Overview
Emphysema
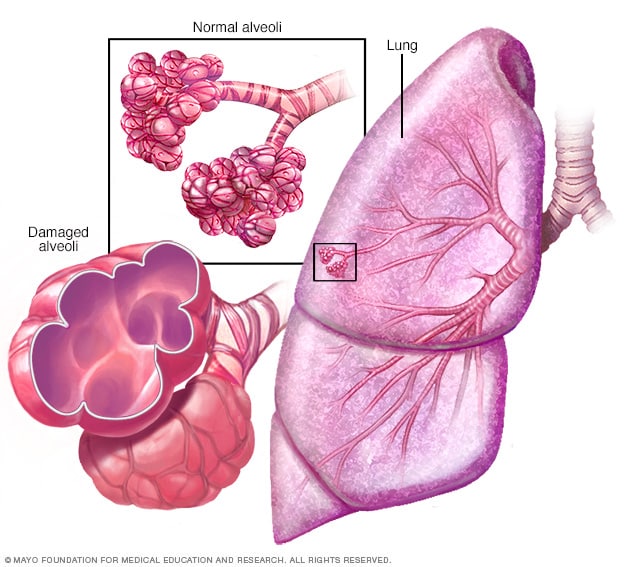
Emphysema
In emphysema, the inner walls of the lungs' air sacs (alveoli) are damaged, causing them to eventually rupture. This creates one larger air space instead of many small ones and reduces the surface area available for the exchange of oxygen and carbon dioxide.
Emphysema is a lung condition that causes shortness of breath. In people with emphysema, the air sacs in the lungs (alveoli) are damaged. Over time, the inner walls of the air sacs weaken and rupture — creating larger air spaces instead of many small ones. This reduces the surface area of the lungs and, in turn, the amount of oxygen that reaches your bloodstream.
When you exhale, the damaged alveoli don't work properly and old air becomes trapped, leaving no room for fresh, oxygen-rich air to enter.
Most people with emphysema also have chronic bronchitis. Chronic bronchitis is inflammation of the tubes that carry air to your lungs (bronchial tubes), which leads to a persistent cough.
Emphysema and chronic bronchitis are two conditions that make up chronic obstructive pulmonary disease (COPD). Smoking is the leading cause of COPD. Treatment may slow the progression of COPD, but it can't reverse the damage.
Products & Services
Symptoms
You can have emphysema for many years without noticing any signs or symptoms. The main symptom of emphysema is shortness of breath, which usually begins gradually.
You may start avoiding activities that cause you to be short of breath, so the symptom doesn't become a problem until it starts interfering with daily tasks. Emphysema eventually causes shortness of breath even while you're at rest.
When to see a doctor
See your doctor if you've had unexplained shortness of breath for several months, especially if it's getting worse or it's interfering with your daily activities. Don't ignore it by telling yourself it's because you're aging or out of shape. Seek immediate medical attention if:
- You're so short of breath, you can't climb stairs
- Your lips or fingernails turn blue or gray with exertion
- You're not mentally alert
Causes
The main cause of emphysema is long-term exposure to airborne irritants, including:
- Tobacco smoke
- Marijuana smoke
- Air pollution
- Chemical fumes and dust
Rarely, emphysema is caused by an inherited deficiency of a protein that protects the elastic structures in the lungs. It's called alpha-1-antitrypsin deficiency emphysema.
Risk factors
Factors that increase your risk of developing emphysema include:
- Smoking. Emphysema is most likely to develop in cigarette smokers, but cigar and pipe smokers also are susceptible. The risk for all types of smokers increases with the number of years and amount of tobacco smoked.
- Age. Although the lung damage that occurs in emphysema develops gradually, most people with tobacco-related emphysema begin to experience symptoms of the disease between the ages of 40 and 60.
- Exposure to secondhand smoke. Secondhand smoke, also known as passive or environmental tobacco smoke, is smoke that you inadvertently inhale from someone else's cigarette, pipe or cigar. Being around secondhand smoke increases your risk of emphysema.
- Occupational exposure to fumes or dust. If you breathe fumes from certain chemicals or dust from grain, cotton, wood or mining products, you're more likely to develop emphysema. This risk is even greater if you smoke.
- Exposure to indoor and outdoor pollution. Breathing indoor pollutants, such as fumes from heating fuel, as well as outdoor pollutants — car exhaust, for instance — increases your risk of emphysema.
Complications
People who have emphysema are also more likely to develop:
- Collapsed lung (pneumothorax). A collapsed lung can be life-threatening in people who have severe emphysema, because the function of their lungs is already so compromised. This is uncommon but serious when it occurs.
- Heart problems. Emphysema can increase the pressure in the arteries that connect the heart and lungs. This can cause a condition called cor pulmonale, in which a section of the heart expands and weakens.
- Large holes in the lungs (bullae). Some people with emphysema develop empty spaces in the lungs called bullae. They can be as large as half the lung. In addition to reducing the amount of space available for the lung to expand, giant bullae can increase your risk of pneumothorax.
Prevention
To prevent emphysema, don't smoke and avoid breathing secondhand smoke. Wear a mask to protect your lungs if you work with chemical fumes or dust.