Overview
Hypoglycemia is a condition in which your blood sugar (glucose) level is lower than the standard range. Glucose is your body's main energy source.
Hypoglycemia is often related to diabetes treatment. But other drugs and a variety of conditions — many rare — can cause low blood sugar in people who don't have diabetes.
Hypoglycemia needs immediate treatment. For many people, a fasting blood sugar of 70 milligrams per deciliter (mg/dL), or 3.9 millimoles per liter (mmol/L), or below should serve as an alert for hypoglycemia. But your numbers might be different. Ask your health care provider.
Treatment involves quickly getting your blood sugar back to within the standard range either with a high-sugar food or drink or with medication. Long-term treatment requires identifying and treating the cause of hypoglycemia.
Products & Services
Symptoms
If blood sugar levels become too low, hypoglycemia signs and symptoms can include:
- Looking pale
- Shakiness
- Sweating
- Headache
- Hunger or nausea
- An irregular or fast heartbeat
- Fatigue
- Irritability or anxiety
- Difficulty concentrating
- Dizziness or lightheadedness
- Tingling or numbness of the lips, tongue or cheek
As hypoglycemia worsens, signs and symptoms can include:
- Confusion, unusual behavior or both, such as the inability to complete routine tasks
- Loss of coordination
- Slurred speech
- Blurry vision or tunnel vision
- Nightmares, if asleep
Severe hypoglycemia may cause:
- Unresponsiveness (loss of consciousness)
- Seizures
When to see a doctor
Seek medical help immediately if:
- You have what might be hypoglycemia symptoms and you don't have diabetes
- You have diabetes and hypoglycemia isn't responding to treatment, such as drinking juice or regular (not diet) soft drinks, eating candy, or taking glucose tablets
Seek emergency help for someone with diabetes or a history of hypoglycemia who has symptoms of severe hypoglycemia or loses consciousness.
Causes
Hypoglycemia occurs when your blood sugar (glucose) level falls too low for bodily functions to continue. There are several reasons why this can happen. The most common reason for low blood sugar is a side effect of medications used to treat diabetes.
Blood sugar regulation
When you eat, your body breaks down foods into glucose. Glucose, the main energy source for your body, enters the cells with the help of insulin — a hormone produced by your pancreas. Insulin allows the glucose to enter the cells and provide the fuel your cells need. Extra glucose is stored in your liver and muscles in the form of glycogen.
When you haven't eaten for several hours and your blood sugar level drops, you will stop producing insulin. Another hormone from your pancreas called glucagon signals your liver to break down the stored glycogen and release glucose into your bloodstream. This keeps your blood sugar within a standard range until you eat again.
Your body also has the ability to make glucose. This process occurs mainly in your liver, but also in your kidneys. With prolonged fasting, the body can break down fat stores and use products of fat breakdown as an alternative fuel.
Possible causes, with diabetes
If you have diabetes, you might not make insulin (type 1 diabetes) or you might be less responsive to it (type 2 diabetes). As a result, glucose builds up in the bloodstream and can reach dangerously high levels. To correct this problem, you might take insulin or other medications to lower blood sugar levels.
But too much insulin or other diabetes medications may cause your blood sugar level to drop too much, causing hypoglycemia. Hypoglycemia can also occur if you eat less than usual after taking your regular dose of diabetes medication, or if you exercise more than you typically do.
Possible causes, without diabetes
Hypoglycemia in people without diabetes is much less common. Causes can include:
- Medications. Taking someone else's oral diabetes medication accidentally is a possible cause of hypoglycemia. Other medications can cause hypoglycemia, especially in children or in people with kidney failure. One example is quinine (Qualaquin), used to treat malaria.
- Excessive alcohol drinking. Drinking heavily without eating can keep the liver from releasing glucose from its glycogen stores into the bloodstream. This can lead to hypoglycemia.
- Some critical illnesses. Severe liver illnesses such as severe hepatitis or cirrhosis, severe infection, kidney disease, and advanced heart disease can cause hypoglycemia. Kidney disorders also can keep your body from properly excreting medications. This can affect glucose levels due to a buildup of medications that lower blood sugar levels.
- Long-term starvation. Hypoglycemia can occur with malnutrition and starvation when you don't get enough food, and the glycogen stores your body needs to create glucose are used up. An eating disorder called anorexia nervosa is one example of a condition that can cause hypoglycemia and result in long-term starvation.
- Insulin overproduction. A rare tumor of the pancreas (insulinoma) can cause you to produce too much insulin, resulting in hypoglycemia. Other tumors also can result in too much production of insulin-like substances. Unusual cells of the pancreas that produce insulin can result in excessive insulin release, causing hypoglycemia.
- Hormone deficiencies. Certain adrenal gland and pituitary tumor disorders can result in an inadequate amount of certain hormones that regulate glucose production or metabolism. Children can have hypoglycemia if they have too little growth hormone.
Hypoglycemia after meals
Hypoglycemia usually occurs when you haven't eaten, but not always. Sometimes hypoglycemia symptoms occur after certain meals, but exactly why this happens is uncertain.
This type of hypoglycemia, called reactive hypoglycemia or postprandial hypoglycemia, can occur in people who have had surgeries that interfere with the usual function of the stomach. The surgery most commonly associated with this is stomach bypass surgery, but it can also occur in people who have had other surgeries.
Complications
Untreated hypoglycemia can lead to:
Hypoglycemia can also cause:
- Dizziness and weakness
- Falls
- Injuries
- Motor vehicle accidents
- Greater risk of dementia in older adults
Hypoglycemia unawareness
Over time, repeated episodes of hypoglycemia can lead to hypoglycemia unawareness. The body and brain no longer produce signs and symptoms that warn of a low blood sugar, such as shakiness or irregular heartbeats (palpitations). When this happens, the risk of severe, life-threatening hypoglycemia increases.
If you have diabetes, recurring episodes of hypoglycemia and hypoglycemia unawareness, your health care provider might modify your treatment, raise your blood sugar level goals and recommend blood glucose awareness training.
A continuous glucose monitor (CGM) is an option for some people with hypoglycemia unawareness. The device can alert you when your blood sugar is too low.
Undertreated diabetes
If you have diabetes, episodes of low blood sugar are uncomfortable and can be frightening. Fear of hypoglycemia can cause you to take less insulin to ensure that your blood sugar level doesn't go too low. This can lead to uncontrolled diabetes. Talk to your health care provider about your fear, and don't change your diabetes medication dose without discussing changes with your health care provider.
Prevention
If you have diabetes
Continuous glucose monitor and insulin pump
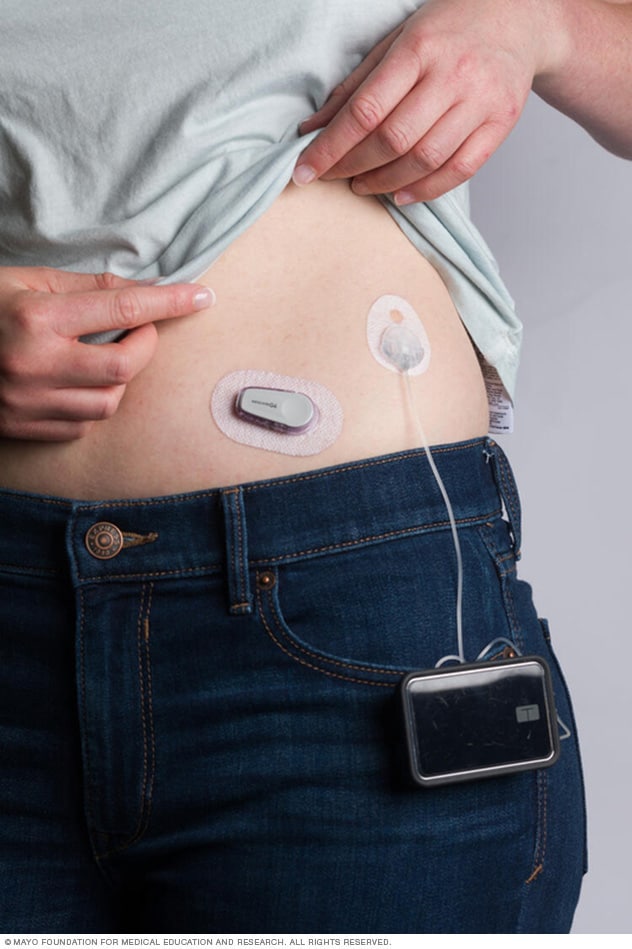
Continuous glucose monitor and insulin pump
A continuous glucose monitor, on the left, is a device that measures your blood sugar every few minutes using a sensor inserted under the skin. An insulin pump, attached to the pocket, is a device that's worn outside of the body with a tube that connects the reservoir of insulin to a catheter inserted under the skin of the abdomen. Insulin pumps are programmed to deliver specific amounts of insulin automatically and when you eat.
Follow the diabetes management plan you and your health care provider have developed. If you're taking new medications, changing your eating or medication schedules, or adding new exercise, talk to your health care provider about how these changes might affect your diabetes management and your risk of low blood sugar.
Learn the signs and symptoms you experience with low blood sugar. This can help you identify and treat hypoglycemia before it gets too low. Frequently checking your blood sugar level lets you know when your blood sugar is getting low.
A continuous glucose monitor (CGM) is a good option for some people. A CGM has a tiny wire that's inserted under the skin that can send blood glucose readings to a receiver. If blood sugar levels are dropping too low, some CGM models will alert you with an alarm.
Some insulin pumps are now integrated with CGMs and can shut off insulin delivery when blood sugar levels are dropping too quickly to help prevent hypoglycemia.
Be sure to always have a fast-acting carbohydrate with you, such as juice, hard candy or glucose tablets so that you can treat a falling blood sugar level before it dips dangerously low.
If you don't have diabetes
For recurring episodes of hypoglycemia, eating frequent small meals throughout the day is a stopgap measure to help prevent blood sugar levels from getting too low. However, this approach isn't advised as a long-term strategy. Work with your health care provider to identify and treat the cause of hypoglycemia.
Nov. 18, 2023