Diagnosis
Spirometer
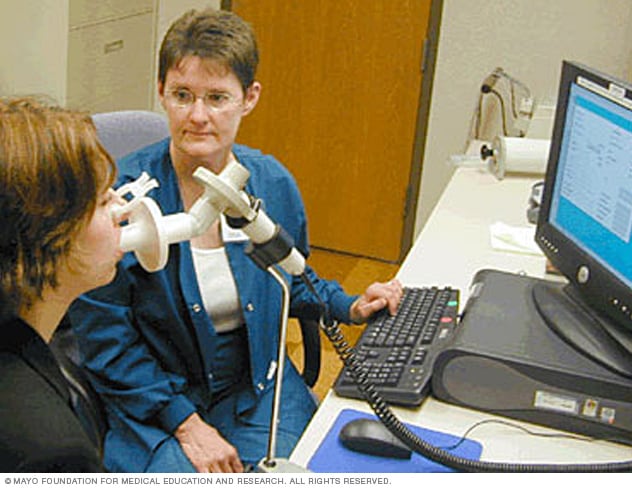
Spirometer
A spirometer is a diagnostic device that measures the amount of air you're able to breathe in and out and the time it takes you to exhale completely after you take a deep breath.
To determine if you have emphysema, your doctor will ask about your medical history and do a physical exam. Your doctor may recommend a variety of tests.
Imaging tests
A chest X-ray can help support a diagnosis of advanced emphysema and rule out other causes of shortness of breath. But the chest X-ray can also show normal findings if you have emphysema.
Computerized tomography (CT) scans combine X-ray images taken from many different directions to create cross-sectional views of internal organs. CT scans can be useful for detecting and diagnosing emphysema. You may also have a CT scan if you're a candidate for lung surgery.
Lab tests
Blood taken from an artery in your wrist can be tested to determine how well your lungs transfer oxygen into, and remove carbon dioxide from, your bloodstream.
Lung function tests
These noninvasive tests measure how much air your lungs can hold and how well the air flows in and out of your lungs. They can also measure how well your lungs deliver oxygen to your bloodstream. One of the most common tests uses a simple instrument called a spirometer, which you blow into.
Treatment
Emphysema and COPD can't be cured, but treatments can help relieve symptoms and slow the progression of the disease.
Medications
Depending upon the severity of your symptoms, your doctor might suggest:
- Bronchodilators. These drugs can help relieve coughing, shortness of breath and breathing problems by relaxing constricted airways.
- Inhaled steroids. Corticosteroid drugs inhaled as aerosol sprays reduce inflammation and may help relieve shortness of breath.
- Antibiotics. If you have a bacterial infection, like acute bronchitis or pneumonia, antibiotics are appropriate.
Therapy
- Pulmonary rehabilitation. A pulmonary rehabilitation program can teach you breathing exercises and techniques that may help reduce your breathlessness and improve your ability to exercise.
- Nutrition therapy. You'll also receive advice about proper nutrition. In the early stages of emphysema, many people need to lose weight, while people with late-stage emphysema often need to gain weight.
- Supplemental oxygen. If you have severe emphysema with low blood oxygen levels, using oxygen regularly at home and when you exercise may provide some relief. Many people use oxygen 24 hours a day. It's usually administered via narrow tubing that fits into your nostrils.
Surgery
Depending on the severity of your emphysema, your doctor may suggest one or more different types of surgery, including:
- Lung volume reduction surgery. In this procedure, surgeons remove small wedges of damaged lung tissue. Removing the diseased tissue helps the remaining lung tissue expand and work more efficiently and helps improve breathing.
- Lung transplant. Lung transplantation is an option if you have severe lung damage and other options have failed.
Lifestyle and home remedies
If you have emphysema, you can take a number of steps to halt its progression and to protect yourself from complications:
- Stop smoking. This is the most important measure you can take for your overall health and the only one that might halt the progression of emphysema. Join a smoking cessation program if you need help giving up smoking. As much as possible, avoid secondhand smoke.
- Avoid other respiratory irritants. These include fumes from paint and automobile exhaust, some cooking odors, certain perfumes, even burning candles and incense. Change furnace and air conditioner filters regularly to limit pollutants.
- Exercise regularly. Try not to let your breathing problems keep you from getting regular exercise, which can significantly increase your lung capacity.
- Protect yourself from cold air. Cold air can cause spasms of the bronchial passages, making it even more difficult to breathe. During cold weather, wear a soft scarf or a cold-air mask — available from a pharmacy — over your mouth and nose before going outside, to warm the air entering your lungs.
- Get recommended vaccinations. Be sure to get an annual flu shot and pneumonia vaccinations as advised by your doctor.
- Prevent respiratory infections. Do your best to avoid direct contact with people who have a cold or the flu. If you have to mingle with large groups of people during cold and flu season, wear a face mask, wash your hands frequently and carry a small bottle of alcohol-based hand sanitizer to use when needed.
Coping and support
The shortness of breath associated with emphysema can severely limit your ability to participate in daily activities. Many people become withdrawn and depressed.
To help you cope with the changes emphysema has made in your life, you might want to:
- Express your feelings. Your emphysema may limit some of your activities and affect your family's plans and routines in ways you can't always anticipate. If you and your family can talk openly about each other's needs, you'll be better able to meet the challenges of living with this disease. Be alert to changes in your mood and your relations with others, and don't be afraid to seek counseling.
- Consider a support group. You may also want to consider joining a support group for people with emphysema. Although support groups aren't for everyone, they can be a good source of information and coping strategies. And it can be encouraging to spend time with other people in circumstances similar to yours. If you're interested in a support group, talk to your doctor or check the American Lung Association's website for local and online support groups.
Preparing for your appointment
Your first appointment to check for emphysema may be with your primary doctor or with a specialist in lung diseases (pulmonologist).
What you can do
Before your appointment, you might want to write a list that answers the following questions:
- Do you smoke? If so, how many packs a day and when did you start?
- Are you exposed to the smoke of other smokers?
- Have any of your jobs exposed you to chemical fumes or industrial dust?
- Does anyone else in your family have lung problems?
- What medications and supplements do you take regularly?
What to expect from your doctor
Your doctor may ask some of the following questions:
- Do you cough every day? If so, when did that start?
- If you smoke, have you tried to quit?
- When did you first notice shortness of breath?
- Does anyone in your family have emphysema or COPD?
- Does shortness of breath keep you from completing daily tasks?
- Have you ever noticed your fingernails or lips turning blue?
- Have you recently gained or lost weight?