Diagnosis
Spirometer
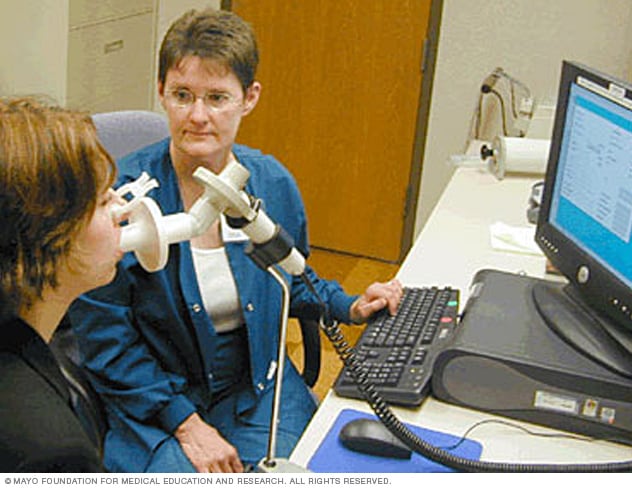
Spirometer
A spirometer is a diagnostic device that measures the amount of air you can breathe in and out and the time it takes you to breathe out completely after you take a deep breath.
To find out if you have emphysema, your doctor or other healthcare professional asks about your medical and family history, smoking, and whether you're often around other lung irritants. Your healthcare professional does a physical exam that includes listening to your lungs. You may have imaging tests, lung function tests and lab tests.
Imaging tests
- Chest X-ray. This test may show some lung changes caused by emphysema. It also can rule out other causes of your symptoms. But the chest X-ray may not show changes even if you have emphysema.
- Computerized tomography (CT) scan. A CT scan combines X-ray images taken from many different angles to create images of structures inside the body. A CT scan gives much greater detail of changes in your lungs than a chest X-ray does. A CT scan of your lungs can show emphysema. It also can help in deciding if you might benefit from surgery. A CT scan can be used to check for lung cancer too.
Lung function tests
Also called pulmonary function tests, lung function tests measure the amount of air you can breathe in and breathe out, and whether your lungs deliver enough oxygen to your blood.
Spirometry is the most common test to diagnose emphysema. During spirometry you blow into a large tube connected to a small machine. This measures how much air your lungs can hold and how fast you can blow the air out of your lungs. Spirometry tells how much airflow is limited.
Other tests include measurement of lung volumes and diffusing capacity, six-minute walk test, and pulse oximetry.
Lung function tests and imaging tests can show whether you have emphysema. And they also can be used to check your condition over time and see how well treatments are working.
Lab tests
Blood tests aren't used to diagnose emphysema, but they may give more information about your condition, find the cause of your symptoms or rule out other conditions.
- Arterial blood gas analysis. This blood test measures how well your lungs are bringing oxygen into your blood and removing carbon dioxide.
- Testing for AAT deficiency. Blood tests can tell if you have the gene change passed down in families that causes the condition alpha-1-antitrypsin deficiency.
Treatment
Treatment is based on how severe your symptoms are and how often you have exacerbations. Effective therapy can control symptoms, slow how fast the condition worsens, lower the risk of complications and exacerbations, and help you lead a more active life.
Quitting smoking
The most important step in any treatment plan for emphysema is to quit all smoking. Stopping smoking can keep emphysema from getting worse and making it harder to breathe. Talk with your healthcare professional about stop-smoking programs, nicotine replacement products and medicines that might help.
Medicine
Several kinds of medicines are used to treat the symptoms and complications of emphysema. You may take some medicines on a regular basis and others as needed. Most medicines for emphysema are given using an inhaler. This small, handheld device delivers the medicine straight to your lungs when you breathe in the fine mist or powder. Talk with your healthcare professional so that you know the right way to use the inhaler prescribed.
Medicines may include:
- Bronchodilators. Bronchodilators are medicines that usually come in inhalers. Bronchodilators relax the muscles around your airways. This can help relieve coughing and make breathing easier. Depending on the severity of your emphysema, you may need a short-acting bronchodilator before activities, a long-acting bronchodilator that you use every day or both.
- Inhaled steroids. Inhaled corticosteroids can lessen airway inflammation and help keep exacerbations from happening. Side effects may include bruising, mouth infections and hoarseness. These medicines are useful if you often have exacerbations of emphysema.
- Combination inhalers. Some inhalers combine bronchodilators and inhaled steroids. There also are combination inhalers that include more than one type of bronchodilator.
- Antibiotics. If you have a bacterial infection, such as acute bronchitis or pneumonia, antibiotics can help.
- Oral steroids. For exacerbations, a short course, for example, of five days of oral corticosteroids may keep symptoms from getting worse. But long-term use of these medicines can have serious side effects, such as weight gain, diabetes, osteoporosis, cataracts and a higher risk of infection.
Lung therapies
- Pulmonary rehabilitation. These programs generally combine education, exercise training, nutrition advice and counseling. You work with a variety of specialists who can tailor your rehabilitation program to meet your needs. Pulmonary rehabilitation may help lessen your breathlessness and allow you to be more active and exercise.
- Nutrition therapy. You may benefit from advice about nutrition by working with a dietitian. In the early stages of emphysema, many people need to lose weight, while people with late-stage emphysema often need to gain weight.
-
Oxygen therapy. If you have severe emphysema with low blood oxygen levels, you may need extra oxygen at home. You can get this extra oxygen to your lungs through a mask or a plastic tubing with tips that fit into your nose. These attach to an oxygen tank. Lightweight, portable units can help some people get around more.
Supplemental oxygen can help your breathing during physical activity and help you sleep better. Many people use oxygen 24 hours a day, even when resting.
Managing exacerbations
When exacerbations occur, you may need added medicines, such as antibiotics, oral steroids or both. You also may need supplemental oxygen or treatment in the hospital. Once symptoms get better, your healthcare professional can talk with you about what steps to take to help stop future exacerbations.
Surgery
Depending on the severity of your emphysema, your healthcare professional may suggest one or more different types of surgery, including:
- Lung volume reduction surgery. In this surgery, the surgeon removes small wedges of damaged lung tissue from the upper lungs. This creates extra space in the chest so that the remaining healthier lung tissue can expand and the muscle that helps in breathing can work better. In some people, this surgery can make their quality of life better and help them live longer.
- Endoscopic lung volume reduction. Also called endobronchial valve surgery, this is a minimally invasive procedure to treat people with emphysema. A tiny one-way endobronchial valve is placed in the lung. Air can leave the damaged part of the lung through the valve, but no new air gets in. This allows the most damaged lung lobe to shrink so that the healthier part of the lung has more space to expand and function.
- Bullectomy. Large air spaces called bullae form in the lungs when the inner walls of the alveoli are destroyed. This leaves one large air sac instead of a cluster of many smaller ones. These bullae can become very large and cause breathing problems. In a bullectomy, the surgeon removes the bullae from the lungs to allow more air flow.
- Lung transplant. A lung transplant may be an option for certain people who meet specific criteria. Getting a new lung can make breathing easier and allow a more active lifestyle. But it's major surgery that has serious risks, such as organ rejection. To try to keep organ rejection from happening, it's necessary to take lifelong medicine that weakens the immune system.
Alpha-1-antitrypsin deficiency
For adults with emphysema related to AAT deficiency, treatment options include those used for people with more-common types of emphysema. Some people can be treated by also replacing the missing AAT protein. This may stop more damage to the lungs.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
If you have emphysema, you can take steps to slow how fast it worsens and to protect yourself from complications:
- Stop smoking. This is the most important step you can take for your overall health. Continuing to smoke can cause more damage to your lungs and worsen emphysema. If you need help giving up smoking, join a stop-smoking program or talk to your healthcare professional about ways to quit. As much as possible, avoid secondhand smoke. Secondhand smoke may add to lung damage.
-
Avoid triggers. These include fumes from paint and automobile exhaust, some cooking odors, certain perfumes, and even burning candles and incense. Change furnace and air conditioner filters regularly to limit pollutants. Get your house checked for radon.
Air pollution also can irritate your lungs, so check daily air quality forecasts before going out. Figure out what may trigger exacerbations for you and avoid them as much as possible.
- Manage your breathing. Talk to your healthcare professional or respiratory therapist about techniques to manage your breathing so it's easier to breathe throughout the day. Also talk about positions that make breathing easier, ways to save your energy such as sitting for tasks when possible, and relaxation strategies to use when you have trouble catching your breath.
- Get regular physical activity. It may seem hard to be physically active when you have trouble breathing. But regular physical activity and exercise can help your overall strength, how long you can be active, and the muscles you use to breathe. Ask your healthcare professional which activities are best for you.
- Eat healthy foods. Eating healthy foods can help you keep your strength. If you're underweight, your healthcare professional may recommend nutritional supplements. If you're overweight, losing weight can greatly help your breathing, especially during activities.
- See your healthcare professional regularly. Stay with your appointment schedule, even if you're feeling fine. It's important to regularly monitor your lung function. Call your healthcare professional if your symptoms get worse or you notice symptoms of infection.
-
Avoid respiratory infections. Do your best to stay away from people who have a cold or the flu. If you must be with large groups of people during cold and flu season, wear a face mask. Also wash your hands often and carry a small bottle of alcohol-based hand sanitizer to use when needed.
And be sure to get your annual flu vaccine in the fall to help prevent infections that can worsen your emphysema. Ask when you need the pneumococcal vaccine, COVID-19 vaccines and other vaccines.
- Protect yourself from cold air. Cold air can cause spasms of the airways, making it even more difficult to breathe. During cold weather, wear a soft scarf or a cold-air mask — available from a pharmacy — over your mouth and nose before going outside. This can warm the air entering your lungs.
Coping and support
Trouble breathing can limit your ability to do daily activities. You may have to give up some activities you used to enjoy. Your family and friends may find they need to adjust to some of these changes too. Here are some suggestions that may help:
- Express your feelings. If you and your family can talk openly about each other's needs, you'll be better able to meet the differences living with emphysema can cause.
- Consider a support group. Think about joining a support group for people with emphysema. Support groups aren't for everyone, but they can be a good source of information and coping strategies. And it can be encouraging to spend time with other people who have the same experiences. Talk with your healthcare professional or check the American Lung Association's website for local and online support groups.
- Get help when needed. Be alert to changes in your mood and your relationships with others, and don't be afraid to ask for help. Talk with your healthcare professional or a mental health professional, if needed. You may benefit from counseling or medicine if you feel overwhelmed or depressed.
Preparing for your appointment
If your primary healthcare professional thinks that you may have emphysema, you'll likely be referred to a doctor who specializes in lung conditions called a pulmonologist.
What you can do
You might want to take a friend or family member with you to your appointment. Someone who goes with you can help you remember information. Take notes if this helps.
Before your appointment, make a list of the following information:
- Symptoms and when they started. Include anything that makes your symptoms worse or better.
- All medicines, vitamins, herbs and supplements you take. Include the doses.
- Family history, such as whether anyone in your family has emphysema or COPD.
- Treatment you've had for emphysema, if any. Include what the treatment was and if it helped.
- Any other medical conditions you have and their treatments.
- If you smoke or have ever smoked. Include whether you're regularly around others who smoke.
- Any jobs where you were around chemical fumes or vapors or industrial dust.
- Questions to ask your healthcare professional.
Questions to ask may include:
- What is likely causing my symptoms?
- What kinds of tests do I need?
- What treatment do you recommend?
- I have other health conditions. How will emphysema affect them?
- Are there any restrictions that I need to follow?
Feel free to ask other questions.
What to expect from your doctor
Your healthcare professional may ask you questions, such as:
- Do you get short of breath easily?
- Does shortness of breath keep you from doing your daily tasks?
- When did you first notice shortness of breath?
- Do you cough every day? If so, when did that start?
- If you smoke, have you tried to quit? Would you like help in quitting?
- Does anyone in your family have emphysema or COPD?
- Have you ever noticed your fingernails or lips turning blue?
- Have you recently gained or lost weight?
Be ready to answer questions so that you have time to talk about what's most important to you.
Nov. 19, 2024