Diagnosis
There are several blood tests for type 1 diabetes in children. These tests are used to diagnose diabetes and to monitor diabetes management:
- Random blood sugar test. This is the primary screening test for type 1 diabetes. A blood sample is taken at a random time. A blood sugar level of 200 milligrams per deciliter (mg/dL), or 11.1 millimoles per liter (mmol/L), or higher, along with symptoms, suggests diabetes.
- Glycated hemoglobin (A1C) test. This test indicates your child's average blood sugar level for the past 3 months. An A1C level of 6.5% or higher on two separate tests indicates diabetes.
- Fasting blood sugar test. A blood sample is taken after your child hasn't eaten (fasted) for at least 8 hours or overnight. A fasting blood sugar level of 126 mg/dL (7.0 mmol/L) or higher suggests type 1 diabetes.
Additional tests
If blood sugar testing indicates diabetes, your health care provider may recommend additional tests to distinguish between type 1 diabetes and type 2 diabetes because treatment strategies differ by type. Additional tests include blood tests to check for antibodies that are common in type 1 diabetes.
Treatment
Treatment for type 1 diabetes includes:
- Taking insulin
- Monitoring blood sugar
- Eating healthy foods
- Exercising regularly
You'll work closely with your child's diabetes treatment team — health care provider, certified diabetes care and education specialist, and registered dietitian. The goal of treatment is to keep your child's blood sugar within certain numbers. This target range helps to keep your child's blood sugar level as close to normal as possible.
Your child's health care provider will let you know what your child's blood sugar target range is. This range may change as your child grows and changes.
Insulin
Anyone who has type 1 diabetes needs lifelong treatment with one or more types of insulin to survive.
Many types of insulin are available, including:
- Rapid-acting insulin. This type of insulin starts working within 15 minutes. It reaches peak effect at 60 minutes and lasts about 4 hours. This type is often used 15 to 20 minutes before meals. Examples are lispro (Humalog, Admelog), aspart (NovoLog, Fiasp) and glulisine (Apidra).
- Short-acting insulin. Sometimes called regular insulin, this type starts working around 30 minutes after injection. It reaches peak effect at 90 to 120 minutes and lasts about 4 to 6 hours. Examples are human insulin (Humulin R, Novolin R).
- Intermediate-acting insulin. Also called NPH insulin, this type of insulin starts working in about 1 to 3 hours. It reaches peak effect at 6 to 8 hours and lasts 12 to 24 hours. Examples are NPH insulin (Humulin N, Novolin N).
- Long- and ultra-long-acting insulin. This type of insulin may provide coverage for as long as 14 to 40 hours. Examples are glargine (Lantus, Toujeo, other), detemir (Levemir) and degludec (Tresiba).
Insulin delivery options
Insulin delivery options include:
- Fine needle and syringe. This looks like a shot you might get in a health care provider's office, but with a smaller syringe and a much thinner, shorter needle.
- Insulin pen with fine needle. This device looks like an ink pen, except the cartridge is filled with insulin. A needle is attached for injection.
-
An insulin pump. This is a small device worn on the outside of your body that you program to deliver specific amounts of insulin throughout the day and when you eat. A tube connects a reservoir of insulin to a catheter that's inserted under the skin of your abdomen.
There's also a tubeless pump option that involves wearing a pod containing the insulin on your body combined with a tiny catheter that's inserted under your skin.
Blood sugar monitoring
You or your child will need to check and record your child's blood sugar at least four times a day. Typically, you or your child test his or her blood glucose before every meal and at bedtime and occasionally during the middle of the night. But you or your child may need to check it more often if your child doesn't have a continuous glucose monitor.
Frequent testing is the only way to make sure that your child's blood sugar level remains within the target range.
Continuous glucose monitoring (CGM)
Continuous glucose monitor and insulin pump
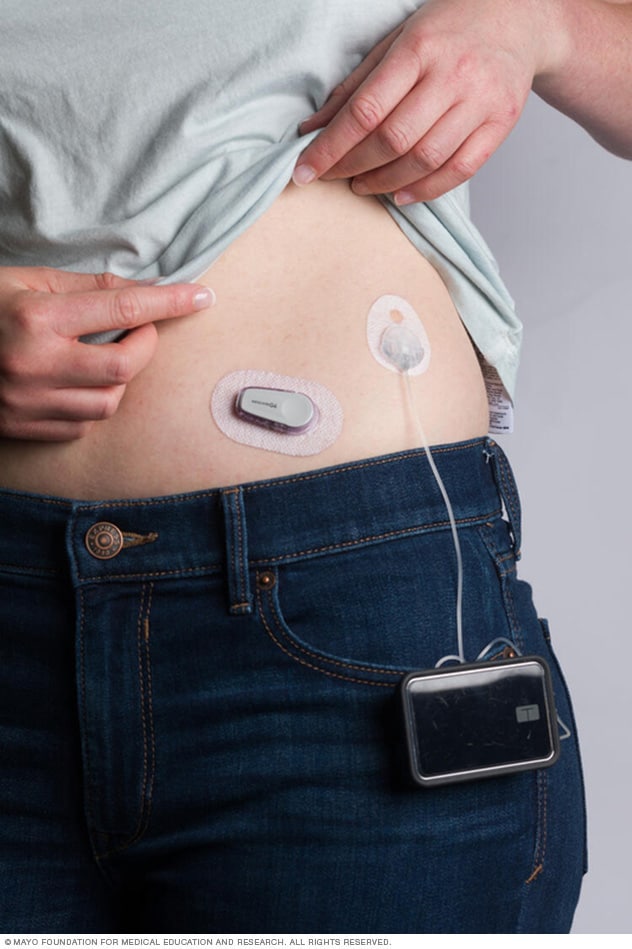
Continuous glucose monitor and insulin pump
A continuous glucose monitor, on the left, is a device that measures your blood sugar every few minutes using a sensor inserted under the skin. An insulin pump, attached to the pocket, is a device that's worn outside of the body with a tube that connects the reservoir of insulin to a catheter inserted under the skin of the abdomen. Insulin pumps are programmed to deliver specific amounts of insulin automatically and when you eat.
Continuous glucose monitoring (CGM) devices measure your blood sugar every few minutes using a temporary sensor inserted under the skin. Some devices show your blood sugar reading at all times on a receiver or your smartphone or smartwatch, while others require that you check your blood sugar by running the receiver over the sensor.
Closed loop system
A closed loop system is a device implanted in the body that links a continuous glucose monitor to an insulin pump. The monitor checks blood sugar levels regularly. The device automatically delivers the right amount of insulin when the monitor shows that it's needed.
The Food and Drug Administration has approved several hybrid closed loop systems for type 1 diabetes. They are called "hybrid" because these systems require some input from the user. For example, you may have to tell the device how many carbohydrates are eaten, or confirm blood sugar levels from time to time.
A closed loop system that doesn't need any user input isn't available yet. But more of these systems currently are in clinical trials.
Healthy eating
Food is a big part of any diabetes treatment plan, but that doesn't mean your child has to follow a strict "diabetes diet." Just like the rest of the family, your child's diet should regularly include foods that are high in nutrition and low in fat and calories, such as:
- Vegetables
- Fruits
- Lean protein
- Whole grains
Your child's registered dietitian can help you create a meal plan that fits your child's food preferences and health goals, as well as help you plan for occasional treats. The dietitian will also teach you how to count carbohydrates in foods so that you can use that information when figuring out insulin doses.
Physical activity
Everyone needs regular aerobic exercise, and children who have type 1 diabetes are no exception.
But remember that physical activity can affect blood sugar. This effect on blood sugar levels can remain for hours after exercise, possibly even overnight. You or your child might need to adjust your child's meal plan or insulin doses for the increased activity.
If your child begins a new activity, check your child's blood sugar more often than usual until you and your child learn how his or her body reacts to the activity.
Make physical activity part of your child's daily routine. Encourage your child to get at least 60 minutes of physical activity daily or, better yet, exercise with your child.
Handling challenges
Blood sugar can sometimes change unpredictably. During these challenges, more frequent blood sugar testing can help identify problems and guide treatment. Ask your child's diabetes treatment team how to handle these and other challenges:
- Picky eating. Very young children with type 1 diabetes might not finish what's on their plates, which can be a problem if they've already received insulin for that food.
- Illness. Sickness has varying effects on children's insulin needs. Hormones produced during illness raise blood sugar levels, but reduced carbohydrate intake due to poor appetite or vomiting lowers the insulin requirement. Your child's health care provider will recommend a flu shot for your child every year and may recommend the pneumonia vaccine as well as the COVID-19 vaccine if your child is age 5 or older.
- Growth spurts and puberty. Just when you've mastered your child's insulin needs, he or she sprouts up seemingly overnight, and suddenly isn't getting enough insulin. Hormones also can affect insulin requirements, particularly for teenage females as they begin to menstruate.
- Sleep. To avoid problems with low blood sugar during the night, you might need to adjust your child's insulin routine and snack times.
- Temporary changes in routine. Despite planning, days don't always stay the same. Check blood sugars often when schedules change unexpectedly. Plan ahead for holidays, special occasions and vacations.
Ongoing medical care
Your child will need regular appointments to ensure good diabetes management. This can include a review of your child's blood sugar patterns, insulin needs, eating and physical activity.
Your health care provider also checks your child's A1C levels. The American Diabetes Association generally recommends an A1C of 7% or lower for all children and teens with diabetes.
Your health care provider also will periodically check your child's:
- Blood pressure
- Growth
- Cholesterol levels
- Thyroid function
- Kidney function
- Feet
- Eyes
Signs of trouble
Despite your best efforts, sometimes problems will arise. Certain short-term complications of type 1 diabetes require immediate care or they could become very serious, including:
- Low blood sugar (hypoglycemia)
- High blood sugar (hyperglycemia)
- Diabetic ketoacidosis (DKA)
Low blood sugar (hypoglycemia)
Hypoglycemia is a blood sugar level below your child's target range. Blood sugar levels can drop for many reasons, including skipping a meal, getting more physical activity than typical or injecting too much insulin. Low blood sugar is not uncommon in people with type 1 diabetes, but if it isn't treated quickly, symptoms will get worse.
Signs and symptoms of low blood sugar include:
- Pallor
- Shakiness
- Hunger
- Sweating
- Irritability and other mood changes
- Difficulty concentrating or confusion
- Dizziness or lightheadedness
- Loss of coordination
- Slurred speech
- Loss of consciousness
- Seizures
Teach your child the symptoms of low blood sugar. When in doubt, he or she should always do a blood sugar test. If a blood glucose meter isn't readily available and your child is having symptoms of a low blood sugar, treat for low blood sugar, and then test as soon as possible.
If your child has a low blood sugar reading:
- Give a fast-acting carbohydrate. Have your child consume 15 to 20 grams of a fast-acting carbohydrate, such as fruit juice, glucose tablets, hard candy, regular (not diet) soda or another source of sugar. Foods with added fat, such as chocolate or ice cream, don't raise blood sugar as quickly because fat slows down the absorption of the sugar.
- Retest blood sugar. Retest your child's blood sugar in about 15 minutes to make sure it's back in the target range. If it's not, repeat giving a fast-acting carbohydrate and testing in 15 minutes as needed until you get a reading in your child's target range.
- Follow up with a snack or meal. Once the blood sugar is back in the target range, have your child eat a healthy snack or a meal to help prevent another low blood sugar level.
If a low blood sugar causes your child to lose consciousness, an emergency injection of a hormone that stimulates the release of sugar into the blood (glucagon) may be necessary.
High blood sugar (hyperglycemia)
Hyperglycemia is a blood sugar level above your child's target range. Blood sugar levels can rise for many reasons, including illness, eating too much, eating certain types of foods and not taking enough insulin.
Signs and symptoms of high blood sugar include:
- Frequent urination
- Increased thirst or dry mouth
- Blurred vision
- Fatigue
- Nausea
If you suspect a high blood sugar level, test your child's blood sugar. If the blood sugar is higher than the target range, follow your child's diabetes treatment plan or check with your child's health care provider. High blood sugar levels don't come down quickly, so ask how long to wait until you check the blood sugar again.
If your child has a blood sugar reading above 240 mg/dL (13.3 mmol/L), your child should use an over-the-counter ketone test kit to check for ketones.
Diabetic ketoacidosis (DKA)
A severe lack of insulin causes your child's body to break down fat for energy. This causes the body to produce a substance called ketones. Excess ketones build up in your child's blood, creating a potentially life-threatening condition known as diabetic ketoacidosis.
Signs and symptoms of DKA include:
- Thirst or very dry mouth
- Increased urination
- Dry or flushed skin
- Nausea, vomiting or abdominal pain
- A sweet, fruity smell on your child's breath
- Confusion
If you suspect DKA, check your child's urine for excess ketones. If the ketone levels are high, call your child's health care provider or seek emergency care.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Following a diabetes treatment plan requires 24-hour care and significant lifestyle changes. Careful management of type 1 diabetes helps reduce your child's risk of serious complications.
As your child gets older:
- Encourage him or her to take an increasingly active role in diabetes management
- Stress the importance of lifelong diabetes care
- Teach your child how to test his or her blood sugar and inject insulin
- Help your child make wise food choices
- Encourage your child to remain physically active
- Foster a relationship between your child and his or her diabetes treatment team
- Make sure your child wears a medical identification tag
The habits you teach your child today will help him or her enjoy an active and healthy life with type 1 diabetes.
School and diabetes
You'll need to work with your child's day care provider or school nurse and teachers to make sure they know the signs and symptoms of high and low blood sugar levels. The school nurse might need to administer insulin or check your child's blood sugar levels.
Federal law protects children with diabetes, and schools must make reasonable accommodations to ensure that all children get a proper education.
Ask your health care provider
Contact your child's health care provider, certified diabetes care and education specialist, or registered dietitian between appointments if you have questions.
Coping and support
If managing your child's diabetes seems overwhelming, take it one day at a time. Some days you'll manage your child's blood sugar ideally and on other days, it may seem as if nothing works well. No one can do it perfectly. But your efforts are worthwhile. Don't forget that you're not alone and that your diabetes treatment team can help.
Your child's emotions
Diabetes can affect your child's emotions both directly and indirectly. Poorly controlled blood sugar can cause behavior changes, such as irritability.
Diabetes can also make your child feel different from other kids. Having to draw blood and give shots sets kids with diabetes apart from their peers. Getting your child together with other children who have diabetes or spending time at a diabetes camp may help your child feel less alone.
Mental health and substance abuse
People with diabetes have an increased risk of depression, anxiety and diabetes-related distress. That's why some diabetes specialists regularly include a social worker or psychologist as part of their diabetes care team.
If you notice that your child or adolescent is persistently sad or pessimistic, or experiences dramatic changes in sleeping habits, weight, friends or school performance, have your child screened for depression.
Rebellion also may be an issue, particularly for teens. A child who has been very good about sticking to his or her diabetes treatment plan may rebel in the teen years by ignoring his or her diabetes care. Additionally, experimenting with drugs, alcohol and smoking can be even more dangerous for people with diabetes.
Support groups
Talking to a counselor or therapist may help your child or you cope with the dramatic lifestyle changes that come with a diagnosis of type 1 diabetes. Your child may find encouragement and understanding in a type 1 diabetes support group for children. Support groups for parents also are available.
If you're interested, your health care provider may be able to recommend a group in your area. Websites that offer support include:
- The American Diabetes Association (ADA). The ADA also offers diabetes camp programs that provide education and support for children and teens with diabetes.
- Juvenile Diabetes Research Foundation (JDRF).
Putting information in perspective
The threat of complications from poorly managed diabetes can be frightening. If you and your child work with your child's health care provider and do your best to manage your child's diabetes, your child will likely live a long and enjoyable life.
Preparing for your appointment
Your child's primary care provider will probably make the initial diagnosis of type 1 diabetes. Hospitalization may be needed to stabilize your child's blood sugar levels.
Your child's long-term diabetes care will likely be handled by a pediatric endocrinologist. Your child's health care team also generally includes a certified diabetes care and education specialist, a registered dietitian, and a social worker.
Here's some information to help you get ready for your appointment.
What you can do
Before your appointment take these steps:
- Make a list of any concerns you have about your child's well-being.
- Ask a family member or friend to join you. Managing diabetes requires you to remember a lot of information. Someone who accompanies you may recall something that you missed or forgot.
- Make a list of questions to ask your health care provider. Ask your health care provider for a referral to a certified diabetes care and education specialist and a registered dietitian to provide additional education about managing diabetes.
Topics you might want to discuss with your health care team include:
- Blood sugar monitoring — frequency and timing and continuous glucose monitors
- Insulin therapy — types of insulin used, dose timing and amount
- Insulin administration — shots versus pumps and new diabetes technology
- Low blood sugar — how to recognize and treat
- High blood sugar — how to recognize and treat
- Ketones — testing and treatment
- Nutrition — types of food and their effects on blood sugar
- Carbohydrate counting
- Exercise — adjusting insulin and food intake for activity
- Dealing with special situations — such as at day care, school or summer camp; during illness; and on special occasions, such as sleepovers, holidays and vacations
- Medical management — how often to visit the health care provider and other diabetes care specialists
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, such as:
- How comfortable are you with managing your child's diabetes?
- How often does your child have low blood sugar episodes?
- What's a typical day's diet like?
- How often does your child participate in physical activity?
Sept. 02, 2023