Overview
Types of hysterectomy surgery
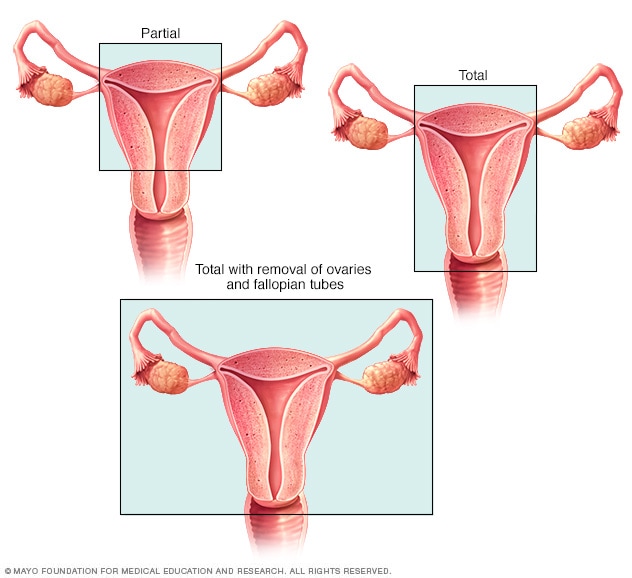
Types of hysterectomy surgery
A partial hysterectomy, shown top left, removes the uterus. A total hysterectomy, shown top right, removes the uterus and cervix. The surgeon also may remove the ovaries and fallopian tubes, shown on the bottom.
An abdominal hysterectomy is an operation that removes the uterus through a cut in the lower belly, also called the abdomen. This is known as an open procedure. The uterus, also called the womb, is where a baby grows when someone is pregnant. A partial hysterectomy removes the uterus, leaving the neck of the womb in place. The neck of the womb is the cervix. A total hysterectomy removes the uterus and the cervix.
A hysterectomy also can be done through a cut in the vagina. This is called a vaginal hysterectomy. Or you may have laparoscopic or robotic surgery, which uses long, thin instruments passed through small cuts in the belly.
You may need an abdominal hysterectomy instead of other types of hysterectomy if:
- You have a large uterus.
- Your health care provider wants to check other pelvic organs for signs of disease.
- Your surgeon feels it's in your best interest to do the surgery as an open procedure.
Products & Services
Why it's done
Female reproductive system
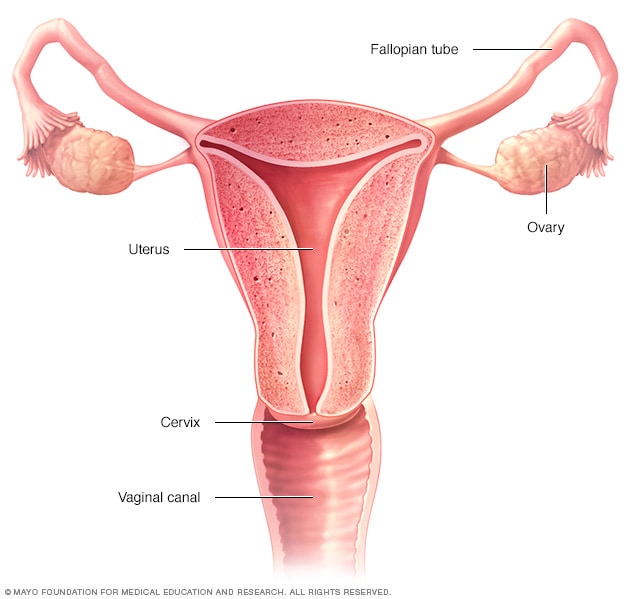
Female reproductive system
The ovaries, fallopian tubes, uterus, cervix and vagina, also called the vaginal canal, make up the female reproductive system.
You may need a hysterectomy to treat:
- Cancer. If you have cancer of the uterus or cervix, a hysterectomy may be the best treatment option. Depending on the specific cancer and how advanced it is, other treatment options might include radiation or chemotherapy.
- Fibroids. A hysterectomy is the only certain, lasting fix for fibroids. Fibroids are tumors that grow in the uterus. They are not cancer. They can cause heavy bleeding, anemia, pelvic pain and bladder pressure.
- Endometriosis. Endometriosis is a condition where tissue that's similar to tissue lining the inside of the uterus grows outside the uterus. The tissue may grow on the ovaries, fallopian tubes and other nearby organs. For severe endometriosis, a hysterectomy may be needed to remove the uterus along with the ovaries and fallopian tubes.
- Uterine prolapse. When pelvic floor muscles and ligaments stretch and weaken, there may not be enough support to keep the uterus in place. When the uterus moves out of place and slips into the vagina, it's called uterine prolapse. This condition can lead to urine leakage, pelvic pressure and problems with bowel movements. A hysterectomy is sometimes needed to treat this condition.
- Irregular, heavy vaginal bleeding. If your periods are heavy, don't come at regular intervals or last many days each cycle, a hysterectomy may bring relief. A hysterectomy is done only when the bleeding can't be managed by other methods.
- Chronic pelvic pain. Surgery may be needed as a last resort if you have chronic pelvic pain that starts in the uterus. But a hysterectomy doesn't fix some forms of pelvic pain. Having a hysterectomy that you don't need may create new problems.
- Gender-confirmation surgery. Some people who wish to better align their bodies with their gender identities choose to have hysterectomies to remove the uterus and cervix. This type of surgery also might include removing the ovaries and fallopian tubes.
After hysterectomy, you can no longer get pregnant. If there's a chance you might want to become pregnant in the future, ask your health care provider about other treatment options. In the case of cancer, a hysterectomy might be your only option. But for conditions such as fibroids, endometriosis and uterine prolapse, there may be other treatments.
During hysterectomy surgery, you might have a related procedure to remove the ovaries and the fallopian tubes. If you're still having periods, removal of both ovaries leads to what's known as surgical menopause.
With surgical menopause, menopause symptoms often begin quickly after having the procedure. Short-term use of hormone therapy can help ease symptoms that really bother you.
Risks
A hysterectomy is generally safe, but with any major surgery comes the risk of complications.
Risks of an abdominal hysterectomy include:
- Infection.
- Too much bleeding during surgery.
- Damage to the urinary tract, bladder, rectum or other pelvic structures during surgery, which may need more surgery to fix them.
- A bad reaction to anesthesia, which is the medicine used during surgery to numb pain.
- Blood clots.
- Menopause that starts at a younger age, even if the ovaries aren't taken out.
- Rarely, death.
How you prepare
You may feel anxious about having a hysterectomy. Being prepared before surgery may help calm your nerves. To get ready for your procedure:
- Gather information. Before surgery, get all the information you need to feel confident about your choice to have a hysterectomy. Ask questions of your health care team. Learn about the surgery, including all the steps involved and what you can expect after surgery.
- Follow instructions about medicines. Find out whether you need to change the usual medicines you take in the days leading up to surgery. Tell your care team about any over-the-counter medicines, dietary supplements or herbs that you take.
- Ask what type of anesthesia you'll have. An abdominal hysterectomy usually requires general anesthesia. This type of anesthesia puts you in a sleep-like state during surgery.
- Plan for a hospital stay. How long you stay in the hospital depends on the type of hysterectomy you have. For an abdominal hysterectomy, plan for a hospital stay of at least 1 to 2 days.
- Arrange for help. Full recovery could take several weeks. You may need to limit your activities during this time. For example, you may need to avoid driving or lifting anything heavy. Arrange for help at home if you think you'll need it.
- Get as fit as possible. Stop smoking if you are a smoker. Focus on eating healthy foods, getting exercise and losing weight, if needed.
What you can expect
Before the procedure
You may need tests to check for cancer and other diseases. Test results could change the surgeon's approach to the operation. Tests may include:
- A Pap test, also called cervical cytology, which finds irregular cervical cells or cervical cancer.
- Endometrial biopsy, which takes a sample of tissue from the lining of the uterus. This test may find irregular cells in the uterine lining or endometrial cancer.
- Pelvic ultrasound, which is an imaging test that can show the size of uterine fibroids, endometrial polyps or ovarian cysts.
- Blood tests, to check for any conditions that might affect surgery.
- Pelvic MRI, which is a scan that uses a magnetic field to create images of organs and tissues inside the body.
- CT of the abdomen and pelvis, which uses X-rays taken from different angles around your body to show cross-sectional images of the uterus and other pelvic structures.
The day before and the morning of the surgery, you'll bathe or shower using a special soap. This can help reduce the risk of infection. Your care team also may have you clean the vagina with a vaginal douche and the rectum with an enema.
During the procedure
Abdominal hysterectomy incisions
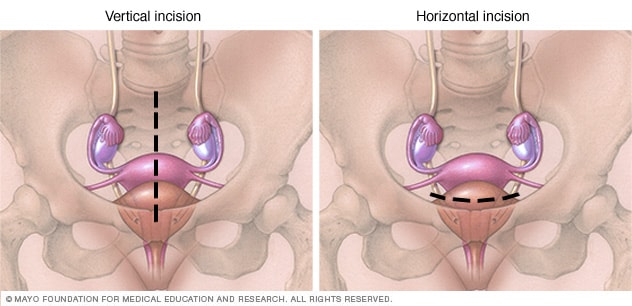
Abdominal hysterectomy incisions
During abdominal hysterectomy, your surgeon makes a vertical or a horizontal cut, called an incision, in the lower abdomen. A vertical cut, shown left, gives the surgeon more access to the pelvis. A horizontal cut, shown right, follows the skin's natural lines, usually leaving a thinner scar.
You'll receive general anesthesia before the procedure. This means you will not feel pain during the surgery. The procedure itself generally lasts about 1 to 2 hours.
You'll have a urinary tube, called a catheter, passed through the urethra to empty the bladder. The catheter remains in place during surgery and for a short time afterward. Your care team uses a sterile solution to clean the abdomen and vagina before surgery. You also will receive antibiotic medicine through a vein in your arm to lower your risk of infection.
Next, the surgeon makes a cut in the lower abdomen. This cut is called an incision. You may have:
- A vertical incision, which starts in the middle of the abdomen and extends from below the bellybutton to above the pubic bone. Sometimes this incision also needs to be extended above the bellybutton. That's determined by the size of the uterus or if other surgical procedures also are planned along with the hysterectomy.
- A horizontal bikini-line incision, which lies about an inch above the pubic bone.
What type of incision you'll need depends on many factors. These include the reason for the hysterectomy, the need to explore the upper abdomen, the size of the uterus and whether you have any scars from prior surgeries.
After the procedure
After surgery, you're moved into the recovery room and then to your hospital room. Your care team will:
- Check for symptoms of pain.
- Give you medicine to control your pain.
- Encourage you to get up and move around soon after surgery.
- Encourage you to drink fluids and eat small meals.
- Watch for surgical complications.
You may be in the hospital for 1 to 2 days, but it could be longer. Sanitary pads can help control vaginal bleeding and discharge. You may have bloody vaginal drainage for several days to weeks after a hysterectomy. Let your care team know if you have bleeding that is as heavy as a period or bleeding that won't stop.
Over time, your incision will heal. But you will have a visible scar on your lower abdomen.
Results
It may take several weeks before you feel like you're back to your usual self. During that time:
- Get plenty of rest.
- Don't lift anything heavy for a full six weeks after the operation.
- Stay active after the surgery, but avoid strenuous physical activity for the first six weeks.
- Wait six weeks to resume sexual activity.
- Follow your care team's suggestions about returning to your usual activities.
Life after a hysterectomy
A hysterectomy changes some aspects of life. For instance:
- You'll no longer have periods.
- You may feel relief from the symptoms that made the surgery necessary.
- You won't be able to become pregnant.
- If you're premenopausal, having the ovaries removed along with the uterus starts menopause.
- You may begin menopause at a younger age after a hysterectomy, even if the ovaries weren't taken out during surgery.
- With a partial hysterectomy, the cervix remains in place. There's still a risk of cervical cancer. Regular Pap tests will often still be needed to screen for cervical cancer.
Other parts of your life likely will return to how they were before surgery or get better. For example:
- If you had a good sex life before a hysterectomy, chances are you'll continue to have a good sex life after surgery. You may even have more sexual pleasure after a hysterectomy. This may be due to relief from chronic pain or heavy bleeding that came from a uterine problem.
- Relief of symptoms may improve your quality of life. You may feel an overall sense of well-being.
But you may have a sense of loss after a hysterectomy. Premenopausal women who need to have a hysterectomy to treat gynecologic cancer may grieve the loss of fertility. If sadness or negative feelings interfere with your enjoyment of everyday life, talk with a health care provider.
Feb. 28, 2023