Diagnosis
Diagnosis of anterior prolapse may involve:
-
A pelvic exam. Your healthcare professional may examine your pelvis. This is to see if there's a tissue bulge in your vagina.
Your healthcare professional may ask you to bear down as you do when passing stool. This shows how bearing down affects the prolapse. You also contract your pelvic floor muscles as you do when stopping the stream of urine. This is to check the strength of the pelvic floor muscles.
- Medical history. This includes medical and surgical history and history of pregnancies.
- Bladder and urine tests. Some people have tests to see how well the bladder empties. Your healthcare professional also may test a urine sample to look for signs of a bladder infection.
Treatment
Types of pessaries
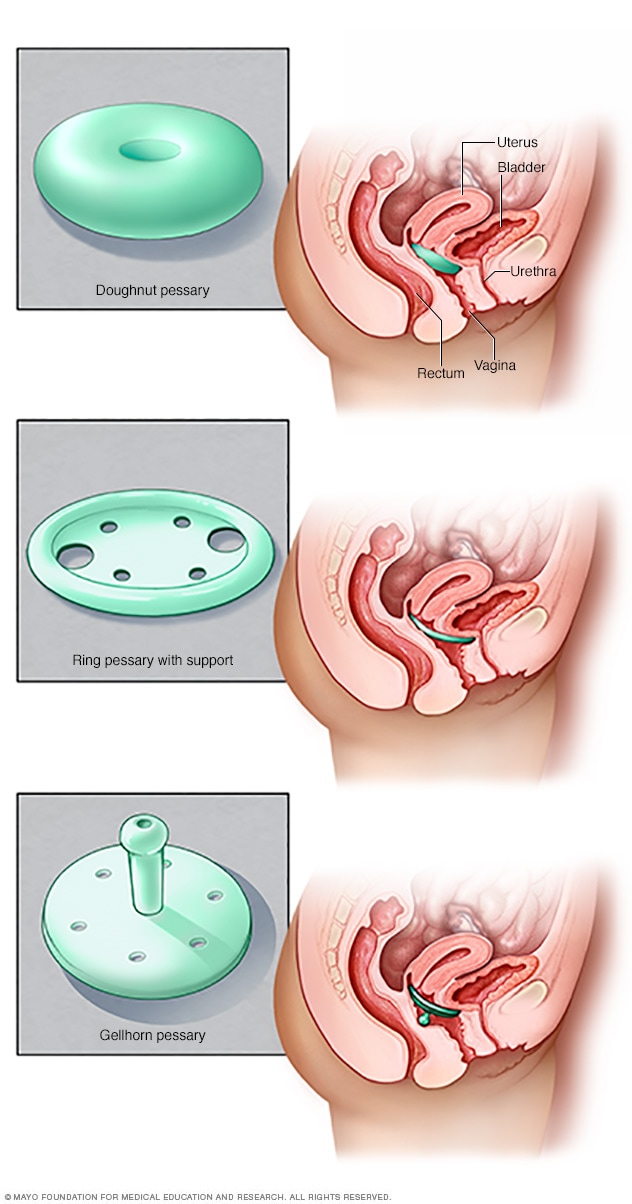
Types of pessaries
Pessaries come in many shapes and sizes. The devices fit into the vagina and support vaginal tissues affected by pelvic organ prolapse. A healthcare professional can fit you for a pessary and help you decide which type would work best for you.
Treatment depends on your symptoms, how much they bother you, the degree of your prolapse and whether you have any related conditions. These might include urinary incontinence or more than one type of pelvic organ prolapse.
People who have few or no symptoms most often don't need treatment. Your healthcare professional may suggest a wait-and-see approach. You have follow-up visits to check the prolapse.
If you have symptoms of anterior prolapse that bother you, treatments may include:
-
Pelvic floor muscle exercises. These exercises also are called Kegel exercises. They strengthen pelvic floor muscles to help them support the bladder and other pelvic organs. Your main healthcare professional or a physical therapist can tell you how to do these exercises.
Having a physical therapist teach you Kegel exercises using biofeedback may be the best way to learn to do them. During biofeedback, a healthcare professional connects you to sensors that let you know that you're doing the exercises right.
-
A device that gives support, called a pessary. A vaginal pessary is a silicone ring put into the vagina to support the bladder. A pessary does not fix the prolapse, but it can help ease symptoms.
A healthcare professional fits you for the device and shows you how to remove it, clean it and put it back in. Many people use pessaries for a time before having surgery. Some people use them when they don't want surgery or surgery is too risky.
Surgery
If other treatments don't help, you may choose surgery.
-
How it's done. Often, a surgeon does the procedure through the vagina. Other ways involve working through small cuts, called incisions, using tiny cameras and surgical tools. This is called laparoscopy. A surgeon may do laparoscopy with robotic help.
Another way to do the surgery is through a cut in the belly, called open surgery.
The surgery involves lifting the bladder back in place and using stitches to hold it there.
- What's done for a prolapsed uterus. For anterior prolapse linked with a prolapsed uterus, your healthcare professional may suggest repairing the prolapse and also removing the uterus, called a hysterectomy. There also are types of these procedures that leave the uterus in place and support the top of the vagina.
If you're pregnant or thinking about becoming pregnant, your healthcare professional may suggest that you not have surgery until you're done having children. Pelvic floor exercises or a pessary may help ease your symptoms in the meantime.
The results of surgery can last many years. But there's some risk of prolapse happening again. That may mean you need another surgery at some point.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Lifestyle and home remedies
Kegel exercises are exercises you can do at home to strengthen your pelvic floor muscles. A stronger pelvic floor gives better support for the pelvic organs and may give relief from symptoms of anterior prolapse.
To do Kegel exercises, follow these steps:
- Tighten your pelvic floor muscles. These are the muscles you use to stop urinating.
- Hold the tightened muscle, called a contraction, for five seconds. Then relax for five seconds. If this is too hard, start by holding for two seconds and relaxing for three seconds.
- Work up to holding the contraction for 10 seconds at a time.
- Repeat the exercises 10 times. Do each set three times a day.
Ask your healthcare professional to teach you how to do Kegel exercises. Once you've learned how, you can do Kegel exercises any time with no one knowing. Try them while sitting at your desk or relaxing on the couch.
To help keep an anterior prolapse from getting worse, you also can try the following:
- Treat and prevent constipation. High-fiber foods can help.
- Don't do heavy lifting. Use good form to lift objects that aren't too heavy. Stand as close as you can to what you're lifting. Don't bend forward to lift. Instead bend your knees so that you use your legs to lift.
- Manage coughing. Get treatment for a long-term cough or bronchitis. And don't smoke.
- Manage your weight. Talk to your healthcare professional about what's a good weight for you. Ask for help with losing weight if you need to.
Preparing for your appointment
Make an appointment with your main healthcare professional or gynecologist if you have symptoms of anterior prolapse that bother you.
Here's some information to help you get ready for your appointment.
What you can do
Make a list of:
- Your symptoms, and when they began.
- Other medical conditions you have and your history of pregnancies.
- All medicines, vitamins and supplements you take, how much you take and how often you take them.
- Questions to ask your healthcare professional.
For anterior prolapse, some basic questions to ask include:
- What is the most likely cause of my symptoms?
- What are other possible causes?
- What tests do I need?
- What treatment do you suggest?
- Should I restrict my activities?
- What can I do at home to ease my symptoms?
- Should I see a specialist?
Be sure to ask all the questions you have.
What to expect from your doctor
Your healthcare professional may ask you questions, such as:
- Do you leak urine?
- Do you have bladder infections often?
- Do you have pain or leak urine during sex?
- Do you have a bad cough?
- Do you strain when passing stool?
- What, if anything, seems to make your symptoms better or worse?
- Do you want to have children in the future?