space-occupying lesion can increase pressure within the skull. This can lead to compression of the brainstem, which links the brain to the spinal cord, after a sample of cerebrospinal fluid is removed.
To prevent this rare complication, a computerized tomography (CT) scan or magnetic resonance imaging (MRI) scan is often performed before a lumbar puncture. The scans are used to look for any sign of a space-occupying lesion resulting in increased intracranial pressure. A detailed neurological examination also can help rule out a space-occupying lesion.
How you prepare
Before your lumbar puncture, also called a spinal tap, your healthcare professional takes your medical history, does a physical exam, and orders blood tests to check for bleeding or clotting conditions. Your healthcare professional also may recommend a CT scan or MRI to look for swelling in or around your brain.
Food and medications
Your healthcare professional gives you specific instructions about food, drink and medicines.
Tell your healthcare professional if you're taking blood-thinning or other anticoagulant medicines. Examples include warfarin (Jantoven), clopidogrel (Plavix) and apixaban (Eliquis). Also, tell your healthcare professional if you are allergic to any medicines, such as numbing medicines, known as local anesthetics.
What you can expect
A lumbar puncture, also known as a spinal tap, is usually done in an outpatient facility or a hospital. Your healthcare professional talks to you about the potential risks, and any discomfort you might feel during the procedure.
If a child is having a lumbar puncture, a parent may be allowed to stay in the room. Talk to your child's healthcare professional about whether this is possible.
Before the procedure
You may be asked to change into a hospital gown or you may have the procedure while wearing your own clothing. There are a few possible positions for a lumbar puncture. Usually, you lie on your side with your knees drawn up to your chest, or you sit and lean forward on a stable surface. These positions flex your back, widening the spaces between your vertebrae and making it easier for your healthcare professional to insert the needle. Your back is washed with antiseptic soap or iodine and covered with a sterile sheet.
For an infant or a young child, someone will hold the child in position during the procedure.
During the procedure
- A local anesthetic is injected into your lower back to numb the puncture site before the needle is inserted. The local anesthetic stings briefly as it's injected.
- A thin, hollow needle is inserted between the two lower vertebrae, known as the lumbar region. The needle goes through the spinal membrane called the dura and into the spinal canal. You may feel pressure in your back during this part of the procedure.
- Once the needle is in place, you may be asked to change your position slightly.
- The cerebrospinal fluid pressure is measured, a small amount of fluid is withdrawn and the pressure is measured again.
- The needle is removed, and the puncture site is covered with a bandage.
The procedure usually lasts about 45 minutes. Your healthcare professional may suggest lying down after the procedure.
Sometimes, an ultrasound may be used as a guide during a lumbar puncture on infants and young children. The ultrasound can help prevent inserting the needle too far.
After the procedure
- Plan to rest. Don't participate in strenuous activities the day of your lumbar puncture. You may return to work if your job doesn't require you to be physically active. Discuss your activities with your healthcare professional if you have questions.
- Take a pain medicine. A nonprescription pain-relieving medicine that contains acetaminophen (Tylenol, others) can help reduce a headache or back pain. If your headache becomes severe, call your healthcare professional.
Results
The spinal fluid samples from the lumbar puncture, also known as a spinal tap, are sent to a laboratory for analysis. Lab technicians check for a number of things when examining spinal fluid, including:
- General appearance. Spinal fluid is normally clear and colorless. If the color is orange, yellow or pink, it might suggest bleeding. Spinal fluid that is green might suggest an infection or the presence of bilirubin.
- Protein, including total protein and the presence of certain proteins. High levels of total protein — greater than 45 milligrams per deciliter (mg/dL) — may suggest an infection or another inflammatory condition. Specific lab values may vary depending on the medical facility.
- White blood cells. Spinal fluid usually contains up to five white blood cells per microliter. Increased numbers may suggest an infection or other condition. Specific lab values may vary depending on the medical facility.
- Sugar, also called glucose. A low glucose level in spinal fluid may indicate an infection, tumor or another condition.
- Microorganisms. The presence of bacteria, viruses, fungi or other microorganisms can indicate an infection.
- Cancer cells. The presence of certain cells in spinal fluid — such as tumor or immature blood cells — can suggest some types of cancer.
Lab results are combined with information obtained during the test, such as spinal fluid pressure, to help make a possible diagnosis.
Your healthcare professional typically gives you the results within a few days, but it could take longer. Ask when you can expect to receive the results of your test.
Write down questions that you want to ask your healthcare professional. Don't hesitate to ask other questions that may come up during your visit. Questions you may want to ask include:
- Based on the results, what are my next steps?
- What kind of follow-up, if any, should I expect?
- Are there any factors that might have affected the results of this test and, therefore, may have altered the results?
- Will I need to repeat the test at some point?
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.