Having healthy sperm is an important part of fertility. But a variety of factors can affect sperm health. Learn about steps to take, as well as things to avoid, to keep sperm healthy and improve fertility.
What are the key parts of sperm health?
Sperm health depends mainly on sperm quantity, movement and shape:
- Quantity. Ideally, the semen in a single ejaculation, called an ejaculate, has at least 15 million sperm per milliliter. Less than that lowers the chances of getting pregnant because there are fewer sperm available to fertilize an egg.
- Movement. To reach and fertilize an egg, sperm must be able to move easily through the cervix, uterus and fallopian tubes. This is called motility. In general, at least 40% of sperm need to be able to move to achieve pregnancy. Although it's possible for pregnancy to happen with lower levels of sperm movement, it's much less common.
- Shape (morphology). Typical sperm have oval heads and long tails, which work together to help sperm move. In general, sperm shape isn't as important to fertility as quantity or movement. But the more sperm there are that have a typical shape, the more likely it is for pregnancy to happen.
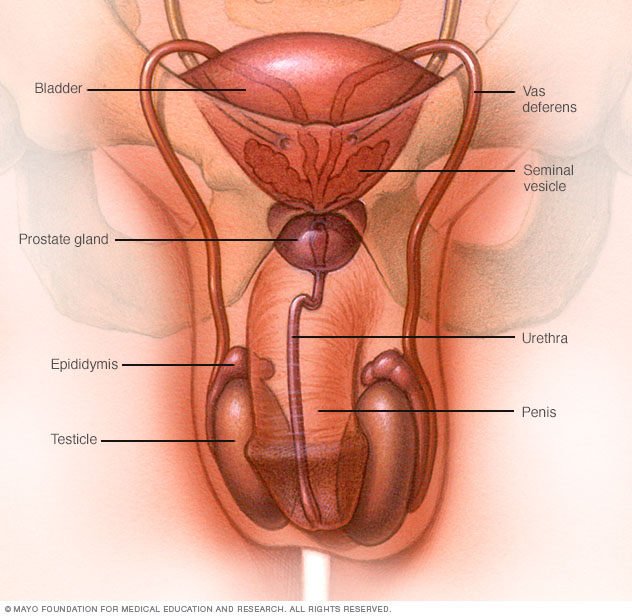
Male reproductive system
The male reproductive system makes, stores and moves sperm. Testicles produce sperm. Fluid from the seminal vesicles and prostate gland combine with sperm to make semen. The penis ejaculates semen during sexual intercourse.
What causes male fertility problems?
Some health issues can have an impact on male fertility, including:
- Diseases and conditions that affect the testicles.
- Conditions that affect how sperm move.
- Medical conditions that affect the hypothalamus or the pituitary gland. These glands send out hormones that cause the testicles to make testosterone and sperm. Some conditions can lower the amount of hormones the glands make. That then lowers the amount of testosterone and sperm in the body.
Age also can play a role. Sperm's ability to move and the number of sperm that have a typical shape tend to go down with age. This is especially true after age 50.
What's the best way to make healthy sperm?
Simple steps to raise the chances of having healthy sperm include:
- Stay at a healthy weight. Some research suggests that increasing body mass index (BMI) is linked with decreasing sperm count and sperm movement.
- Prevent sexually transmitted infections. Sexually transmitted infections, also called STIs, such as chlamydia and gonorrhea can cause male infertility. To lower the risk of getting an STI, don't have a lot of sexual partners and always use a condom for sex. Or stay in a relationship with only one person who doesn't have an STI.
- Manage stress. Stress may lower a person's ability to have sex. Stress also could have an impact on hormones that the body needs to make healthy sperm.
What can harm sperm?
Some things may damage sperm, such as alcohol, certain medicines and toxic chemicals. To protect fertility:
- Don't smoke. People who smoke cigarettes are more likely to have low sperm counts. If you smoke, ask your healthcare professional to help you quit.
- Limit alcohol. Heavy drinking can lead to lower sperm counts. And it can cause a drop in the hormone testosterone. Drinking a lot also can make it difficult to get and keep an erection. If you choose to drink, do so in moderation. For healthy adults, that means up to one drink a day for women and two drinks a day for men.
- Don't use lubricants. Some lubricants might interfere with sperm movement. When you're trying to start a pregnancy, it's best not to use a lubricant for sex. Or, if you need lubricant, consider options such as vegetable oil, mineral oil, canola oil or mustard oil. You also could try a lubricant designed for people trying to get pregnant (BabyDance, Conceive Plus, Pre-Seed, others).
- Understand the effect of medicines. Certain medicines may lessen fertility. Examples include some medicines used to control blood pressure, some antidepressants, antiandrogens, opioids and anabolic steroids. Many kinds of illegal drugs also have an impact on fertility. If you're trying to start a pregnancy and you take medicines, ask your healthcare professional if any of them could affect your fertility.
- Watch out for toxins. Being around pesticides, lead and other toxins can affect sperm quantity and quality. If you must work with toxins, do so safely. Wear protective clothing, use protective equipment, such as safety goggles, and avoid skin contact with chemicals.
- Stay cool. Some research suggests that if the scrotum gets too warm, it could lower the body's ability to make sperm effectively. Wearing loose-fitting underwear, sitting less, and not using saunas and hot tubs may improve sperm quality.
Chemotherapy and radiation therapy for cancer can disrupt the body's ability to make sperm and could cause lasting infertility. If you need cancer treatment, you may want to talk with your healthcare professional about storing sperm before treatment.
When is it time to get help?
Following a healthy lifestyle that fosters sperm health and fertility can improve the chances of achieving pregnancy. But if a pregnancy hasn't happened after a year of having sex without birth control, you may want to be checked for infertility. A fertility specialist may be able to identify the cause of the problem and provide helpful treatment.
ART-20047584
