Diagnosis
A diagnosis of posterior vaginal prolapse often happens during a pelvic exam of the vagina and rectum.
The pelvic exam might involve:
- Bearing down as if having a bowel movement. Bearing down might cause the prolapse to bulge, revealing its size and location.
- Tightening pelvic muscles as if stopping a stream of urine. This test checks the strength of the pelvic muscles.
You might fill out a questionnaire to assess your condition. Your answers can tell your health care provider about how far the bulge extends into the vagina and how much it affects your quality of life. This information helps guide treatment decisions.
Rarely, you might need an imaging test:
- MRI or an X-ray can determine the size of the tissue bulge.
- Defecography is a test to check how well your rectum empties. The procedure combines the use of a contrasting agent with an imaging study, such as X-ray or MRI.
More Information
Treatment
Types of pessaries
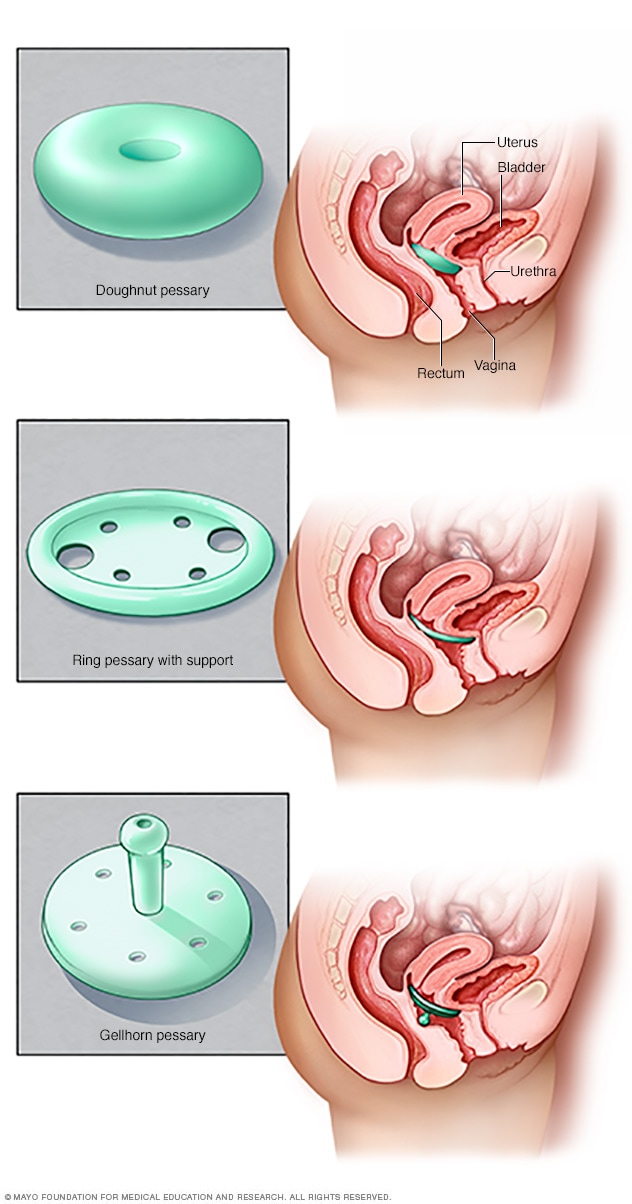
Types of pessaries
Pessaries come in many shapes and sizes. The device fits into the vagina and provides support to vaginal tissues displaced by pelvic organ prolapse. A health care provider can fit a pessary and help provide information about which type would work best.
Treatment depends on how severe your prolapse is. Treatment might involve:
- Observation. If the posterior vaginal prolapse causes few or no symptoms, simple self-care measures — such as performing Kegel exercises to strengthen pelvic muscles — might give relief.
- Pessary. A vaginal pessary is a silicone device that you put into the vagina. The device helps support bulging tissues. A pessary must be removed regularly for cleaning.
Surgery
Surgery to fix the prolapse might be needed if:
- Pelvic floor strengthening exercises or using a pessary doesn't control your prolapse symptoms well enough.
- Other pelvic organs are prolapsed along with the rectum, and your symptoms really bother you. Surgery to fix each prolapsed organ can be done at the same time.
Surgery often involves removing extra, stretched tissue that forms the vaginal bulge. Then stitches are placed to support pelvic structures. When the uterus is also prolapsed, the uterus might need to be removed (hysterectomy). More than one type of prolapse can be repaired during the same surgery.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Sometimes, self-care measures provide relief from prolapse symptoms. You could try to:
- Perform Kegel exercises to strengthen pelvic muscles
- Avoid constipation by eating high-fiber foods, drinking plenty of fluids and, if needed, taking a fiber supplement
- Avoid bearing down during bowel movements
- Avoid heavy lifting
- Control coughing
- Achieve and maintain a healthy weight
Kegel exercises
Kegel exercises strengthen pelvic floor muscles. A strong pelvic floor provides better support for pelvic organs. It also might relieve bulge symptoms that posterior vaginal prolapse can cause.
To perform Kegel exercises:
- Find the right muscles. To find your pelvic floor muscles, try stopping urine midstream when you use the toilet. Once you know where these muscles are, you can practice these exercises. You can do the exercises in any position, although you might find it easiest to do them lying down at first.
- Perfect your technique. To do Kegels, imagine you are sitting on a marble and tighten your pelvic muscles as if you're lifting the marble. Try it for three seconds at a time, then relax for a count of three.
- Maintain your focus. For best results, focus on tightening only your pelvic floor muscles. Be careful not to flex the muscles in your abdomen, thighs or buttocks. Avoid holding your breath. Instead, breathe freely during the exercises.
- Repeat three times a day. Aim for at least three sets of 10 to 15 repetitions a day.
Kegel exercises may be most successful when they're taught by a physical therapist or nurse practitioner and reinforced with biofeedback. Biofeedback uses monitoring devices to let you know that you're tightening the right set of muscles in the right way.
Preparing for your appointment
For posterior vaginal prolapse, you might need to see a doctor who specializes in female pelvic floor conditions. This type of doctor is called a urogynecologist.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms and when they began
- All medicines, vitamins and supplements you take, including doses
- Key personal and medical information, including other conditions, recent life changes and stressors
- Questions to ask your health care provider
For posterior vaginal prolapse, some basic questions to ask your care provider include:
- What can I do at home to ease my symptoms?
- Should I restrict any activities?
- What are the chances that the bulge will grow if I don't do anything?
- What treatment approach do you think would be best for me?
- What are the chances that my condition will come back after I have surgery?
- What are the risks of surgery?
Be sure to ask any other questions that occur to you during your appointment.
What to expect from your health care provider
Your provider is likely to ask you a number of questions, including:
- Do you have pelvic pain?
- Do you ever leak urine?
- Have you had a severe or ongoing cough?
- Do you do any heavy lifting in your job or daily activities?
- Do you strain during bowel movements?
- Has anyone in your family ever had pelvic organ prolapse or other pelvic problems?
- How many children have you given birth to? Were your deliveries vaginal?
- Do you plan to have children in the future?
Aug. 10, 2022