Diagnosis
Your doctor will ask about your medical history and conduct a physical exam. Then he or she may recommend the following steps:
- IGF-1 measurement. After you've fasted overnight, your doctor will take a blood sample to measure the IGF-1 level in your blood. An elevated IGF-1 level suggests acromegaly.
- Growth hormone suppression test. This is the best method for confirming an acromegaly diagnosis. During this test, your GH blood level is measured both before and after you drink a preparation of sugar (glucose). In people who don't have acromegaly, the glucose drink typically causes the GH level to fall. But if you have acromegaly, your GH level will tend to stay high.
- Imaging. Your doctor may recommend an imaging test, such as magnetic resonance imaging (MRI), to help pinpoint the location and size of a tumor on your pituitary gland. If no pituitary tumors are seen, your doctor may order other imaging tests to look for nonpituitary tumors.
Treatment
Acromegaly treatment varies by person. Your treatment plan will likely depend on the location and size of your tumor, the severity of your symptoms, and your age and overall health.
To help lower your GH and IGF-1 levels, treatment options typically include surgery or radiation to remove or reduce the size of the tumor that is causing your symptoms, and medication to help normalize your hormone levels.
If you're experiencing health problems as a result of acromegaly, your doctor may recommend additional treatments to help manage your complications.
Surgery
Endoscopic transnasal transsphenoidal surgery
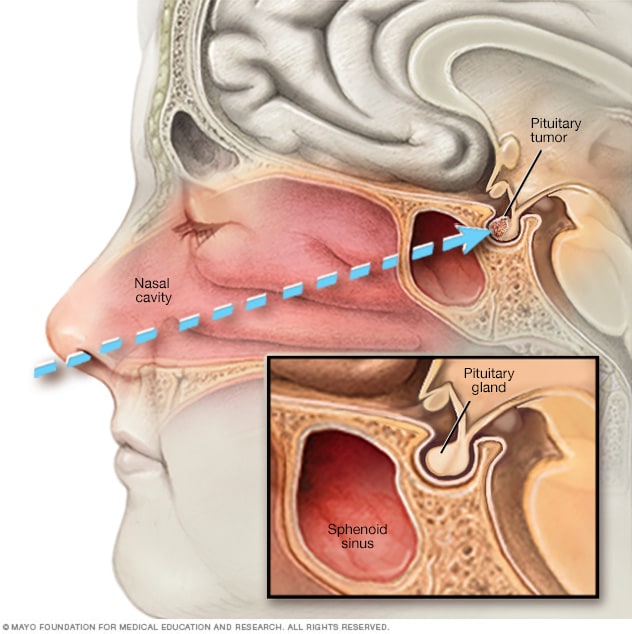
Endoscopic transnasal transsphenoidal surgery
In transnasal transsphenoidal endoscopic surgery, a surgical instrument is placed through the nostril and alongside the nasal septum to access a pituitary tumor.
Doctors can remove most pituitary tumors using a method called transsphenoidal surgery. During this procedure, your surgeon works through your nose to remove the tumor from your pituitary gland. If the tumor causing your symptoms isn't located on your pituitary gland, your doctor will recommend another type of surgery to remove the tumor.
In many cases — especially if your tumor is small — removal of the tumor returns your GH levels to normal. If the tumor was putting pressure on the tissues around your pituitary gland, removing the tumor also helps relieve headaches and vision changes.
In some cases, your surgeon may not be able to remove the entire tumor. If this is the case, you may still have elevated GH levels after surgery. Your doctor may recommend another surgery, medications or radiation treatments.
Medications
Your doctor may recommend one of the following medications — or a combination of medications — to help your hormone levels return to normal:
- Drugs that reduce growth hormone production (somatostatin analogues). In the body, a brain hormone called somatostatin works against (inhibits) GH production. The drugs octreotide (Sandostatin) and lanreotide (Somatuline Depot) are man-made (synthetic) versions of somatostatin. Taking one of these drugs signals the pituitary gland to produce less GH, and may even reduce the size of a pituitary tumor. Typically, these drugs are injected into the muscles of your buttocks (gluteal muscles) once a month by a health care professional.
- Drugs to lower hormone levels (dopamine agonists). The oral medications cabergoline and bromocriptine (Parlodel) may help lower levels of GH and IGF-1 in some people. These drugs may also help decrease tumor size. To treat acromegaly, these medications usually need to be taken at high doses, which can increase the risk of side effects. Common side effects of these drugs include nausea, vomiting, stuffy nose, tiredness, dizziness, sleep problems and mood changes.
- Drug to block the action of GH (growth hormone antagonist). The medication pegvisomant (Somavert) blocks the effect of GH on the body's tissues. Pegvisomant may be particularly helpful for people who haven't had good success with other treatments. Given as a daily injection, this medication can help lower IGF-1 levels and relieve symptoms, but it doesn't lower GH levels or reduce tumor size.
Radiation
If your surgeon wasn't able to remove the whole tumor during surgery, your doctor may recommend radiation treatment. Radiation therapy destroys any lingering tumor cells and slowly reduces GH levels. It may take years for this treatment to noticeably improve acromegaly symptoms.
Radiation treatment often lowers levels of other pituitary hormones, too — not just GH. If you receive radiation treatment, you'll likely need regular follow-up visits with your doctor to make sure that your pituitary gland is working properly, and to check your hormone levels. This follow-up care may last for the rest of your life.
Types of radiation therapy include:
- Conventional radiation therapy. This type of radiation therapy is usually given every weekday over a period of four to six weeks. You may not see the full effect of conventional radiation therapy for 10 or more years after treatment.
- Stereotactic radiosurgery. Stereotactic radiosurgery uses 3D imaging to deliver a high dose of radiation to the tumor cells, while limiting the amount of radiation to normal surrounding tissues. It can usually be delivered in a single dose. This type of radiation may bring GH levels back to normal within five to 10 years.
Preparing for your appointment
You'll probably first see your family doctor or a general doctor. However, in some cases, you may be referred immediately to a doctor who specializes in hormonal disorders (endocrinologist).
It's good to prepare for your appointment. Here's some information to help you get ready for your appointment and to know what to expect from your doctor.
What you can do
- Be aware of any pre-appointment restrictions. When you make the appointment, ask if there's anything you need to do to prepare for diagnostic tests.
- Write down the symptoms you're experiencing. Keep track of anything causing you discomfort or concern, such as headaches, vision changes or discomfort in your hands, even if those things seem unrelated to the reason for which you scheduled the appointment.
- Write down key personal information, including any changes in your sex life or, for women, in your menstrual cycle.
- Make a list of all medications, vitamins and supplements you're taking.
- Take along old photographs that your doctor can use to compare against your appearance today. Your doctor will likely be interested in photos from 10 years ago through the present.
- Take along a family member or friend, if possible. The person who accompanies you may remember something that you miss or forget.
- Write down questions to ask your doctor.
Preparing a list of questions will help you make the most of your time with your doctor. For acromegaly, some basic questions to ask your doctor include:
- What's the most likely cause of my symptoms?
- Other than the most likely cause, what are possible causes for my symptoms or condition?
- What tests do I need?
- What treatments are available for this condition? Which approach do you recommend?
- How long will I need treatment before my symptoms improve?
- With treatment, will I go back to looking and feeling as I did before I developed symptoms of acromegaly?
- Will I have long-term complications from this condition?
- I have other health conditions. How can I best manage the conditions together?
- Should I see a specialist?
- Is there a generic alternative to the medicine you're prescribing?
- Are there brochures or other printed material I can take with me? What websites do you recommend?
Don't hesitate to ask any other questions you have.
What to expect from your doctor
Your doctor is likely to ask you a number of questions, including:
- What symptoms are you experiencing, and when did they appear?
- Have you noticed any changes in how you feel or how you look? Has your sex life changed? How are you sleeping? Do you have headaches or joint pain, or has your vision changed? Have you noticed excessive sweating?
- Does anything seem to improve or worsen your symptoms?
- How much would you say your features have changed over time? Do you have old pictures I can use for comparison?
- Do your old shoes and rings still fit? If not, how much has their fit changed over time?
- Have you had colon cancer screening?
Feb. 06, 2024