Diagnosis
Liver biopsy
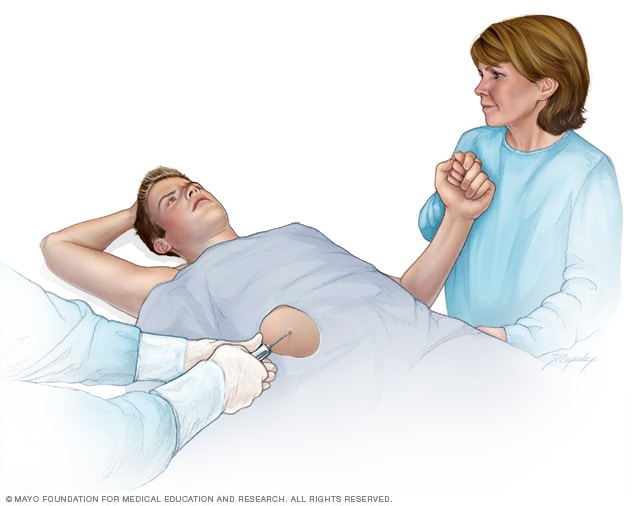
Liver biopsy
A liver biopsy is a procedure to remove a small sample of liver tissue for laboratory testing. A liver biopsy is commonly performed by inserting a thin needle through your skin and into your liver.
Diagnosing Wilson's disease can be hard because its symptoms often are like other liver diseases, such as hepatitis. Also, symptoms can occur over time. Changes in behavior that come on gradually can be especially hard to link to Wilson's disease.
Doctors rely on symptoms and test results to make the diagnosis. Tests and procedures used to diagnose Wilson's disease include:
- Blood and urine tests. Blood tests can monitor your liver function and check the level of a protein called ceruloplasmin that binds copper in the blood. They can check the level of copper in your blood too. Your doctor also might want to measure the amount of copper removed in your urine during a 24-hour period.
- Eye exam. Using a microscope with a high-intensity light, an eye doctor checks your eyes for Kayser-Fleischer rings. This is called a slit-lamp exam. These rings are caused by extra copper in the eyes. Wilson's disease also is related to a type of cataract, called a sunflower cataract. This cataract can be seen during an eye exam.
- Removing a sample of liver tissue for testing, also known as a biopsy. In a biopsy, your doctor inserts a thin needle through your skin and into your liver. Then your doctor draws a small sample of tissue. A laboratory tests the tissue for extra copper.
- Genetic testing. A blood test can pinpoint the genetic changes that cause Wilson's disease. If you have the changed gene that causes Wilson's disease, doctors also can screen any siblings. If any have the changed gene, that sibling can start treatment before symptoms begin.
More Information
Treatment
Your doctor might recommend medicines called copper chelating agents. These medicines attach themselves to copper and cause your organs to release that copper into your bloodstream. Your kidneys then filter the copper and release it into your urine.
Treatment then focuses on stopping copper from building up again. For severe liver damage, a liver transplant might be needed.
Medicines
If you take medicines for Wilson's disease, treatment is lifelong. Medicines include:
- Penicillamine (Cuprimine, Depen). Penicillamine is a copper chelating agent. It can cause serious side effects, including skin and kidney issues, and worsen nervous system symptoms. It also can cause bone marrow suppression, so bone marrow can't make enough red blood cells and platelets. Use penicillamine cautiously if you have a penicillin allergy. It also keeps vitamin B6 (pyridoxine) from working. That means you'll need to take a B6 supplement in small doses.
- Trientine (Cuvrior, Syprine). Another copper chelation agent called trientine works much like penicillamine, but it tends to cause fewer side effects. Still, nervous system symptoms can get worse when taking trientine.
- Zinc acetate (Galzin). This medicine stops your body from absorbing copper from the food you eat. It's usually used to stop copper from building up again after treatment with penicillamine or trientine. Zinc acetate might be used as the main therapy if you can't take penicillamine or trientine after completing therapy to remove excess copper or if you have no symptoms. Zinc acetate can upset your stomach.
Your doctor also might recommend ways to treat other symptoms of Wilson's disease.
Surgery
Living liver transplant
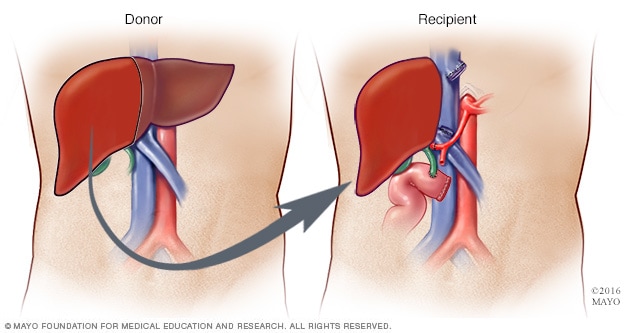
Living liver transplant
During living liver donation, surgeons remove about 40% to 70% of the donor liver and place it into the recipient.
If your liver damage is serious, you might need a liver transplant. During a liver transplant, a surgeon removes your diseased liver and replaces it with a healthy liver from a donor.
Most transplanted livers come from donors who have died. Sometimes a liver can come from a living donor, such as a family member. In that case, the surgeon removes your diseased liver and replaces it with a portion of the donor's liver.
Lifestyle and home remedies
If you have Wilson's disease, your doctor likely will recommend that you limit the amount of copper in your diet. Also, if you have copper pipes in your home, you might want to test the copper levels in your tap water. Be sure to stay away from multivitamins that contain copper.
Foods that contain high amounts of copper include:
- Liver.
- Shellfish.
- Mushrooms.
- Nuts.
- Chocolate.
Ask your healthcare team for more information on foods that have high amounts of copper.
Preparing for your appointment
You'll likely first see your family doctor. Then you might be referred to a doctor who specializes in the liver, also known as a hepatologist.
What you can do
When you make the appointment, ask if there's anything you need to do ahead of time, such as change your diet for blood tests.
Make a list of:
- Your symptoms and when they began.
- Key personal information, including major stresses, other medical conditions you have and any family history of Wilson's disease.
- All medicines, vitamins or other supplements you take, including doses.
- Questions to ask your doctor.
If possible, take a family member or friend along to help you remember the information you're given.
For Wilson's disease, questions to ask your doctor include:
- What tests do I need?
- What treatment do you recommend?
- What are the side effects of the recommended treatment?
- Are there other treatment options?
- I have these other health conditions. How can I best manage them together?
- Do I need to limit the types of food I eat?
- Should I see a specialist?
- Should my family be tested for Wilson's disease?
- Are there brochures or other printed material that I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your doctor is likely to ask you several questions, such as:
- Do your symptoms occur all the time or only once in a while?
- How serious are your symptoms?
- How long have you had these symptoms?
- What, if anything, seems to make your symptoms better or worse?
- Does anyone else in your family have Wilson's disease?
Dec. 02, 2023