Overview
Thrombocytopenia is a condition in which you have a low blood platelet count. Platelets (thrombocytes) are colorless blood cells that help blood clot. Platelets stop bleeding by clumping and forming plugs in blood vessel injuries.
Thrombocytopenia might occur as a result of a bone marrow disorder such as leukemia or an immune system problem. Or it can be a side effect of taking certain medications. It affects both children and adults.
Thrombocytopenia can be mild and cause few signs or symptoms. In rare cases, the number of platelets can be so low that dangerous internal bleeding occurs. Treatment options are available.
Products & Services
Symptoms
Petechiae
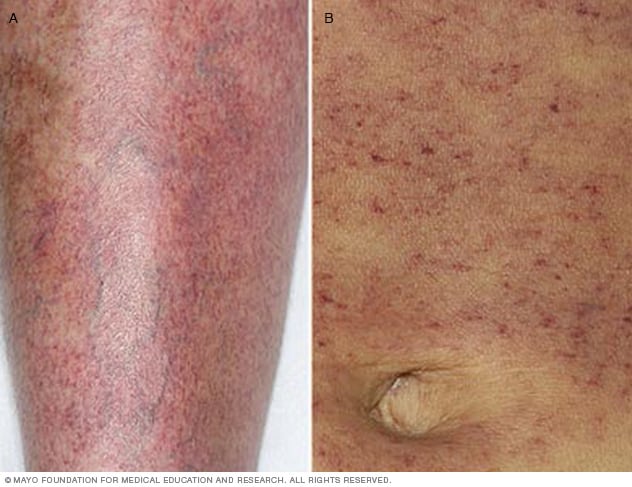
Petechiae
Bleeding into the skin looks like tiny reddish-purple spots, also known as petechiae. Petechiae might look like a rash. Here they appear on a leg (A) and on the stomach area (B).
Thrombocytopenia signs and symptoms may include:
- Easy or excessive bruising (purpura)
- Superficial bleeding into the skin that appears as a rash of pinpoint-sized reddish-purple spots (petechiae), usually on the lower legs
- Prolonged bleeding from cuts
- Bleeding from your gums or nose
- Blood in urine or stools
- Unusually heavy menstrual flows
- Fatigue
- Enlarged spleen
When to see a doctor
Make an appointment with your doctor if you have signs of thrombocytopenia that worry you.
Bleeding that won't stop is a medical emergency. Seek immediate help for bleeding that can't be controlled by the usual first-aid techniques, such as applying pressure to the area.
Causes
Enlarged spleen
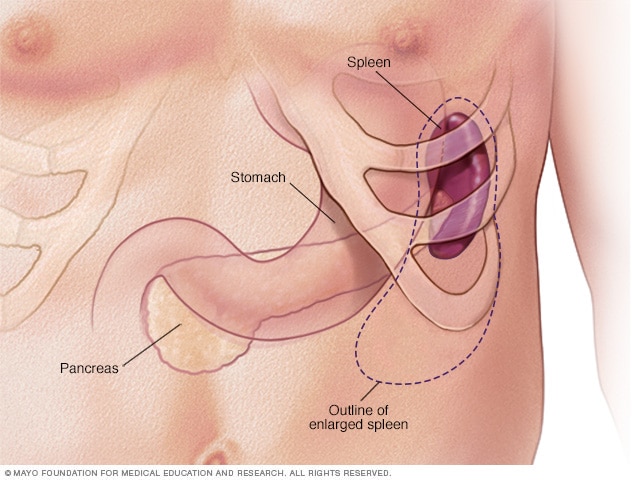
Enlarged spleen
The spleen is a small organ usually about the size of your fist. But a number of conditions, including liver disease and some cancers, can cause your spleen to become enlarged.
Thrombocytopenia means you have fewer than 150,000 platelets per microliter of circulating blood. Because each platelet lives only about 10 days, your body normally renews your platelet supply continually by producing new platelets in your bone marrow.
Thrombocytopenia rarely is inherited; or it can be caused by a number of medications or conditions. Whatever the cause, circulating platelets are reduced by one or more of the following processes: trapping of platelets in the spleen, decreased platelet production or increased destruction of platelets.
Trapped platelets
The spleen is a small organ about the size of your fist situated just below your rib cage on the left side of your abdomen. Normally, your spleen works to fight infection and filter unwanted material from your blood. An enlarged spleen — which can be caused by a number of disorders — can harbor too many platelets, which decreases the number of platelets in circulation.
Decreased production of platelets
Platelets are produced in your bone marrow. Factors that can decrease platelet production include:
- Leukemia and other cancers
- Some types of anemia
- Viral infections, such as hepatitis C or HIV
- Chemotherapy drugs and radiation therapy
- Heavy alcohol consumption
Increased breakdown of platelets
Some conditions can cause your body to use up or destroy platelets faster than they're produced, leading to a shortage of platelets in your bloodstream. Examples of such conditions include:
- Pregnancy. Thrombocytopenia caused by pregnancy is usually mild and improves soon after childbirth.
- Immune thrombocytopenia. Autoimmune diseases, such as lupus and rheumatoid arthritis, cause this type. The body's immune system mistakenly attacks and destroys platelets. If the exact cause of this condition isn't known, it's called idiopathic thrombocytopenic purpura. This type more often affects children.
- Bacteria in the blood. Severe bacterial infections involving the blood (bacteremia) can destroy platelets.
- Thrombotic thrombocytopenic purpura. This is a rare condition that occurs when small blood clots suddenly form throughout your body, using up large numbers of platelets.
- Hemolytic uremic syndrome. This rare disorder causes a sharp drop in platelets, destruction of red blood cells and impairs kidney function.
- Medications. Certain medications can reduce the number of platelets in your blood. Sometimes a drug confuses the immune system and causes it to destroy platelets. Examples include heparin, quinine, sulfa-containing antibiotics and anticonvulsants.
Complications
Dangerous internal bleeding can occur when your platelet count falls below 10,000 platelets per microliter. Though rare, severe thrombocytopenia can cause bleeding into the brain, which can be fatal.