Overview
Overactive bladder, also called OAB, causes sudden urges to urinate that may be hard to control. There might be a need to pass urine many times during the day and night. There also might be loss of urine that isn't intended, called urgency incontinence.
People with an overactive bladder might feel self-conscious. That can cause them to keep away from others or limit their work and social life. The good news is that it can be treated.
Simple behavior changes might manage symptoms of an overactive bladder. These might include changes in diet, urinating on a certain schedule and using pelvic floor muscles to control the bladder. There also are other treatments to try.
Products & Services
Symptoms
If you have an overactive bladder, you may:
- Feel a sudden urge to urinate that's hard to control.
- Lose urine without meaning to after an urgent need to urinate, called urgency incontinence.
- Urinate often. This can mean eight or more times in 24 hours.
- Wake up more than twice a night to urinate, called nocturia.
Even if you can get to the toilet in time when you feel an urge to urinate, having to urinate often during day and night can disrupt your life.
When to see a doctor
Although common among older adults, overactive bladder isn't a typical part of aging. It might not be easy to talk about your symptoms. But if the symptoms distress you or disrupt your life, talk to your healthcare professional. There are treatments that might help.
Causes
How a healthy bladder works
Female urinary system
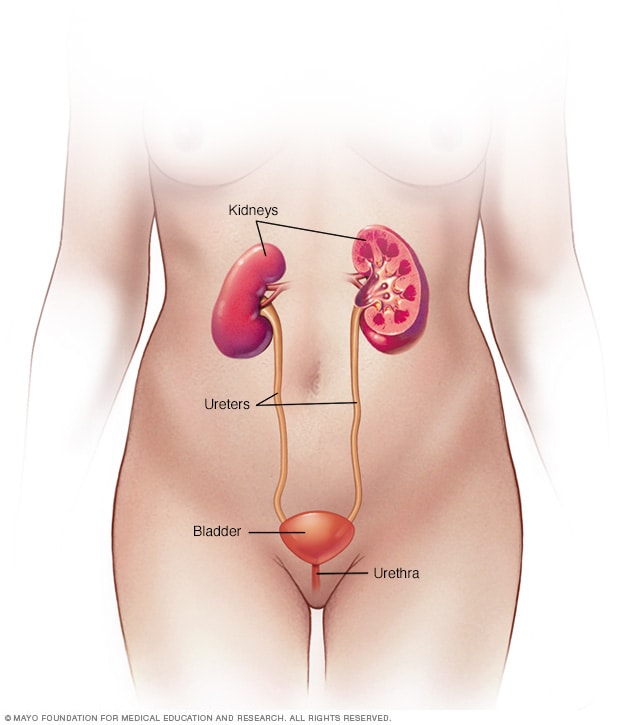
Female urinary system
Your urinary system includes the kidneys, ureters, bladder and urethra. The urinary system removes waste from the body through urine. The kidneys are located toward the back of the upper abdomen. They filter waste and fluid from the blood and produce urine. Urine moves from the kidneys through narrow tubes to the bladder. These tubes are called the ureters. The bladder stores urine until it's time to urinate. Urine leaves the body through another small tube called the urethra.
Male urinary system
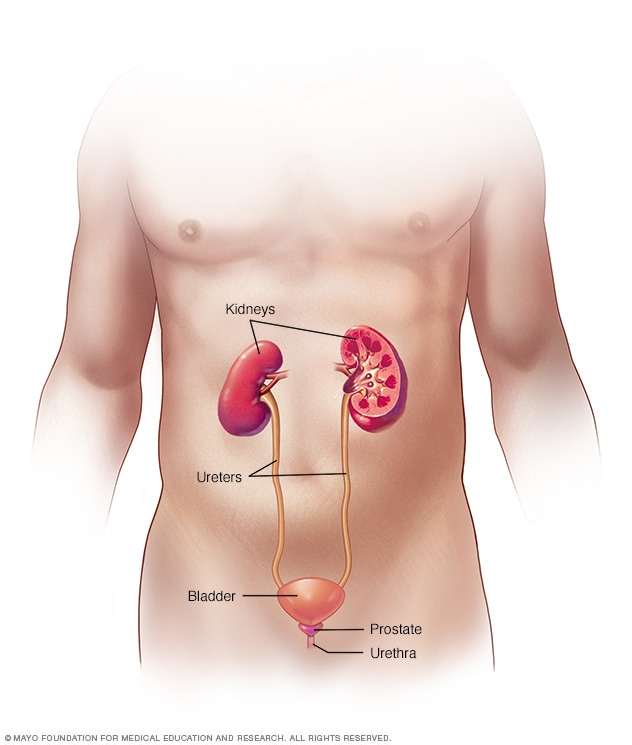
Male urinary system
Your urinary system includes the kidneys, ureters, bladder and urethra. The urinary system removes waste from the body through urine. The kidneys are located toward the back of the upper abdomen. They filter waste and fluid from the blood and produce urine. Urine moves from the kidneys through narrow tubes to the bladder. These tubes are called the ureters. The bladder stores urine until it's time to urinate. Urine leaves the body through another small tube called the urethra.
The kidneys make urine, which drains into the bladder. When urinating, urine passes from the bladder through a tube called the urethra (u-REE-thruh). A muscle in the urethra called the sphincter opens to release urine out of the body.
In people assigned female at birth, the urethral opening is just above the vaginal opening. In people assigned male at birth, the urethral opening is at the tip of the penis.
As the bladder fills, nerve signals sent to the brain trigger the need to urinate. When urinating, these nerve signals cause the pelvic floor muscles and the muscles of the urethra, called the urinary sphincter muscles, to relax. The muscles of the bladder tighten, also called contract, pushing the urine out.
Involuntary bladder contractions
Overactive bladder happens when the muscles of the bladder start to tighten on their own even when the amount of urine in the bladder is low. These are called involuntary contractions. They cause an urgent need to urinate.
Several conditions may be a part of overactive bladder, including:
- Conditions that affect the bladder, such as tumors or bladder stones.
- Conditions that affect the brain and spinal cord, such as stroke and multiple sclerosis.
- Diabetes.
- Factors that get in the way of urine leaving the bladder, such as an enlarged prostate, constipation or having had surgery to treat lack of control over urinating, called incontinence.
- Hormonal changes during menopause.
- Urinary tract infections, which can cause symptoms like those of an overactive bladder.
Overactive bladder symptoms also may be linked to:
- Cognitive decline due to aging. This can make it harder for the bladder to use the signals it gets from the brain.
- Drinking too much caffeine or alcohol.
- Medicines that cause the body to make a lot of urine or that need to be taken with a lot of fluids.
- Not being able to get to the bathroom quickly.
- Not emptying the bladder all the way. This leads to not enough space in the bladder for more urine.
Sometimes the cause of overactive bladder isn't known.
Risk factors
Aging increases the risk of overactive bladder. So does being female. Conditions such as enlarged prostate and diabetes also can increase the risk.
Many people with declines in thinking ability, such as those who have had a stroke or have Alzheimer's disease, get an overactive bladder. That's because they're less able to notice the symptoms of needing to urinate. Drinking fluids on a schedule, timing and prompting urination, absorbent garments, and bowel programs can help manage the condition.
Some people with an overactive bladder also have trouble with bowel control. Tell your healthcare professional if you're having trouble controlling your bowels.
Complications
Any type of incontinence can affect quality of life. If your overactive bladder symptoms disrupt your life, you might also have:
- Anxiety.
- Emotional distress or depression.
- Sexual problems.
- Sleep disturbances and interrupted sleep cycles.
People assigned female at birth who have an overactive bladder also may have a condition called mixed incontinence. This has both urgency and stress incontinence.
Stress incontinence is the sudden loss of urine from physical movement or activity that puts pressure on the bladder. Examples are coughing, sneezing, laughing or exercising.
Prevention
These healthy lifestyle choices may reduce your risk of overactive bladder:
- Do exercises to make the pelvic floor muscles stronger. These are called Kegel exercises.
- Get regular, daily physical activity and exercise.
- Limit caffeine and alcohol.
- Maintain a healthy weight.
- Manage ongoing, called chronic, conditions, such as diabetes, that might add to overactive bladder symptoms.
- Quit smoking.