Overview
Barrett's esophagus

Barrett's esophagus
In Barrett's esophagus, normally flat, pink cells are replaced with a thick, red lining with potential for cancerous changes, thought to be triggered by long-standing gastroesophageal reflux disease (GERD).
Barrett's esophagus is a condition in which the flat pink lining of the swallowing tube that connects the mouth to the stomach (esophagus) becomes damaged by acid reflux, which causes the lining to thicken and become red.
Between the esophagus and the stomach is a critically important valve, the lower esophageal sphincter (LES). Over time, the LES may begin to fail, leading to acid and chemical damage of the esophagus, a condition called gastroesophageal reflux disease (GERD). GERD is often accompanied by symptoms such as heartburn or regurgitation. In some people, this GERD may trigger a change in the cells lining the lower esophagus, causing Barrett's esophagus.
Barrett's esophagus is associated with an increased risk of developing esophageal cancer. Although the risk of developing esophageal cancer is small, it's important to have regular checkups with careful imaging and extensive biopsies of the esophagus to check for precancerous cells (dysplasia). If precancerous cells are discovered, they can be treated to prevent esophageal cancer.
Symptoms
The development of Barrett's esophagus is most often attributed to long-standing GERD, which may include these signs and symptoms:
- Frequent heartburn and regurgitation of stomach contents
- Difficulty swallowing food
- Less commonly, chest pain
Curiously, approximately half of the people diagnosed with Barrett's esophagus report little if any symptoms of acid reflux. So, you should discuss your digestive health with your doctor regarding the possibility of Barrett's esophagus.
When to see a doctor
If you've had trouble with heartburn, regurgitation and acid reflux for more than five years, then you should ask your doctor about your risk of Barrett's esophagus.
Seek immediate help if you:
- Have chest pain, which may be a symptom of a heart attack
- Have difficulty swallowing
- Are vomiting red blood or blood that looks like coffee grounds
- Are passing black, tarry or bloody stools
- Are unintentionally losing weight
Causes
The exact cause of Barrett's esophagus isn't known. While many people with Barrett's esophagus have long-standing GERD, many have no reflux symptoms, a condition often called "silent reflux."
Whether this acid reflux is accompanied by GERD symptoms or not, stomach acid and chemicals wash back into the esophagus, damaging esophagus tissue and triggering changes to the lining of the swallowing tube, causing Barrett's esophagus.
Risk factors
Factors that increase your risk of Barrett's esophagus include:
- Family history. Your odds of having Barrett's esophagus increase if you have a family history of Barrett's esophagus or esophageal cancer.
- Being male. Men are far more likely to develop Barrett's esophagus.
- Being white. White people have a greater risk of the disease than do people of other races.
- Age. Barrett's esophagus can occur at any age but is more common in adults over 50.
- Chronic heartburn and acid reflux. Having GERD that doesn't get better when taking medications known as proton pump inhibitors or having GERD that requires regular medication can increase the risk of Barrett's esophagus.
- Current or past smoking.
- Being overweight. Body fat around your abdomen further increases your risk.
Complications
Esophageal cancer
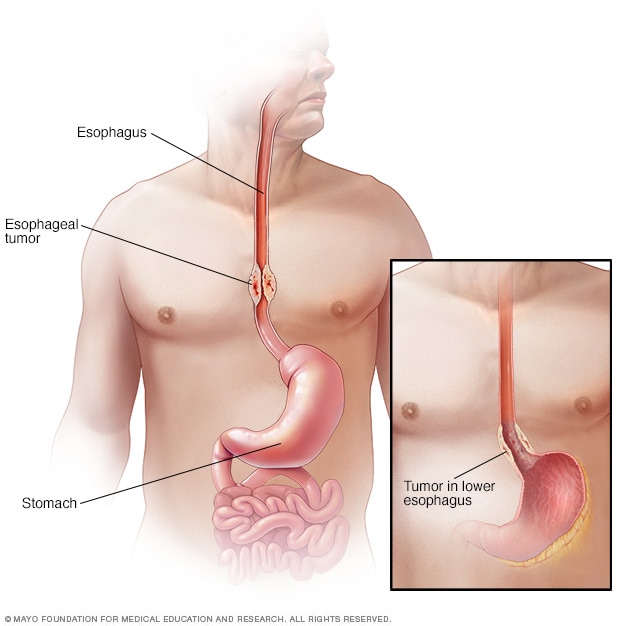
Esophageal cancer
Esophageal cancer most often occurs in the cells that line the inside of the esophagus.
People with Barrett's esophagus have an increased risk of esophageal cancer. The risk is small, even in people who have precancerous changes in their esophagus cells. Fortunately, most people with Barrett's esophagus will never develop esophageal cancer.
Feb. 08, 2023