Diagnosis
Meningioma
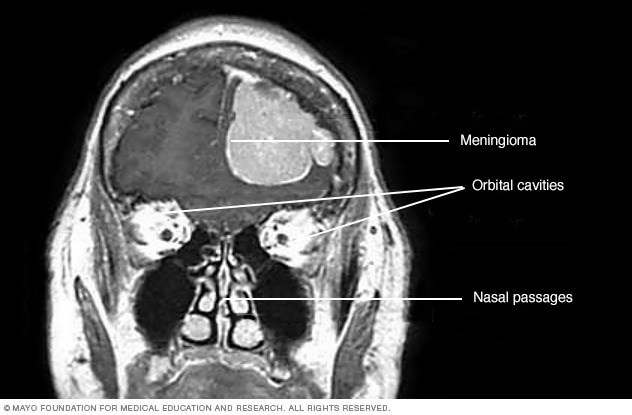
Meningioma
This contrast-enhanced MRI scan of a person's head shows a meningioma. This meningioma has grown large enough to push down into the brain tissue.
A meningioma can be hard to diagnose because the tumor is often slow growing. Symptoms of a meningioma also may be subtle and thought to be other health conditions or signs of aging.
If your healthcare professional suspects a meningioma, you may be referred to a doctor who specializes in conditions of the brain and spine, called a neurologist.
To diagnose a meningioma, a neurologist conducts a thorough neurological exam followed by an imaging test with contrast dye, such as:
- CT scan. CT scans take X-rays that make cross-sectional images of a full picture of the brain. Sometimes an iodine-based dye is used to make the picture easier to read.
- MRI scan. With this imaging study, a magnetic field and radio waves create cross-sectional images of the structures in the brain. MRI scans provide a more detailed picture of the brain and meningiomas.
Sometimes, a sample of the tumor sent to a lab for study, called a biopsy, may be needed to rule out other types of tumors and confirm a meningioma diagnosis.
Treatment
Treatment for a meningioma depends on many factors, including:
- The size of the meningioma and where it is.
- The rate of growth of the tumor.
- Your age and overall health.
- Your goals for treatment.
Wait-and-see approach
Not everyone with a meningioma needs treatment right away. A small, slow-growing meningioma that isn't causing symptoms may not need treatment.
If the plan is for you not to have treatment for a meningioma, you'll likely have brain scans at times to assess your meningioma and look for signs that it's growing.
If your healthcare provider finds that the meningioma is growing and needs to be treated, you have several treatment choices.
Surgery
If the meningioma causes symptoms or shows signs that it's growing, your healthcare professional may suggest surgery.
Surgeons work to remove the entire meningioma. But because a meningioma may be near fragile structures in the brain or spinal cord, it isn't always possible to remove the entire tumor. Then, surgeons remove as much of the meningioma as they can.
The type of treatment, if any, you need after surgery depends on several factors.
- If no visible tumor remains, then no further treatment may be needed. But you will have follow-up scans from time to time.
- If the tumor is benign and only a small piece remains, then your healthcare professional may suggest follow-up scans only. Some small leftover tumors may be treated with a form of radiation treatment called stereotactic radiosurgery.
- If the tumor is irregular or cancer, you'll likely need radiation.
Surgery may pose risks including infection and bleeding. The risks of your surgery will depend on where your meningioma is. For instance, surgery to remove a meningioma from around the optic nerve can lead to vision loss. Ask your surgeon about the risks of your surgery.
Radiation therapy
If the entire meningioma can't be removed surgically, your healthcare professional may suggest radiation therapy after or instead of surgery.
The goal of radiation therapy is to destroy any meningioma cells that are left and reduce the chance that the meningioma may come back. Radiation therapy uses a large machine to aim high-powered energy beams at the tumor cells.
Advances in radiation therapy increase the dose of radiation to the meningioma while giving less radiation to healthy tissue. Radiation therapy types for meningiomas include:
- Stereotactic radiosurgery (SRS). This type of radiation treatment aims several beams of powerful radiation at a precise point. Despite its name, radiosurgery doesn't involve scalpels or cuts. Radiosurgery most often is done in an outpatient setting in a few hours. Radiosurgery may be a choice for people with meningiomas that can't be removed with conventional surgery or for meningiomas that come back despite treatment.
- Fractionated stereotactic radiotherapy (SRT). This type gives radiation in small fractions over time, such as one treatment a day for 30 days. This approach may be used for tumors too large for radiosurgery or those in an area where radiosurgery is too strong, such as near the optic nerve.
- Intensity-modulated radiation therapy (IMRT). This uses computer software to lower the intensity of radiation to the meningioma site. This may be used for meningiomas that are near sensitive brain structures or those with a complex shape.
- Proton beam radiation. This uses radioactive protons aimed right at the tumor. This type lessens damage to the tissue around the tumor.
Medicines
Medicine therapy, also called chemotherapy, rarely is used to treat meningiomas. But it may be used when the meningioma doesn't respond to surgery and radiation.
There isn't a widely used chemotherapy approach to the treatment of meningiomas. But researchers are studying other targeted approaches.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Alternative medicine
Alternative medicine treatments don't treat meningioma. But some may help give relief from treatment side effects. Or they might help you cope with the stress of having a meningioma.
Alternative medicine therapies that may be helpful include:
- Acupuncture.
- Hypnosis.
- Massage.
- Meditation.
- Music therapy.
- Relaxation exercises.
Discuss choices with your healthcare professional.
Coping and support
A meningioma diagnosis can disrupt your life. You have visits to doctors and surgeons as you prepare for your treatment. To help you cope, try to:
-
Learn all you can about meningiomas. Ask your healthcare team where you can learn more about meningiomas and your treatment options. Visit your local library and ask a librarian to help you find good sources of information, including online sources.
Write down questions to ask at your next appointment with your healthcare professional. The more you know about your condition, the better able you'll be to decide about your treatment.
-
Build a support network. It can help to have someone to talk with about your feelings. Other people who can support you include social workers and psychologists. Ask your healthcare provider to refer you. Talk with your pastor, rabbi or other spiritual leader.
It also can help to talk with other people with meningiomas. Think about joining a support group, either in person or online. Ask your healthcare team about brain tumor or meningioma support groups in your area. Or contact the American Brain Tumor Association.
-
Take care of yourself. Eat a diet rich in fruits and vegetables. Get moderate exercise daily if your healthcare professional OKs it. Get enough sleep to feel rested.
Reduce stress in your life. Focus on what matters to you. These measures won't cure your meningioma. But they may help you feel better as you recover from surgery or help you cope during radiation therapy.
Preparing for your appointment
You can start by seeing your main healthcare professional. From there, you may be referred to specialists who treat brain disorders, called neurologists and neurosurgeons.
Here's some information to help you prepare for your appointment.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, be sure to ask if there's anything you need to do in advance, such as restrict your diet.
- Write down any symptoms you have, including any that may seem unrelated to the reason for which you scheduled the appointment and when they began.
- Write down key personal information, including any major stresses or recent life changes.
- Make a list of all medicines, vitamins or supplements you take, including doses.
- Take a family member or friend along, if possible. Someone who goes with you can help you remember the information you get.
- Write down questions to ask your healthcare professional.
Preparing a list of questions will help you make the most of your time. For a meningioma, some basic questions to ask include:
- Is my meningioma cancerous?
- How large is my meningioma?
- Is my meningioma growing? How quickly?
- What treatments do you suggest?
- Do I need treatment now? Or is it better to wait and see?
- What are the potential complications of each treatment?
- Are there long-term complications I should know about?
- Should I seek a second opinion? Can you suggest a specialist or hospital that has experience in treating meningiomas?
- Are there any brochures or other printed material that I can have? What websites do you suggest?
- Do I need to decide about treatment right away? How long can I wait?
Be sure to ask all the questions you have.