Overview
Prostate cancer
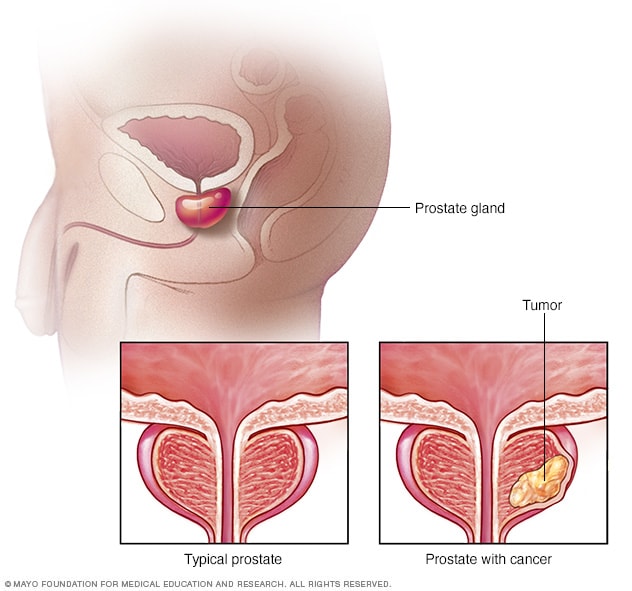
Prostate cancer
Prostate cancer occurs in the prostate gland. The gland sits just below the bladder in males. It surrounds the top part of the tube that drains urine from the bladder, called the urethra. This illustration shows a healthy prostate gland and a prostate gland with cancer.
Hormone therapy for prostate cancer is a treatment that stops the hormone testosterone either from being made or from reaching prostate cancer cells.
Most prostate cancer cells rely on testosterone to grow. Hormone therapy causes prostate cancer cells to die or to grow more slowly.
Hormone therapy for prostate cancer may involve medicines or possibly surgery to remove the testicles.
Hormone therapy for prostate cancer also is known as androgen deprivation therapy.
Products & Services
Why it's done
Hormone therapy for prostate cancer is used to block the hormone testosterone in the body. Testosterone fuels the growth of prostate cancer cells.
Hormone therapy might be a choice for prostate cancer at different times and for different reasons during cancer treatment.
Hormone therapy can be used:
- For prostate cancer that has spread, called metastatic prostate cancer, to shrink the cancer and slow the growth of tumors. The treatment also might relieve symptoms.
- After prostate cancer treatment if the prostate-specific antigen (PSA) level remains high or starts rising.
- In locally advanced prostate cancer, to make external beam radiation therapy better at lowering the risk of the cancer coming back.
- To lower the risk that the cancer will come back in those who have a high risk of cancer recurrence.
Risks
Side effects of hormone therapy for prostate cancer can include:
- Loss of muscle mass.
- Increased body fat.
- Loss of sex drive.
- Not being able to get or keep an erection, called erectile dysfunction.
- Bone thinning, which can lead to broken bones.
- Hot flashes.
- Less body hair, smaller genitals and growth of breast tissue.
- Tiredness.
- Diabetes.
- Heart disease.
Intermittent dosing
In certain situations, doctors may recommend taking hormone therapy medicines for a set amount of time or until the PSA level is very low. Then the medicine is stopped. For some people, this approach can help reduce the side effects of hormone therapy. If the prostate cancer comes back or gets worse, it might be necessary to start the medicines again.
Early research shows that starting and stopping hormone therapy medicines, sometimes called intermittent dosing, may lower the risk of side effects without affecting long-term survival. And this dosing approach might improve quality of life.
How you prepare
If you're thinking of having hormone therapy for prostate cancer, discuss your choices with your doctor. Types of hormone therapy for prostate cancer include:
- Medicines that stop the testicles from making testosterone. Certain medicines stop cells from getting the signals that tell them to make testosterone. These medicines are called luteinizing hormone-releasing hormone (LHRH) agonists and antagonists. Another name for these medicines is gonadotropin-releasing hormone agonists and antagonists.
- Medicines that stop testosterone from acting on cancer cells. These medicines, known as anti-androgens, are often used with LHRH agonists. That's because LHRH agonists can cause a brief rise in testosterone levels before testosterone levels go down.
- Surgery to remove the testicles, called an orchiectomy. Surgery to remove both testicles lowers testosterone levels in the body quickly. A version of this procedure removes only the tissue that makes testosterone, not the testicles. Surgery to remove the testicles can't be reversed.
What you can expect
LHRH agonists and antagonists
LHRH agonist and antagonist medicines stop the testicles from making testosterone.
Most of these medicines are given as a shot under the skin or into a muscle. They're given monthly, every three months or every six months. Or they can be put under the skin as an implant. The implant slowly releases medicines over time.
LHRH agonists include:
- Leuprolide (Eligard, Lupron Depot, others).
- Goserelin (Zoladex).
- Triptorelin (Trelstar).
LHRH antagonists include:
- Degarelix (Firmagon).
- Relugolix (Orgovyx).
Testosterone levels might rise briefly, called a flare, for a few weeks after an LHRH agonist. LHRH antagonists don't cause a testosterone flare.
Cutting the risk of a flare is important for those who have pain or other cancer symptoms. An increase in testosterone can make symptoms worse. Taking an anti-androgen either before or with an LHRH agonist can cut the risk of flare.
Anti-androgens
Anti-androgens keep testosterone from acting on cancer cells. These oral medicines often are taken with an LHRH agonist or before taking an LHRH agonist.
Anti-androgens include:
- Bicalutamide (Casodex).
- Flutamide.
- Nilutamide (Nilandron).
- Apalutamide (Erleada).
- Darolutamide (Nubeqa).
- Enzalutamide (Xtandi).
Other androgen-blocking medicines
When hormone therapy treatment stops the testicles from making testosterone, other cells in the body might make testosterone that can cause prostate cancer cells to grow. Other hormone therapy medicines can stop these other sources of testosterone. The medicines might be used when prostate cancer remains or comes back. These medicines are sometimes mixed with corticosteroids, such as prednisone. These medicines include:
- Abiraterone (Yonsa, Zytiga).
- Ketoconazole.
These medicines treat advanced prostate cancer that no longer responds to other hormone therapy treatments.
Orchiectomy
This treatment to remove the testicles is rarely used. After numbing the groin area, a surgeon cuts into the groin and takes the testicle through the opening. The surgeon repeats the process for the other testicle.
All surgery carries a risk of pain, bleeding and infection. Most people can go home after this operation. It usually doesn't require staying the hospital.
Results
If you take hormone therapy for prostate cancer, you'll have regular follow-up meetings with your doctor. Your doctor may ask about any side effects you're experiencing. Many side effects can be controlled.
Your doctor might order tests to check your health and watch for signs that the cancer is coming back or getting worse. Results of these tests can show your response to hormone therapy. The treatment might be adjusted, if needed.