Diagnosis
Type 1 diabetes FAQs
Endocrinologist Yogish Kudva, M.B.B.S., answers the most frequently asked questions about type 1 diabetes.
Hi, I'm Dr. Yogish C Kudva. I'm an endocrinologist at Mayo Clinic and I'm here to answer some of the important questions you may have about type one diabetes.
The best current treatment for type one diabetes is an automated insulin delivery system. This system includes a continuous glucose monitor, insulin pump, and a computer algorithm that continually adjusts insulin responding to the continuous glucose monitoring signal. The patient still has to enter information about the amount of carbohydrate he or she eats at mealtimes to provide the meal time related insulin.
Testing using a glucose meter is not enough because glucose measurements in people with type one diabetes, vary from normal to low and normal to high very rapidly in the course of a day, a continuous glucose monitor is needed to assess whether treatment is effective and also to determine how to improve treatment.
Current guidelines recommend use of a continuous glucose monitor. The percentage of time that is spent daily with glucose between 70 and 180 milligram per deciliter is the main measurement of appropriate treatment. This percentage should be 70% or higher daily. In addition, percentage of time spent with glucose below 70 should be less than four percent and greater than 250 should be less than five percent. Clearly, hemoglobin A1C testing to evaluate adequacy of treatment is not enough.
In certain people with type one diabetes transplantation can be undertaken. This could be pancreas transplantation or transplantation of insulin making cells called islet. Islet transplantation is considered research in the US. Pancreas transplantation is available as a clinical treatment. These patients with hypoglycemia unawareness may benefit from a pancreas transplant. People with type one diabetes who develop recurrent diabetic ketoacidosis may also benefit from a pancreas transplant. People with type one diabetes who have developed kidney failure, could have their lives transformed by transplantation of both the pancreas and the kidney.
There is active research going on to prevent type one diabetes from happening in children and adults who are less than 45 years old. People who are eligible for such research studies are people who have a positive antibody test for type one diabetes and are willing to be in such studies. The treatment being tested is medication that suppresses the immune system. Willing participants would be randomized to receive immune suppressive treatment or placebo treatment. Placebo looks like the medication, but does not do the same thing in the body. Initial research studies have been successful in decreasing the risk of development of type one diabetes in people that have received the immune system suppressing treatment and therefore, larger studies are now being undertaken.
Try to be informed about research going on and treatments that may be approved for type one diabetes. You can get this information through already available publications. Make sure that at least annually you see a physician who is an expert on your disorder. Never hesitate to ask your medical team any questions or concerns you have. Being informed makes all the difference. Thanks for your time and we wish well.
Type 1 diabetes symptoms often start suddenly and are often the reason for checking blood sugar levels. Because symptoms of other types of diabetes and prediabetes come on more gradually or may not be easy to see, the American Diabetes Association (ADA) has developed screening guidelines. The ADA recommends that the following people be screened for diabetes:
- Anyone with a body mass index higher than 25 (23 for Asian Americans), regardless of age, who has additional risk factors. These factors include high blood pressure, non-typical cholesterol levels, an inactive lifestyle, a history of polycystic ovary syndrome or heart disease, and having a close relative with diabetes.
- Anyone older than age 35 is advised to get an initial blood sugar screening. If the results are normal, they should be screened every three years after that.
- Women who have had gestational diabetes are advised to be screened for diabetes every three years.
- Anyone who has been diagnosed with prediabetes is advised to be tested every year.
- Anyone who has HIV is advised to be tested.
Tests for type 1 and type 2 diabetes and prediabetes
-
A1C test. This blood test, which doesn't require not eating for a period of time (fasting), shows your average blood sugar level for the past 2 to 3 months. It measures the percentage of blood sugar attached to hemoglobin, the oxygen-carrying protein in red blood cells. It's also called a glycated hemoglobin test.
The higher your blood sugar levels, the more hemoglobin you'll have with sugar attached. An A1C level of 6.5% or higher on two separate tests means that you have diabetes. An A1C between 5.7% and 6.4% means that you have prediabetes. Below 5.7% is considered normal.
- Random blood sugar test. A blood sample will be taken at a random time. No matter when you last ate, a blood sugar level of 200 milligrams per deciliter (mg/dL) — 11.1 millimoles per liter (mmol/L) — or higher suggests diabetes.
- Fasting blood sugar test. A blood sample will be taken after you haven't eaten anything the night before (fast). A fasting blood sugar level less than 100 mg/dL (5.6 mmol/L) is normal. A fasting blood sugar level from 100 to 125 mg/dL (5.6 to 6.9 mmol/L) is considered prediabetes. If it's 126 mg/dL (7 mmol/L) or higher on two separate tests, you have diabetes.
-
Glucose tolerance test. For this test, you fast overnight. Then, the fasting blood sugar level is measured. Then you drink a sugary liquid, and blood sugar levels are tested regularly for the next two hours.
A blood sugar level less than 140 mg/dL (7.8 mmol/L) is normal. A reading of more than 200 mg/dL (11.1 mmol/L) after two hours means you have diabetes. A reading between 140 and 199 mg/dL (7.8 mmol/L and 11.0 mmol/L) means you have prediabetes.
If your provider thinks you may have type 1 diabetes, they may test your urine to look for the presence of ketones. Ketones are a byproduct produced when muscle and fat are used for energy. Your provider will also probably run a test to see if you have the destructive immune system cells associated with type 1 diabetes called autoantibodies.
Your provider will likely see if you're at high risk for gestational diabetes early in your pregnancy. If you're at high risk, your provider may test for diabetes at your first prenatal visit. If you're at average risk, you'll probably be screened sometime during your second trimester.
Treatment
Depending on what type of diabetes you have, blood sugar monitoring, insulin and oral drugs may be part of your treatment. Eating a healthy diet, staying at a healthy weight and getting regular physical activity also are important parts of managing diabetes.
Treatments for all types of diabetes
An important part of managing diabetes — as well as your overall health — is keeping a healthy weight through a healthy diet and exercise plan:
-
Healthy eating. Your diabetes diet is simply a healthy-eating plan that will help you control your blood sugar. You'll need to focus your diet on more fruits, vegetables, lean proteins and whole grains. These are foods that are high in nutrition and fiber and low in fat and calories. You'll also cut down on saturated fats, refined carbohydrates and sweets. In fact, it's the best eating plan for the entire family. Sugary foods are OK once in a while. They must be counted as part of your meal plan.
Understanding what and how much to eat can be a challenge. A registered dietitian can help you create a meal plan that fits your health goals, food preferences and lifestyle. This will likely include carbohydrate counting, especially if you have type 1 diabetes or use insulin as part of your treatment.
-
Physical activity. Everyone needs regular aerobic activity. This includes people who have diabetes. Physical activity lowers your blood sugar level by moving sugar into your cells, where it's used for energy. Physical activity also makes your body more sensitive to insulin. That means your body needs less insulin to transport sugar to your cells.
Get your provider's OK to exercise. Then choose activities you enjoy, such as walking, swimming or biking. What's most important is making physical activity part of your daily routine.
Aim for at least 30 minutes or more of moderate physical activity most days of the week, or at least 150 minutes of moderate physical activity a week. Bouts of activity can be a few minutes during the day. If you haven't been active for a while, start slowly and build up slowly. Also avoid sitting for too long. Try to get up and move if you've been sitting for more than 30 minutes.
Treatments for type 1 and type 2 diabetes
Treatment for type 1 diabetes involves insulin injections or the use of an insulin pump, frequent blood sugar checks, and carbohydrate counting. For some people with type 1 diabetes, pancreas transplant or islet cell transplant may be an option.
Treatment of type 2 diabetes mostly involves lifestyle changes, monitoring of your blood sugar, along with oral diabetes drugs, insulin or both.
Monitoring your blood sugar
Depending on your treatment plan, you may check and record your blood sugar as many as four times a day or more often if you're taking insulin. Careful blood sugar testing is the only way to make sure that your blood sugar level remains within your target range. People with type 2 diabetes who aren't taking insulin generally check their blood sugar much less often.
People who receive insulin therapy also may choose to monitor their blood sugar levels with a continuous glucose monitor. Although this technology hasn't yet completely replaced the glucose meter, it can lower the number of fingersticks necessary to check blood sugar and provide important information about trends in blood sugar levels.
Even with careful management, blood sugar levels can sometimes change unpredictably. With help from your diabetes treatment team, you'll learn how your blood sugar level changes in response to food, physical activity, medications, illness, alcohol and stress. For women, you'll learn how your blood sugar level changes in response to changes in hormone levels.
Besides daily blood sugar monitoring, your provider will likely recommend regular A1C testing to measure your average blood sugar level for the past 2 to 3 months.
Compared with repeated daily blood sugar tests, A1C testing shows better how well your diabetes treatment plan is working overall. A higher A1C level may signal the need for a change in your oral drugs, insulin regimen or meal plan.
Your target A1C goal may vary depending on your age and various other factors, such as other medical conditions you may have or your ability to feel when your blood sugar is low. However, for most people with diabetes, the American Diabetes Association recommends an A1C of below 7%. Ask your provider what your A1C target is.
Insulin
People with type 1 diabetes must use insulin to manage blood sugar to survive. Many people with type 2 diabetes or gestational diabetes also need insulin therapy.
Many types of insulin are available, including short-acting (regular insulin), rapid-acting insulin, long-acting insulin and intermediate options. Depending on your needs, your provider may prescribe a mixture of insulin types to use during the day and night.
Insulin can't be taken orally to lower blood sugar because stomach enzymes interfere with insulin's action. Insulin is often injected using a fine needle and syringe or an insulin pen — a device that looks like a large ink pen.
An insulin pump also may be an option. The pump is a device about the size of a small cellphone worn on the outside of your body. A tube connects the reservoir of insulin to a tube (catheter) that's inserted under the skin of your abdomen.
Continuous glucose monitor and insulin pump
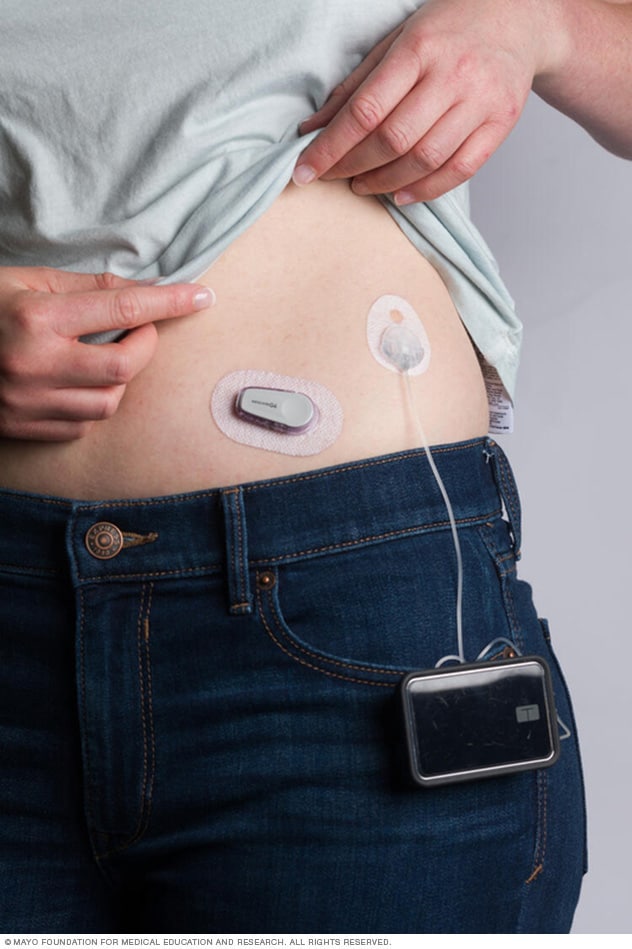
Continuous glucose monitor and insulin pump
A continuous glucose monitor, on the left, is a device that measures your blood sugar every few minutes using a sensor inserted under the skin. An insulin pump, attached to the pocket, is a device that's worn outside of the body with a tube that connects the reservoir of insulin to a catheter inserted under the skin of the abdomen. Insulin pumps are programmed to deliver specific amounts of insulin automatically and when you eat.
A continuous glucose monitor, on the left, is a device that measures blood sugar every few minutes using a sensor inserted under the skin. An insulin pump, attached to the pocket, is a device that's worn outside of the body with a tube that connects the reservoir of insulin to a catheter inserted under the skin of the abdomen. Insulin pumps are programmed to deliver specific amounts of insulin continuously and with food.
A tubeless pump that works wirelessly is also now available. You program an insulin pump to dispense specific amounts of insulin. It can be adjusted to give out more or less insulin depending on meals, activity level and blood sugar level.
A closed loop system is a device implanted in the body that links a continuous glucose monitor to an insulin pump. The monitor checks blood sugar levels regularly. The device automatically delivers the right amount of insulin when the monitor shows that it's needed.
The Food and Drug Administration has approved several hybrid closed loop systems for type 1 diabetes. They are called "hybrid" because these systems require some input from the user. For example, you may have to tell the device how many carbohydrates are eaten, or confirm blood sugar levels from time to time.
A closed loop system that doesn't need any user input isn't available yet. But more of these systems currently are in clinical trials.
Oral or other drugs
Sometimes your provider may prescribe other oral or injected drugs as well. Some diabetes drugs help your pancreas to release more insulin. Others prevent the production and release of glucose from your liver, which means you need less insulin to move sugar into your cells.
Still others block the action of stomach or intestinal enzymes that break down carbohydrates, slowing their absorption, or make your tissues more sensitive to insulin. Metformin (Glumetza, Fortamet, others) is generally the first drug prescribed for type 2 diabetes.
Another class of medication called SGLT2 inhibitors may be used. They work by preventing the kidneys from reabsorbing filtered sugar into the blood. Instead, the sugar is eliminated in the urine.
Transplantation
In some people who have type 1 diabetes, a pancreas transplant may be an option. Islet transplants are being studied as well. With a successful pancreas transplant, you would no longer need insulin therapy.
But transplants aren't always successful. And these procedures pose serious risks. You need a lifetime of immune-suppressing drugs to prevent organ rejection. These drugs can have serious side effects. Because of this, transplants are usually reserved for people whose diabetes can't be controlled or those who also need a kidney transplant.
Bariatric surgery
Some people with type 2 diabetes who are obese and have a body mass index higher than 35 may be helped by some types of bariatric surgery. People who've had gastric bypass have seen major improvements in their blood sugar levels. But this procedure's long-term risks and benefits for type 2 diabetes aren't yet known.
Treatment for gestational diabetes
Controlling your blood sugar level is essential to keeping your baby healthy. It can also keep you from having complications during delivery. In addition to having a healthy diet and exercising regularly, your treatment plan for gestational diabetes may include monitoring your blood sugar. In some cases, you may also use insulin or oral drugs.
Your provider will monitor your blood sugar level during labor. If your blood sugar rises, your baby may release high levels of insulin. This can lead to low blood sugar right after birth.
Treatment for prediabetes
Treatment for prediabetes usually involves healthy lifestyle choices. These habits can help bring your blood sugar level back to normal. Or it could keep it from rising toward the levels seen in type 2 diabetes. Keeping a healthy weight through exercise and healthy eating can help. Exercising at least 150 minutes a week and losing about 7% of your body weight may prevent or delay type 2 diabetes.
Drugs — such as metformin, statins and high blood pressure medications — may be an option for some people with prediabetes and other conditions such as heart disease.
Signs of trouble in any type of diabetes
Many factors can affect your blood sugar. Problems may sometimes come up that need care right away.
High blood sugar
High blood sugar (hyperglycemia in diabetes) can occur for many reasons, including eating too much, being sick or not taking enough glucose-lowering medication. Check your blood sugar level as directed by your provider. And watch for symptoms of high blood sugar, including:
- Urinating often
- Feeling thirstier than usual
- Blurred vision
- Tiredness (fatigue)
- Headache
- Irritability
If you have hyperglycemia, you'll need to adjust your meal plan, drugs or both.
Increased ketones in your urine
Diabetic ketoacidosis is a serious complication of diabetes. If your cells are starved for energy, your body may begin to break down fat. This makes toxic acids known as ketones, which can build up in the blood. Watch for the following symptoms:
- Nausea
- Vomiting
- Stomach (abdominal) pain
- A sweet, fruity smell on your breath
- Shortness of breath
- Dry mouth
- Weakness
- Confusion
- Coma
You can check your urine for excess ketones with a ketones test kit that you can get without a prescription. If you have excess ketones in your urine, talk with your provider right away or seek emergency care. This condition is more common in people with type 1 diabetes.
Hyperglycemic hyperosmolar nonketotic syndrome
Hyperosmolar syndrome is caused by very high blood sugar that turns blood thick and syrupy.
Symptoms of this life-threatening condition include:
- A blood sugar reading over 600 mg/dL (33.3 mmol/L)
- Dry mouth
- Extreme thirst
- Fever
- Drowsiness
- Confusion
- Vision loss
- Hallucinations
This condition is seen in people with type 2 diabetes. It often happens after an illness. Call your provider or seek medical care right away if you have symptoms of this condition.
Low blood sugar (hypoglycemia)
If your blood sugar level drops below your target range, it's known as low blood sugar (diabetic hypoglycemia). If you're taking drugs that lower your blood sugar, including insulin, your blood sugar level can drop for many reasons. These include skipping a meal and getting more physical activity than normal. Low blood sugar also occurs if you take too much insulin or too much of a glucose-lowering medication that causes the pancreas to hold insulin.
Check your blood sugar level regularly and watch for symptoms of low blood sugar, including:
- Sweating
- Shakiness
- Weakness
- Hunger
- Dizziness
- Headache
- Blurred vision
- Heart palpitations
- Irritability
- Slurred speech
- Drowsiness
- Confusion
- Fainting
- Seizures
Low blood sugar is best treated with carbohydrates that your body can absorb quickly, such as fruit juice or glucose tablets.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Diabetes is a serious disease. Following your diabetes treatment plan takes total commitment. Careful management of diabetes can lower your risk of serious or life-threatening complications.
- Commit to managing your diabetes. Learn all you can about diabetes. Build a relationship with a diabetes educator. Ask your diabetes treatment team for help when you need it.
- Choose healthy foods and stay at a healthy weight. If you're overweight, losing just 7% of your body weight can make a difference in your blood sugar control if you have prediabetes or type 2 diabetes. A healthy diet is one with plenty of fruits, vegetables, lean proteins, whole grains and legumes. And limit how much food with saturated fat you eat.
-
Make physical activity part of your daily routine. Regular physical activity can help prevent prediabetes and type 2 diabetes. It can also help those who already have diabetes to maintain better blood sugar control. A minimum of 30 minutes of moderate physical activity — such as brisk walking — most days of the week is recommended. Aim for at least 150 minutes of moderate aerobic physical activity a week.
Getting regular aerobic exercise along with getting at least two days a week of strength training exercises can help control blood sugar more effectively than does either type of exercise alone. Aerobic exercises can include walking, biking or dancing. Resistance training can include weight training and body weight exercises.
Also try to spend less time sitting still. Try to get up and move around for a few minutes at least every 30 minutes or so when you're awake.
Lifestyle recommendations for type 1 and type 2 diabetes
Also, if you have type 1 or type 2 diabetes:
- Identify yourself. Wear a tag or bracelet that says you have diabetes. Keep a glucagon kit nearby in case of a low blood sugar emergency. Make sure your friends and loved ones know how to use it.
- Schedule a yearly physical and regular eye exams. Your regular diabetes checkups aren't meant to replace yearly physicals or routine eye exams. During the physical, your provider will look for any diabetes-related complications and screen for other medical problems. Your eye care specialist will check for signs of eye damage, including retinal damage (retinopathy), cataracts and glaucoma.
-
Keep your vaccinations up to date. High blood sugar can weaken your immune system. Get a flu shot every year. Your provider may recommend the pneumonia and COVID-19 vaccines, as well.
The Centers for Disease Control and Prevention (CDC) also currently recommends hepatitis B vaccination if you haven't previously had it and you're an adult ages 19 to 59 with type 1 or type 2 diabetes.
The most recent CDC guidelines suggest vaccination as soon as possible after diagnosis with type 1 or type 2 diabetes. If you are age 60 or older, have been diagnosed with diabetes, and haven't previously received the vaccine, talk to your provider about whether it's right for you.
- Pay attention to your feet. Wash your feet daily in lukewarm water. Dry them gently, especially between the toes. Moisturize with lotion, but not between the toes. Check your feet every day for blisters, cuts, sores, redness or swelling. Talk to your provider if you have a sore or other foot problem that doesn't heal quickly on its own.
- Control your blood pressure and cholesterol. Eating healthy foods and exercising regularly can help control high blood pressure and cholesterol. Drugs may be needed, too.
- Take care of your teeth. Diabetes may leave you prone to more-serious gum infections. Brush and floss your teeth at least twice a day. And if you have type 1 or type 2 diabetes, schedule regular dental exams. Talk to your dentist right away if your gums bleed or look red or swollen.
- If you smoke or use other types of tobacco, ask your provider to help you quit. Smoking increases your risk of many diabetes complications. Smokers who have diabetes are more likely to die of cardiovascular disease than are nonsmokers who have diabetes. Talk to your provider about ways to stop smoking or to stop using other types of tobacco.
-
If you drink alcohol, do so responsibly. Alcohol can cause either high or low blood sugar. This depends on how much you drink and if you eat at the same time. If you choose to drink, do so only in moderation — one drink a day for women and up to two drinks a day for men — and always with food.
Remember to include the carbohydrates from any alcohol you drink in your daily carbohydrate count. And check your blood sugar levels before going to bed.
- Take stress seriously. The hormones your body may make in response to long-term stress may prevent insulin from working properly. This will raise your blood sugar and stress you even more. Set limits for yourself and prioritize your tasks. Learn relaxation techniques. And get plenty of sleep.
Alternative medicine
Many substances have been shown to improve the body's ability to process insulin in some studies. Other studies fail to find any benefit for blood sugar control or in lowering A1C levels. Because of the conflicting findings, there aren't any alternative therapies that are currently recommended to help everyone to manage blood sugar.
If you decide to try any type of alternative therapy, don't stop taking the drugs that your provider has prescribed. Be sure to discuss the use of any of these therapies with your provider. Make sure that they won't cause bad reactions or interact with your current therapy.
Also, no treatments — alternative or conventional — can cure diabetes. If you're using insulin therapy for diabetes, never stop using insulin unless directed to do so by your provider.
Coping and support
Living with diabetes can be difficult and frustrating. Sometimes, even when you've done everything right, your blood sugar levels may rise. But stick with your diabetes management plan and you'll likely see a positive difference in your A1C when you visit your provider.
Good diabetes management can take a great deal of time and feel overwhelming. Some people find that it helps to talk to someone. Your provider can probably recommend a mental health professional for you to speak with. Or you may want to try a support group.
Sharing your frustrations and triumphs with people who understand what you're going through can be very helpful. And you may find that others have great tips to share about diabetes management.
Your provider may know of a local support group. You can also call the American Diabetes Association at 800-DIABETES (800-342-2383) or the Juvenile Diabetes Research Foundation at 800-533-CURE (800-533-2873).
Preparing for your appointment
You're likely to start by seeing your health care provider if you're having diabetes symptoms. If your child is having diabetes symptoms, you might see your child's health care provider. If blood sugar levels are very high, you'll likely be sent to the emergency room.
If blood sugar levels aren't high enough to put you or your child immediately at risk, you may be referred to a provider trained in diagnosing and treating diabetes (endocrinologist). Soon after diagnosis, you'll also likely meet with a diabetes educator and a registered dietitian to get more information on managing your diabetes.
Here's some information to help you get ready for your appointment and to know what to expect.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask if you need to do anything in advance. This will likely include restricting your diet, such as for a fasting blood sugar test.
- Write down any symptoms you're experiencing, including any that may seem unrelated.
- Write down key personal information, including major stresses or recent life changes. If you're monitoring your glucose values at home, bring a record of the glucose results, detailing the dates and times of testing.
- Make a list of any allergies you have and all medications, vitamins and supplements you're taking.
- Record your family medical history. Be sure to note any relatives who have had diabetes, heart attacks or strokes.
- Bring a family member or friend, if possible. Someone who accompanies you can help you remember information you need.
- Write down questions to ask your provider. Ask about aspects of your diabetes management you're unclear about.
- Be aware if you need any prescription refills. Your provider can renew your prescriptions while you're there.
Preparing a list of questions can help you make the most of your time with your provider. For diabetes, some questions to ask include:
- Are the symptoms I'm having related to diabetes or something else?
- Do I need any tests?
- What else can I do to protect my health?
- What are other options to manage my diabetes?
- I have other health conditions. How can I best manage these conditions together?
- Are there restrictions I need to follow?
- Should I see another specialist, such as a dietitian or diabetes educator?
- Is there a generic alternative to the medicine you're prescribing?
- Are there brochures or other printed material I can take with me? What websites do you recommend?
What to expect from your doctor
Your provider is likely to ask you many questions, such as:
- Can you describe your symptoms?
- Do you have symptoms all the time, or do they come and go?
- How severe are your symptoms?
- Do you have a family history of preeclampsia or diabetes?
- Tell me about your diet.
- Do you exercise? What type and how much?