Diagnosis
Liver biopsy
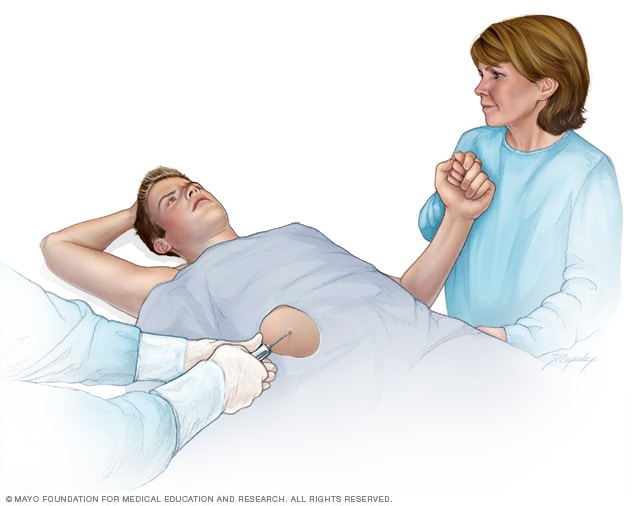
Liver biopsy
A liver biopsy is a procedure to remove a small sample of liver tissue for laboratory testing. A liver biopsy is commonly performed by inserting a thin needle through the skin and into the liver.
Your healthcare professional does a physical exam and asks about your alcohol use, now and in the past. Be honest about your drinking. Your care professional might ask to talk to family members about your drinking.
Diagnosing liver disease might involve these tests:
- Liver function tests.
- Blood tests.
- An ultrasound, CT or MRI scan of the liver.
- A liver biopsy, if other tests and imaging don't give a clear diagnosis or if you are at risk of other causes of hepatitis.
More Information
Treatment
Treatment for alcoholic hepatitis involves quitting drinking as well as therapies to ease the symptoms of liver damage.
Quitting drinking
If you've been diagnosed with alcoholic hepatitis, you need to stop drinking alcohol and never drink alcohol again. It's the only way that might reverse liver damage or keep the disease from getting worse. People who don't stop drinking are likely to have some life-threatening health problems.
If you depend on alcohol and want to stop drinking, your healthcare professional can suggest a therapy that meets your needs. It can be harmful to stop drinking all at once. So discuss a plan with your healthcare professional.
Treatment might include:
- Medicines.
- Counseling.
- Alcoholics Anonymous or other support groups.
- Outpatient or live-in treatment program.
Treatment for malnutrition
Your healthcare professional might suggest a special diet to fix poor nutrition. You might be referred to an expert in diet to manage disease, called a dietitian. A dietitian can suggest ways to eat better to make up for the vitamins and nutrients you lack.
If you have trouble eating, your care professional might suggest a feeding tube. A tube is passed down the throat or through the side and into the stomach. A special nutrient-rich liquid diet is then passed through the tube.
Medicines to reduce liver swelling, called inflammation
These might help severe alcoholic hepatitis:
- Corticosteroids. These medicines might help some people with severe alcoholic hepatitis live longer. However, corticosteroids have serious side effects. They're not likely to be used if you have failing kidneys, stomach bleeding or an infection.
- Pentoxifylline. Your healthcare professional might suggest this medicine f you can't take corticosteroids. How well pentoxifylline works for alcoholic hepatitis isn't clear. Study results differ.
- Other treatment. N-acetylcysteine may help some people with alcoholic hepatitis. More study is needed.
Liver transplant
For many people with severe alcoholic hepatitis, the risk of dying is high without a liver transplant.
In the past, those with alcoholic hepatitis have not been given new livers. This is because of the risk that they'll continue drinking after transplant. But recent studies suggest that well-chosen people with severe alcoholic hepatitis have survival rates after a transplant similar to people with other types of liver disease who get liver transplants.
For transplant to be an option, you would need:
- To find a program that works with people who have alcoholic hepatitis.
- To follow the rules of the program. This includes making a promise not to drink alcohol for the rest of your life.
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Preparing for your appointment
You might be referred to a digestive disease specialist, called a gastroenterologist.
What you can do
When you make the appointment, ask if there's anything you need to do before certain tests, such as not eating or drinking.
Make a list of:
- Your symptoms, including any that don't seem linked to the reason you made the appointment, and when they began.
- All medicines, vitamins and supplements you take, including doses.
- Key medical information, including other conditions you have.
- Key personal information, including recent changes or stressors in your life. Keep track of how much alcohol you drink for a few days for your healthcare professional.
- Questions to ask your healthcare professional.
Have a relative or friend go with you, if possible, to help you remember the information you're given.
Questions to ask your doctor
- What's the most likely cause of my symptoms? Are there other possible causes?
- Do I have any other liver disease?
- Is there scarring of my liver?
- What tests do I need? How do I prepare for them?
- Is my condition likely to go away or be long-lasting?
- What treatment do you suggest?
- I have other health problems. How can I best manage these conditions together?
Be sure to ask all the questions you have about your condition.
What to expect from your doctor
Your healthcare professional is likely to ask you questions, including:
- How bad are your symptoms? Do they come and go, or do you have them all the time?
- Does anything improve your symptoms or make them worse?
- Have you had hepatitis or yellowing of the skin or whites of your eyes?
- Do you use illicit drugs?
- Have you ever felt you should cut down on drinking or felt guilty or bad about your drinking?
- Are your family members or friends worried about your drinking? Have you been arrested or had other problems because of your drinking?
- Do you get angry or upset when anyone talks about your drinking?
- Do you feel guilty about drinking?
- Do you drink in the morning?
Nov. 09, 2023